Grassmere Animal Hospital information
Greyhound Lab Work
HYPOTHYROIDISM
It is widely recognized that greyhounds normally have a lower thyroid level than other breeds. Any interpretation of seemingly low hormone levels must keep that in mind. There is some debate over how prevalent true hypothyroidism is within the breed and many feel it is over diagnosed. Here's why...
A study by Bloomberg at the University of Florida checked 221 greyhounds - both active racers and retired dogs - and found their normal T4's ranged from .5 - 3.6 with a mean of 1.47. That's about half the normal levels of other breeds and could lead to a normal grey with a T4 of .8 being diagnosed as hypothyroid.
What are the possible signs of a hypothyroid greyhound?
- dry dull brittle coat
- weight gain or weight loss
- exercise intolerance or low stamina
- sensitivity to the cold
- slow healing
- symmetrical hair loss
- "rat tail"
- temperament changes have been reported
Treating a hypothyroid Greyhound is also different than other breeds. If your greyhound is found to be truly low thyroid, the thyroid supplement is given at half the dose recommended for other breeds - greys get .1 mg per 20 pounds. An 80 pound Doberman would receive .8 mg Soloxine every 12 hrs while an 80 pound Greyhound would only receive .4 mg Soloxine every 12 hrs.
KIDNEY TESTS - CREATININE and BUN
Greyhounds have a higher creatinine than other breeds, and can be inadvertently misdiagnosed with kidney failure when, in fact, their kidneys are quite healthy.
Depending on the lab's normal range, other breeds have a high of about 1.2 to 1.4 for their creatinine level, Greyhounds can normally run up to 2.1 (some say to 2.4) before it's considered to be possibly abnormal. If there is any doubt, run a second test on the urine called a specific gravity to help distinguish true kidney failure from a normal value. A specific gravity in the 1.008 to 1.012 range combined with a truly elevated creatinine requires further testing. BUN's can also run a little above other breed's normal.
BLOOD COUNTS
| TEST | GREYHOUND | OTHER BREEDS |
Platelets | 80,000 to 200,000 | 150,000 to 400,000 |
| PCV | 50-65% | 37-55% |
| RBC | 7.4 to 9.0 million | 5.5 to 8.5 million |
| WBC | 3000 to 6500 | 6000 to 17000 |
| Total protein | 4.5 to 6.0 | 5.4 to 7.8 |
| Globulin | 2.1 to 3.2 | 2.8 to 4.2 |
A few things worth noting:
A platelet count of 100,000 or slightly less may be normal, but if this Greyhound hasn't been tested for the various tick diseases, it would be a good time to do that.
While a PCV of 45% is fine for other breeds, and will be noted as normal on all lab reports, remember that a PCV of 50% or less in an adult greyhound is too low and suggests an anemic Greyhound. Again, if the Greyhound hasn't been checked for tick diseases, have it done.
WBC's can run even lower than 3000 on an otherwise normal Greyhound, but low-end counts also warrant a tick check.
Separation Anxiety
WHAT IS IT?

Sometimes our pets love us too much - the fear of being separated from us becomes overwhelming. Some people believe it's because they feel responsible for our safety and when we are not in their sight, we might be in danger. Others believe it is the sadness of separation.
Whatever the underlying cause, dogs suffering from SA have a dramatic anxiety response usually within 30 minutes of the owner's departure. Dogs can cry, chew furniture, tear down blinds, urinate, defecate, self-mutilate, dig, and scratch at windows, doors and walls. They do this out of a sense of panic, NOT out of a conscious effort to punish the owner for leaving them.
Typical dogs suffering from SA display the panic with every departure - short or long. These are probably the dogs that follow you room to room around the house when you're home, and that watch you carefully as you prepare to leave. When you return, they are likely to greet you with an exaggerated excitement. Many of these dogs dislike being outside unless their owner is out with them.
WHY MY DOG?

Some of the predisposing causes of SA are thought to be:
- Spending time continuously with your dog, not leaving the pet alone for some time each day from the beginning of adoption.
- A reaction to an unsettling event such as boarding, rehoming, being lost.
- Changes in the family’s routine such as a change in work schedule, a move to a new home, or the addition of a new pet or person in the home.
- Behaviors by the owner that foster dependency - you must be alpha!
WHAT CAN I DO ABOUT IT?
Milder cases of SA often respond well to the techniques discussed below. Severe cases can take time and patience, and can be quite challenging. Remember each dog is an individual and you must try different things - some might work, others might not.
- Avoid eye contact or interaction with your dog for 30 minutes before leaving him and for the first 30 minutes after you return. Basically, that means IGNORE him. Even if he's jumping up, wagging hard, bumping you... IGNORE him. Pay no attention to him until he is calm, quiet and no longer trying to get your attention. If he's in a crate, let him out but ignore him.
- Analyze your own departure routine - gather keys, put on coat, check the kitchen, pick up purse, say something to your dog, walk out a specific door. Then perform these things in front of your dog without actually leaving. This sends confusing signals and will begin to defuse some of the building anxiety they feel as they watch your preparations. For example, pick up your keys and purse but then sit down. Leave the house through a different door. Certainly ignore your dog. Doing this over and over should relieve your dog of a lot of the initial apprehension.
- Stage very short departures (literally seconds long, in some cases) so you return before any anxiety is manifested. Walk out the door and immediately return. Continue to ignore your dog. Gradually - very slowly - extend the length of your absence as you see acceptance of your absence. If there are regressions, you have to shorten the departure time again. If you can leave for 30 minutes without signs of anxiety, you can usually then increase your departure time in longer increments. If you can get to 90 minutes without a panic, then you can very likely leave for any length of time.
- Safety cues or distractions are sometimes helpful. Don't use or do anything that has previously been associated with the anxiety behavior. Find something new. Leave an article of your clothing with your scent. Use a Kong filled with peanut butter. Turn on the radio or TV if you haven't been doing it. Never use your safety cue if you are going to leave beyond what you know is his tolerance limit at that time. You want it to be associated with safety and sense of wellness.
- In very severe cases, anti-anxiety medications can help a dog transition into accepting your absence. Check with your vet. These medications are not to be feared. If your dog's problem is not responding to the behavior modification techniques mentioned here, adding an anxiety-relieving medication may make a tremendous difference.
WHAT SHOULDN'T I DO ABOUT IT?
- Never punish your dog for SA behavior. This is not a behavior he is doing freely. It is a real panic attack.
- Don't impulsively adopt another pet. It may or may not help, depending on the origin of your dog's problem. If the problem is loneliness, it might. If it's true SA, it probably won't help.
- The effect of crating is different with different dogs. SA behaviors can certainly occur in a crate. If your dog is crated and has SA, you can try not crating him. And vice versa.
- Obedience classes will not address the underlying problem. Obedience classes can be fun and are almost always good to do, but don't expect it to resolve SA.
SOME FINAL THOUGHTS
Most dogs can be helped through this issue. If you persevere, you will probably make significant progress. If you get discouraged, you can also seek professional help. I recommend the Appalachian Veterinary Specialists practice in Knoxville. Dr Shull and her associates are excellent and fully qualified to help both with SA and with other behavior issues such as aggression, noise phobias, obsessive/compulsive disorders, etc. You will need a simple referral from your veterinarian. There are only 37 veterinarians certified in animal behavior in the US, so we are fortunate indeed to have one so close. ![]()

| If you haven't already read it, a book worth reading (several times) is | The Dog Listener by Jan Fennell, available online through Amazon and other retailers. This insightful book guides you through a non-violent peaceful method of training and relating to your dogs, and the techniques described have been very helpful for many SA dogs.

| Also very helpful is another book called | Leader of the Pack by Nancy Baer and Steve Duno. Again, the emphasis is on understanding why dogs behave the way they do and what behaviors WE do that send the wrong signals to our pets resulting in dominance issues, SA, barking, etc. This book is available through Grassmere Animal Hospital, as well as on line.
Osteosarcoma (Bone Cancer)
There is no more dreaded diagnosis for a Greyhound owner than this. Everyone knows someone who has lost a Greyhound to osteosarcoma. It's not the purpose of this section to replace an honest discussion with your veterinarian about the disease and treatment options. Information changes quickly in the field of oncology, and we all hope that there will be better treatment options in the future.
WHAT IS IT?
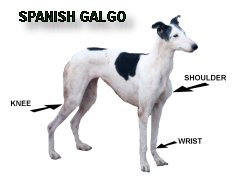
Bone cancer can strike relatively young dogs, even as young as 5 years.
While it can affect any bone in the body, 75% to 85% of these cancers are found on the legs at the shoulder, wrist or knee joints as shown in the illustration.
The disease begins inside the bone, initially causing an intermittent lameness but eventually causing constant, deep and severe pain after just a short period (1-3 months, most likely). The bone weakens and can eventually break with minimal trauma or pressure (a "pathological" fracture).
The following x-rays illustrate the bone changes caused by osteosarcoma (click for enlargement):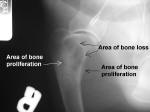
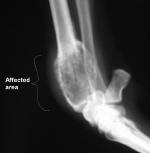
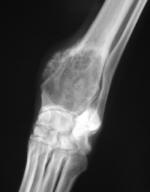
HOW IS IT DIAGNOSED?
If your Greyhound has a persistent lameness and the physical exam shows bone pain, your vet will very likely recommend an x-ray to distinguish the different causes. Depending on the stage of the osteosarcoma, the x-ray itself can be diagnostic. Early cases may be more ambiguous and require a follow-up x-ray in a few weeks.
If there is doubt, the definitive diagnosis can usually be obtained through bone biopsy.
Other diseases causing similar changes on an x-ray include some bone infections, other types of bone tumors, and fungal infections of the bone.
CAN IT BE TREATED?
Osteosarcoma is a terrible disease and managing it requires a strong commitment, both financially and emotionally.
Treatment addresses two aspects of the disease: the pain and the cancer itself. You must commit to aggressive pain relief for the remainder of your Greyhound's life. The pain of bone cancer is thought to be greater than almost any other disease, and it is continuous, non-stop, relentless, and never-ending. Even the strongest pain medications can fail to control this kind of pain, so it is imperative that you and your vet aggressively manage this part of the disease. Together, you must recognize when pain is no longer controlled, so you can make an appropriate quality-of-life decision.
TREATMENT OPTIONS
- Medical pain relief only - combinations of pain medications to control pain, followed by euthanasia when they fail to do so. The caution here is the difficulty in objectively judging pain. It's hard to know how much our pets are really suffering, and it's easy to think because they don't scream, they don't hurt. MOST DOGS SUFFER SEVERE PAIN IN SILENCE. With this treatment option, life expectancy is 4 months, although pain control may well fail long before that. You must find the courage to face appropriate timing of euthanasia.
- Amputation and pain relief - while seemingly drastic, amputation provides pain relief to 100% of the dogs who receive it. With amputation alone, the life expectancy remains at an average of 4 months, but the quality of life is improved.
- Amputation and chemotherapy - this improves the life expectancy, although does not cure the disease. With this the average life expectancy is 1 year.
- Limb sparing surgery - a new technique adapted from human medicine and done at some referral centers. The cancerous bone is removed and replace with grafted bone, and the nearest joint is fused. This is only done on the wrist area at this time.
- Radiotherapy to control pain - the tumor is irradiated and this can provide about 4 months of pain relief in about 65% of the patients.
- Euthanasia - eventually it is likely that treatment will fail, the pain will overcome your Greyhound again, and the cancer will prevail. When that day comes, the final gift you can give your pet is to relieve him/her of an impossible struggle. Euthanasia is the beginning of your grief, but it is the end of their suffering, and with this disease it is something that must be faced.
THE FUTURE
Studies are underway to try to understand and treat this disease more effectively. One aspect of this is a genetic study being done at the University of Michigan. If your Greyhound develops osteosarcoma, please consider the donation a small blood sample to this study. We need all the information we can get to eventually be able to cure these cancer victims. Dr. Macherey has further information on this.
Tick Diseases
This is an extensive topic of great importance to Greyhound adopters. The limited space here will serve as a summary of tick disease issues and hopefully a guide for you to pursue further information.
WHAT ARE THEY?
These are a group of diseases caused by microorganisms transmitted by an attached tick. Racing Greyhounds seem to be disproportionately over represented among groups of exposed dogs. Tick disease infection can occur in utero (during fetal development), during their puppyhood or training, or during their active racing careers. In our testing, approximately 30% of the retired racers tested are testing positive for exposure to one or more of the tick diseases.
The diseases most commonly seen are Babesia canis, Ehrlichia canis, and Borrelia burgdorferi (Lyme). Other diseases sometimes found include Ehrlichia equi, Ehrlichia risticii, Rickettsia rickettsii (Rocky Mountain Spotted Fever), and Bartonella spp.
SYMPTOMS
Each tick disease does tend to have its most likely associated symptoms, but there can also be much overlap in the symptoms of different tick diseases. Individually, your dog may have an atypical case, or one of the less common organisms, so the most common signs of tick disease in general are listed as a group here.
- Low platelet count (remember the Greyhound normal is lower than other breeds, but if your hound's is below 100,000 consider tick testing if it hasn't been done) resulting in possible nose bleeds, bruising, and any other sign of bleeding.
- Low (or high) white blood cell count
- Anemia
- Neck pain
- Seizures
- Fever
- Weight loss
- Lethargy
- Stiff gait
- Enlarged liver or spleen
- Enlarged lymph nodes
TESTING
The reason for testing sick dogs is obvious, but why screen apparently healthy Greyhounds? The reason is that all but Rocky Mountain Spotted Fever can remain dormant in a dog's body, sometimes for years, before causing significant signs of illness. By testing, you are trying to discover a potential problem in the future.
If a dog has an active TBD (tick borne disease), it is very likely that there will be measurable changes in their CBC (complete blood count). A normal CBC suggests of an absence of active disease. If the CBC shows anemia, a depressed platelet count, or a low white cell count, the patient could be infected and further testing is warranted.
There are two common methods of testing:
ANTIBODY DETECTION - by submitting serum for this test, your vet is looking for signs of past or current exposure to one of these diseases. The confusion in interpretation of the resulting antibodies titers rests with the difficulty of distinguishing between a current active infection, a dormant infection, or simply the memory of a past cured infection. Many Greyhounds are tested by Protatek labs in Arizona, although Antech and other labs also perform this testing.
PCR TESTING - considered to be the gold standard for testing because it actually detects the DNA of the organism. A positive test indicates current infection 99.99% of the time. A negative test, however, doesn't completely rule out a dormant infection since the sample submitted for testing is blood and the organism may be present in other tissues, but not in the blood. PCR testing is not valid for Lyme's disease for that same reason - the organism is never found in the blood. Both PCR and serology (antibody) testing is performed at the North Carolina State Tick Borne Diagnostic Laboratory.
TREATMENT
When and how to treat these diseases is a controversial subject. Again, you must be informed about the tick disease(s) found in your dog, and discuss with your veterinarian whether your dog needs to be treated. Many veterinarians are reluctant to treat a seemingly healthy dog aggressively, while others recognize the potential for future problems and might treat an asymptomatic dog. Stay involved in the care of your Greyhound.
We follow this protocol for our antibody positive Greyhounds:
Ehrlichia titers - all positive titers are treated doxycycline. If doxycycline isn't tolerated, Imizol (imidocarb) can be tried but its effectiveness is unclear.
Babesia canis titers above 1:160 are treated with 2 injections of Imizol given 2 weeks apart.
Borrelia (Lyme) - all titers are treated with doxycycline. If doxycycline isn't tolerated, Amoxicillin is given.
Bartonella spp - Doxycycline or Azithromycin can be used.
Rocky Mountain Spotted Fever - only symptomatic dogs are tested and treated. This is the one tick disease that does not lay dormant, so a positive antibody titer on a healthy dog only indicates past infection.
Again, the decision to treat, and what protocol to use, is one you must make with your own veterinarian.
A word about doxycycline - The traditional dose of doxycycline is much lower than what is now used by many veterinarians who treat tick diseases on a regular basis. We are now dosing doxycycline at 10 mg/pound divided into 2-3 doses over the day for 6-8 weeks. That means that a 60 pound dog gets 600 mg each day, divided either as 300 mg twice a day or 200 mg three times a day. This is double what the traditional dosing has been. Only you and your vet can decide what dosing is appropriate for your dog, but consulting with a veterinarian who is familiar with treating tick diseases would be wise.
Doxycycline must be given with food to try to avoid a stomach upset.
Happy Tail / Comedones / Bald Thighs

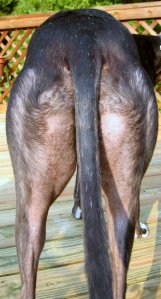
It's very common to see Greyhounds with shiny skin on the back of their thighs, and little or no hair growing there - bald thighs. The exact cause of this is unknown, and it is considered to be largely a cosmetic "problem" perhaps in the same category as pattern baldness in people. It is NOT linked to hypothyroidism and your Greyhound should not be supplemented with thyroid medicine on the basis of their hairless thighs alone.
As an aside, many Greyhound gatherings have "Shiney Hiney" or "Bald Butt" contests! If your Greyhound can't seem to grow hair back there, you may win a blue ribbon!


Another "Greyhound thing" is the incidence of comedones or black heads found on their lower chest. Again, this is usually a cosmetic concern more than a real medical problem, but it can be very unsightly.
Milder cases may resolve spontaneously once the Greyhound is adopted into a home.
The affected area can also be gently rubbed with non-prescription witch hazel or with raw virgin coconut oil. Repeat every day or two until the area clears.
More stubborn and advanced cases of comedones can be treated with a benzoyl peroxide gel or a deep cleaning medicated shampoo likeSulfoxydex, both available through your veterinarian.
Also, Renova (a human prescription cream) can be applied nightly to the chest for 3-4 weeks. In a few cases, these areas can become infected and will require antibiotics.

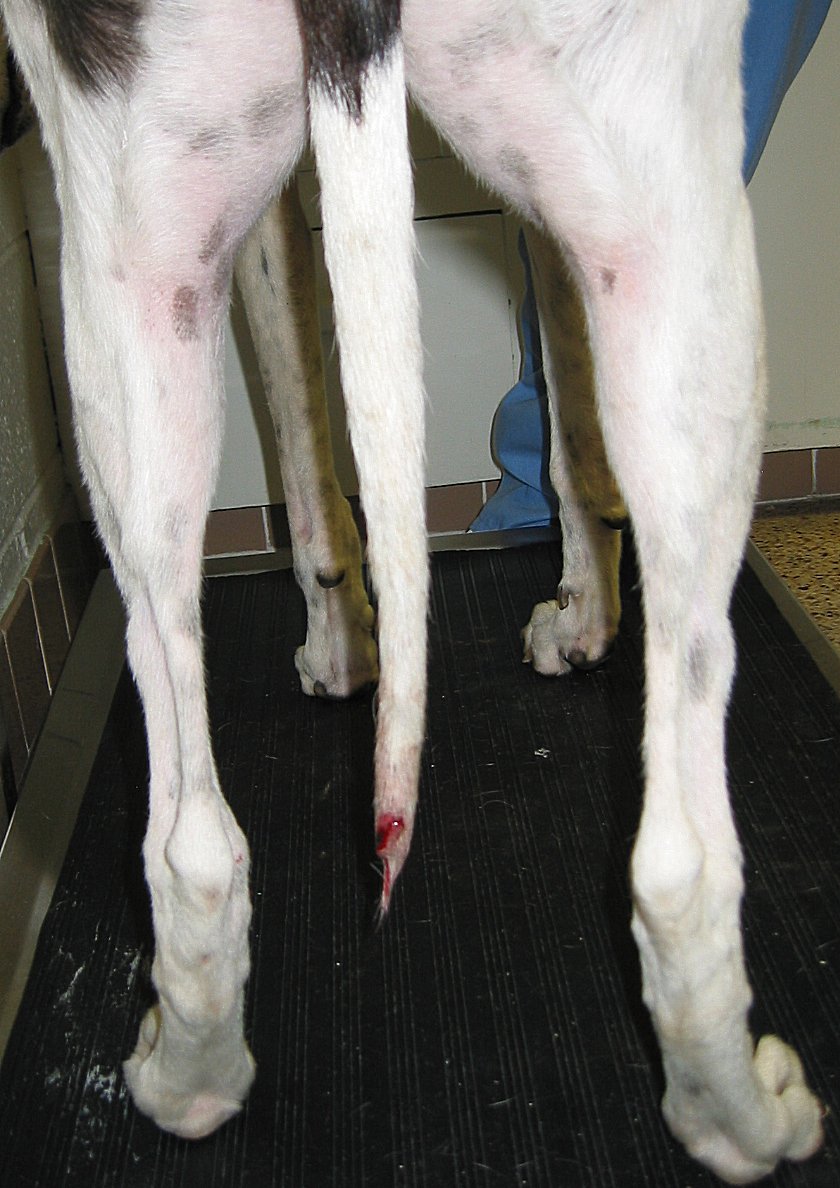
One of the admirable features of our Greyhounds is their long delicate tail. Another is their happy disposition and joyful wagging when they're happy. Unfortunately, when you put the two things together, you can have a minor disaster in just a few minutes. It's called "happy tail".
The skin on greyhounds is thinner than other dog breeds and is more prone to tears and cuts. When they wag their tail very hard against something hard (a wall, door, cabinet), they can easily break the skin and begin to bleed. Even a small wound can bleed enough to make your home look like a crime scene!
If that happens, you'll have two problems: treat the tail and clean up your house. Neither one is a small matter.
TREAT THE TAIL
- Keep the tail from further injury by getting your grey away from hard surfaces
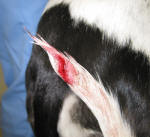
- Get a softly padded bandage on the tail to both protect it and to keep it from bleeding everywhere. Place a non-stick pad over the wound (don't try to clean it if it's still bleeding - just get it covered) and cover it with a good layer of soft cotton, a sanitary napkin, or many layers of soft roll gauze. KEEP THE BANDAGE LIGHTWEIGHT so it has a better chance of staying on. Cover your padding material with soft adhesive tape with some contact with the hair. If the bandage is too heavy, they wag it off (think about how far you can throw a feather vs. a rock!!)
- See your vet as soon as possible. No wound will heal well if it's infected so antibiotics will probably be prescribed. This is rarely an emergency, although the amount of blood will make you think it is. A trip to the emergency clinic is rarely needed if you can get the end of the tail bandaged.
- If there's a delay seeing the vet (weekend, holiday, etc) remove your first bandage after 6-8 hours. By then the bleeding should have stopped and you can assess the damage. If the wound is small, I prefer not to clip the hair away as the hair actually offers some protection against further trauma as it's healing. If the wound is large, the hair must be clipped.

- Keep the tail bandaged for at least 2 weeks - much longer if the wound is large.
- In the worst cases, the wound may be severe enough that the end of the tail will need to be amputated.
TREAT THE HOUSE
There are several good cleaners that will remove blood. Always test on delicate fabrics first. One of the best I've found is hydrogen peroxide and most of us have it at home already.
EPILOGUE
Once this has happened to you, you'll never let your hound wag against anything hard again. If this hasn't happened to you yet, please take every precaution to keep that long delicate tail from hitting hard surfaces. It's really hard to imagine how bad a happy tail incident can be.
Trancing / Nitting / Grinning
Trancing
(not a seizure)

One Greyhound behavior that deserves mention in their medical information is "trancing". Some greys seem to go into a trance when they brush their back against low hanging branches or bushes. They may actually stand motionless for several minutes with their eyes glazed over as they seem to be feeling the touch of the branches.
This odd behavior has caused some concern to adopters who think it might be a seizure. It is not a seizure! It's not even unique to Greyhounds - other breeds reported to do this include the Bull Terrier and Basset Hound. They can be roused be a gentle nudge, and it seems to be harmless trait.
Above is Julie Fitzpatrick's "Honey" trancing in their Christmas tree and to the right is Deb Lipartito's boy "Reo" trancing in some tall grass.
Nitting
(not aggressive biting)
Another behavior trait of some Greyhounds is called "nitting". When a Greyhound is very happy, and loves their "person" they may nibble at their arm or side (or any available skin) with their front teeth. It's actually an expression of great happiness but it might be misinterpreted as aggression. The nibble is hard enough to easily leave a bruise, so, although it's actually meant as a true compliment, it's wise to be careful.
A variant of this is chattering and air snapping. When some greys are happy, they may chatter quite loudly, clicking their lower jaw as though they were cold. You may see a greyhound do this at meal time or when their "person" comes home. Air snapping is similar to nitting but instead of nibbling at your skin, they snap at the air. Again, this could easily be misinterpreted as aggression when it's not. The "snapping" is not aimed at you - it's aimed at the air.
Your adoption group should be able to tell you whether the greyhound you're adopting does any of these things.
Grinning
(not snarling)
Finally, there's "grinning", a facial expression shared with other breeds but also frequently misinterpreted. Grinning is usually a submissive expression although it looks very much like a snarl. The clue is in the rest of the Greyhound's body language and the circumstances that you see this. The right and left pictures below were taken after an exciting run and this greyhound - Rin - was really excited and happy! The middle picture, Fandango, was also simply an excited, happy fella!
Again, your adoption group should know whether your greyhound is likely to do these things. Sometimes, however, these traits don't appear til the greyhound has been in their new home long enough to be settled and relaxed.




Individually, any dog or cat can show an intolerance to any product, so when you try a new product it is always wise to observe your pet afterwards for any signs of a problem. If your individual Greyhound seems intolerant of something, look for a substitute.
Remember to weigh the brief annoyance of an odor, itch, or slight redness from a topical treatment against the long-term problems from a flea or tick infestation.
FLEA AND TICK PRODUCTS WE CARRY AND CAN RECOMMEND FOR YOUR GREYHOUND
- Advantage® - gives very good topical flea control
- Front Line's Top Spot® is commonly used on Greyhounds for both flea and tick control with topical drops
- Advantix® - a somewhat controversial flea/tick product but one that has been used very successful in many many Greyhounds. It contains permethrin, so is best not used around cats.
- Revolution® - another topical product that combines heartworm, flea, and some tick control, but may seem slow to work
- Sentinel® is an oral medication that combines excellent heartworm and intestinal worm protection with luferon, an ingredient that prevents flea eggs and larvae from developing.
- Preventic® collars are a tick-collar (does NOT kill fleas) that can be used on Greyhounds.
- Advantage Multi® - combines Advantage with another chemical to provide protection against heartworms, fleas, roundworms, hookworms, and whipworms with a monthly topical application. It does not treat for ticks.
HEARTWORM PRODUCTS FOR YOUR GREYHOUND - We strongly recommend year-round heartworm protection for your Greyhound
- Interceptor® - a monthly oral chewable tablet that also protects against hookworms, roundworms, and whipworms
- Sentinel® - same as Interceptor, but with luferon added for some flea protection
- Revolution® - a topical monthly heartworm preventative
- Heartguard® - another safe monthly heartworm preventative
- Advantage Multi® - a new topical monthly preventative with added protection against fleas and intestinal worms
Thunderstorm Phobia
| Most dogs seem to tolerate storms, but others show obvious | signs of anxiety:
| panting |
| pacing |
| hiding |
| drooling |
| shaking |
| house soiling |
| escape behavior - running into glass doors, over fences |

SOME TREATMENT OPTIONS
Xanax® (alprazolam) - this is a true anti-anxiety medication and is generally safe to give to most dogs including greyhounds. It can be given at a low dose over a long period of time, or at a higher dose for a brief period. It is only available through your veterinarian. It is the most effective drug I've seen for storms. Unfortunately, even that doesn't help all dogs.
Clomicalm® (clomipramine) - another prescription medication that can be used long term for the entire season. This is also prescribed for separation anxiety and some obsessive compulsive disorders.
Benadryl® (diphenhydramine) - this is an over-the-counter antihistamine that causes drowsiness. It's not an anti-anxiety drug, but with milder problems it may allow your dog to sleep through the storm. It can be dosed at 1-2 mg per pound. Adjust the dose down if it makes your dog too sleepy.
Acepromazine - this is the old time veterinary remedy. It's a tranquilizer and causes immobilization or mild sedation. There is no anti-anxiety component to the drug - it simply keeps the dogs quiet. Mentally, they probably still are aware of the storm. It's helpful with some, and has been used also with separation anxiety.
Melatonin - this is another natural medication that may be a bit more effective in some dogs that Rescue Remedy. It can be dosed at 1.5 mg per dose for dogs under 30 pounds, and 3 mg per dose for dogs over 30 pounds. Repeat, if needed, 2-3 times a day. I would not recommend continuous dosing for weeks at a time, but during a stormy day or two, you can do it for the duration. Again, it may not be enough for the severe thunder-phobe. It can be purchased in the vitamin/herbal section of drug stores and grocery stores.
Rescue Remedy - a Bach Flower homeopathic remedy - this is a mild, anti-anxiety, natural medication that is given either directly in the mouth or in the drinking water. It can also be used for separation anxiety, traveling, company coming, etc. In my experience, it may help mild anxieties, but if you have a dog in full blown thunder phobia, it will probably not be enough by itself. In Nashville, it can be purchased at Wild Oats, and always on line. The dose is 1 drop per 5 pounds up to 20 pounds. Above 20 pounds, add 1 drop per 10 pounds. Thus, a 70 pound dog would get 9 drops. Put it directly in the mouth, wait 10 minutes and repeat if necessary.
Desensitization to the sound - you'll hear about buying a recording of a storm and playing it at gradually increasing volume to try to desensitize the dog to the sound. Well, I have yet to see it succeed, but if you do it, let me know what you think. Very time consuming. In theory, a good idea.
Anxiety wrap - This coat provides light and comforting pressure. Here is a link to one of many on-line resources offering the coat: Anxiety Wrap Coat
Storm Defender Cape - this sounds like voodoo but the success with this is reported to be pretty good. It's a custom made dog coat made of material to block the static associated with an electrical storm. The theory is that dogs feel the static in a storm before the storm even arrives, and that sensation severely heightens their fear. You put the coat on before the storm and many dogs remain calm during the storm. You can read more about it from the link. Many happy customers.
Dryer sheet - along the same line of thinking re the static electricity, you can rub your dog down with a dryer sheet to remove some of the static from their coat.


Safe havens - some dogs just need a safe place to hide. If they are there, they feel safe. It may be a closet, under the bed, in a tub, in a crate, wherever. It may make you uncomfortable to see your dog hiding like that, but if it gives him a sense of security to be there, you should let him stay.
Your own behavior - this is hard. We hate to see our much loved pets so terrified. It's instinctive to cuddle them, pet them, reassure them with sweet talk. Don't do that! There is very strong belief that you are actually reinforcing the behavior when you do that. You should be calm, reassuring only in your demeanor, go about your normal routine. If you "reward" your dog with extra attention, you may actually be training him to keep doing it. I know it's a very hard idea to accept, but try it!
Greyhound Anesthesia
Most Greyhound owners are aware that Greyhounds can have some special anesthetic issues, but fear of anesthesia should never prevent you from seeking proper care for your hound. There have been remarkable advances in anesthetic safety and, while we can never guarantee the outcome of an anesthetic procedure, the anesthetics available today are generally much safer than most we have had in the past.

Prior to anesthesia, your vet may recommend any or all of these precautionary procedures:
- Screening lab work - to detect hidden underlying problems that might complicate anesthesia, or guide which anesthetic would be used.
- Chest x-ray - for the delicate seniors or those with abnormalities related to the chest.
- IV catheter and perioperative fluids - this maintains normal blood pressure and normal perfusion to vital organs like the kidneys during anesthesia, and it also provides an immediate portal for drugs in case of an emergency.
- Home medications - your vet may have you begin antibiotics or pain medication at home before the actual anesthetic procedure.
It is important to understand that there is no single safe anesthetic protocol for Greyhounds.
With many agents to chose from, the safest anesthetic is the one your vet is comfortable using. Here are some examples of drugs and comments:
BARBITURATES - NEVER use a thiobarbiturate anesthetic in a Greyhound. They are far less common these days, but still available. NEVER EVER use this category of anesthetic on a sighthound.
PRE-ANESTHETIC MEDICATIONS - these drugs are used shortly before the actual anesthetic is administered to provide some early pain relief and a calming light sedation. Often, a combination of medications are given. By using these drugs, a lower dose of anesthetic agent can be used, and that makes the whole process safer. Examples of acceptable pre-anesthetics for Greyhounds are:
- Acepromazine (we dose significantly lower than other breeds - 50% or less)
- Butorphanol (Torbugesic) (we dose at 75-80% normal amount)
- Buprenorphine
- Medetomidine
- Morphine
- Glycopyrollate
- Atropine

- Telazol (we dose at 75-80% normal amount)
- Ketamine/Valium
- Propofol
- Isoflurane
- Sevoflurane
MALIGNANT HYPERTHERMIA
A rare complication of anesthesia in Greyhounds is an emergency condition called malignant hyperthermia. With MH, their body temperature rises very rapidly immediately after an anesthetic. Temperatures above 106.0 can occur and, unless caught and treated, can lead to death within 90 minutes. This condition is thought to be genetically predisposed so if you know of littermates who have experienced it, extra precautions should be taken with your hound. The anesthetic agents often mentioned (but not the only ones) with the onset of this syndrome are succinylcholine and halothane.
Should this syndrome begin, every effort must be made to cool the Greyhound. A drug called Dantrolene is best to treat the emergency. Great caution should be taken with any future anesthetic procedure with a MH Greyhound.
MUSCLE FASCICULATIONS - As they awaken, some Greyhounds experience marked muscle "fasciculations" (tremors). Because of their powerful muscles and large muscle mass, these fasciculations can also cause a temperature rise. This temperature spike is much more easily controlled than MH, and can be mistaken for MH when it isn't.
Cauda Equina Syndrome
This orthopedic problem can mimic other hip and rear-end diseases, but it is unquestionable a prevalent disease in its own right among greyhounds. It's not just a Greyhound problem, though, as it is found in many other large-breed, athletic dogs. Afflicted dogs can begin showing signs as young as 5 years or less but, as the disease progresses, veterinarians are often presented with a wobbly and weak aging greyhound.
WHAT IS CAUDA EQUINA?
This disease goes by several names - cauda equina, lumbosacral instability, lumbosacral stenosis. It's a compression of the nerves in the spinal canal near the hip. This can be from arthritic changes, disc rupture, or tumor. When nerves are pinched you feel pain, numbness, or a stimulation, and the range of possible signs with CES (cauda equina syndrome) come from one of these effects.
Here are some remarkable pictures to illustrate what happens. These are MRI's of a 7 year old Labrador Retriever named Trapper. Trapper lived in Alaska, and was diagnosed with CES, and treated surgically at the Washington State Veterinary Teaching Hospital. Many MANY thanks to Bob Shem for sharing these images. They clearly show the compression of the nerves:
This is a side view of Trapper's spine. In this image, Trapper's legs are in their normal standing position. You can clearly see the marked compression of his nerves.
1 = pinching or compression of the spinal nerves
2 = healthy spinal discs of the lumbar vertebrae
3 = collapsed disc space between the last lumbar and first sacral vertebrae (the lumbosacral junction). Note the rounded bony arthritic bridging that has developed under the joint
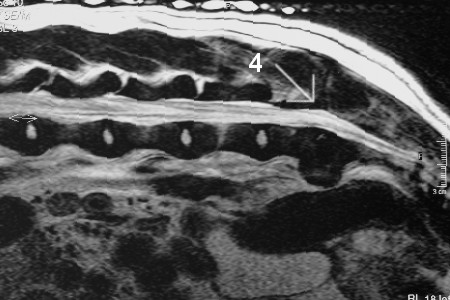
In this image, Trapper's legs are drawn forward, changing the position of the vertebrae and opening up the spinal canal, relieving the pinching (#4). This is the inherent "instability" that defines this problem. The movement leads to pressure on nerves.
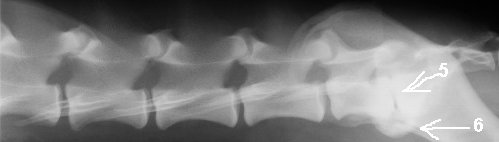
This is how this same area would look on a simple x-ray. The nerves are not visible, and the only visible sign of a problem is the collapse of the LS disc space (# 5) and the visible bone proliferation beneath the LS space (# 6).
SYMPTOMS
AN AFFECTED DOG WILL PROBABLY NOT DISPLAY ALL THESE SIGNS.
DO NOT RULE OUT CAUDA EQUINA BECAUSE YOUR DOG ISN'T DOING ALL THESE THINGS.
- Sharp pain - remember dogs don't cry out with every pain, especially chronic pain that develops slowly and they can adjust to it. DON'T EXPECT THEM TO CRY OUT CONSTANTLY!!!
- Slow to rise - again, related to pain
- Changes in posture and gait - how they place their rear legs or stand or their posture laying down
- Unwillingness to exercise, or significant discomfort after exercise
- Unwillingness to use stairs, or noticeable change in speed and skill using stairs
- Poor coordination
- Shuffling gait
- Weakness in the back end
- Urinary or fecal incontinence
- Chewing at feet or tail
- Less tail movement
- Worn rear nails due to dragging the paws
- Intermittent lameness
- Partial rear-end paralysis (paresis)
- Complete rear-end paralysis
DIAGNOSIS
This is a surprisingly difficult disease to prove. Frequently mistaken for hip dysplasia, the nerve injury is not visible on plain x-rays and to be able to "see" the problem, the patient must submit to a myelogram, epidurogram, or if feasible, a CT or MRI (as illustrated above).
It is possible to make a presumptive diagnosis of CES based just on a physical exam. Dogs with cauda equina are very sensitive over the LS area. Your veterinarian may test your dog by applying targeted pressure to the affected LS area. Also, many dogs with CES are very uncomfortable when their tail is lifted or hyperextended. A careful patient history, a good physical exam, and probably plain x-rays to rule out other problems are likely to be suggested.
Remember, if your dog tests "positive" to the exam described above, we must also consider other diseases that cause pain or nerve compression - spinal tumors, prostatic disease, bone infection, etc - in the differentials.
TREATMENT
- Avoid strenuous exercise, or even lighter exercise if it causes your dog visible discomfort afterwards.
- Oral NSAID's like Rimadyl®, Deramaxx®, and Metacam®, and oral steroids, sometimes provide some relief, but it may be minimal depending on the level of pain.
- Tramadol (Ultram) can be a helpful analgesic.
- An injection of 20 mg DepoMedrol® on either side of the LS midline can be very helpful to affected dogs. Here is a diagram to illustrate the location:

- Surgery to remove herniated disc material and open the compressed areas can be attempted. Results vary with the individual case and should only be done by a surgeon experienced in this area.
PROGNOSIS
This is a progressive and debilitating disease, and one that can become a legitimate cause for euthanasia if the terrible pain and disability cannot be relieved.
The speed and extent of progression will vary from dog to dog. Some may never develop symptoms severe enough that their owner must make major treatment decisions. Many dogs, however, face a difficult future and if this happens to yours, you must discuss your options with your veterinarian, based on your individual dog's symptoms, age, and general health.
Some dogs have made a complete recovery with surgery. Others recover briefly and then relapse. Some do well with the DepoMedrol® injections. Whatever you decide, you must be fully informed about this disease and its effects on your dog.
SLO Symmetrical Lupoid Onychodystrophy
Imagine one day your Greyhound limps a bit and you look at his paw to find that an entire toe nail is missing. Your first thought is likely that he ran too hard and caught it, and in some cases, that really is all that happened. Sometimes, though, if you look at the remaining nails, you'll discover a bigger problem. There may be several toe nails that seem abnormal - loose, tender, draining.
SLO is thought to be an autoimmune disease that targets the toe nails. The hallmark of autoimmune diseases is that the body mistakenly forms antibodies against part of itself. If it's antibodies against our our red blood cells then we destroy our own blood and become anemic. If it's antibodies against our joints then we become arthritic. In the case of symmetrical lupoid onychodystrophy, Greyhounds form antibodies against their toe nails, and reject them.
WHAT ARE THE SIGNS?
- multiple nail loss
- licking the nails
- visible oozing around the base of the nail
- separation of the nail from the quick
- limping
- infection
- odor
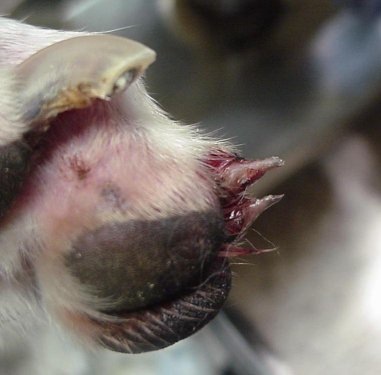
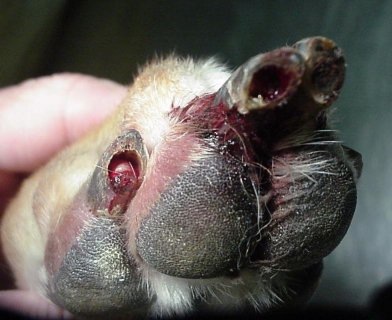


DIAGNOSIS
While the only 100% accurate way to diagnose this problem is by biopsy (and that means amputating the end of the toe, called "P3"), this problem in a Greyhound is one that experienced veterinarians will feel comfortable making a diagnosis based on the appearance of the feet. Amputation of the tip of a toe is disfiguring, expensive, and unnecessary.
This condition can be confused with simple bacterial infection and fungal infections, and valuable time may be lost with antibiotics, foot soaks, and other medications that don't target the underlying immune nature to the problem.
TREATMENT
- this must be treated as an immune disorder, not a simple infection
- loose and painful nails should be removed - usually under anesthesia
- there is often a 6-10 week lag time to see a good response to treatment
- treatment must extend over a period of at least many months, and in many cases, years
- relapses are common
- medications may need to be adjusted based on response to treatment - there is no single successful protocol
- SEE YOUR VETERINARIAN but go in with information about the disease and treatment. This is not a common diagnosis and many vets might not be familiar with it.
MEDICATIONS (any doses mentioned here are for greyhounds - other breeds need their own levels)
- in all cases, essential fatty acids should be started immediately but because of the nature of the disease, it may be 6 weeks or longer to see improvement. The recommended dose is 180 mg eicosapentanoic acid (EPA) per 10 pounds. Sources of EPA are:
- The 1000 mg fish oil capsules contain 180 mg EPA, so a 60 pound Greyhound should get 6 fish oil capsules a day, a 70 pound Greyhound should get 7. These are readily available over-the-counter.
- 3V HP caps
- Derm Caps ES
- Vitamin E 400 IU every 12 hrs
- if the problem is severe or advanced at diagnosis, the following medications are also used:
- tetracycline and niacinamide (500 mg each every 8 hours for an average sized Greyhound)
- pentoxiphylline (Trental) - some vets prefer this over the tetracycline/niacinamide combination
- prednisone and azathioprine should be avoided if possible, but in resistant or very aggressive onset cases, prednisone can be dosed in greyhounds at 15 mg total dose per day, and then weaned down as soon as possible.
- Pain medication - this is a very painful condition and there can be some relief with NSAID's like Rimadyl, Deramaxx, etc.
A WORD ABOUT DIET
Most dermatologists agree that one of the possible triggers for this disease is food related. Thus, treating your SLO dog as a severe food allergy patient might be of some benefit. This involves very strict dietary restrictions, and the details should be discussed with your vet. Foods that have proven useful include Eukanuba Veterinary Diet (Response FP - a fish based food), IVD foods, Hill's ZD, and other truly hypoallergenic foods.
PROGNOSIS
This disease tends to remain a life-long problem with afflicted dogs, but it is also one that can almost always be controlled with medication. With luck, over 6-8 months, new nails will regrow and your hound will be pain-free.
Corns
WHAT ARE THEY?
(click pictures for enlargement)


|
A Greyhound may have 1 or more corns, and they may vary in size and exact location on the pads.
They all share the generally circular appearance, the hard core, and they are consistently painful at least to some extent.
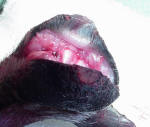
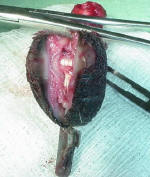
|
As these pictures show, corns extend deep into the pad. It's easy to see why walking becomes so very painful for the "corn dogs". Affected Greyhounds seek soft surfaces for walking - grass and carpet - rather than hard pavement or flooring.
Any lameness examination on a Greyhound MUST include
an examination of each pad for the presence of a corn.
WHAT CAUSES THEM?
The exact cause remains uncertain and that discussion will be left to others. It does seem to be an almost exclusive Greyhound affliction. One non-Greyhound (perhaps a lurcher?) did present to our hospital with a true corn:

HOW CAN THEY BE TREATED?
- Flatten the corn
By rasping, Dremeling, or filing the corn flat, the painful pressure on the inside of the pad is relieved. The corn will reform and, as the pressure mounts, and the pain will return. This does provide temporary relief, however. Some corns will need to be flattened as often as every few weeks but this is something most Greyhound owners can learn to do at home.
- Soften the corn - apply any of the keratolytic agents like KeraSolv or human corn softener.
- Cushion the corn
Specially made Therapaw Boots have proven to be extremely helpful to Greyhounds with corns. The cushioning sole protects the sensitive pads, especially while walking on pavement and sidewalks. These boots are different than other every-day protective boots. Follow the link to the right.
- Shell or hull out the corn -
This procedure should only be done by a veterinarian with the proper tools. It does allow for a deeper removal of the embedded corn, without resorting to surgery, and seems to give the Greyhound a longer period of relief than filing or dremeling. Again, the corn may return. For a more complete description of the procedure, click on the picture to the right or here.
- Surgery - A deeper more invasive removal can be attempted by scalpel or laser excision.
- Fat implants - Auburn university is implanting a fat pad in the digit to see if by providing better cushioning, it might prevent recurrence of the corns.
- Amputation - a last resort. While it removes the painful corn permanently, there is a real possibility that another corn will appear on another digit.
CAN THEY BE CURED?
Corns can resolve permanently, although in some cases, they seem to disappear only to return later. In other cases, they never regress but require regular maintenance to keep your Greyhound walking as painlessly as possible.
Pannus
WHAT IS IT?
This eye disease is also called chronic superficial keratitis. It's a chronic, immune-mediated disease that can affect both eyes, and if not treated, can cause blindness. The eyes develop areas of inflammation that can cover the corneas, blood vessels grow across the eye to the affected areas, and pigmentation may develop on the surface of the cornea.
WHAT CAUSES IT?
- Genetic factors - there are unquestionable breed predispositions (Greyhound, German Shepherd), so when there are breed predispositions, a genetic link is always suspected.
- UV light - sunlight is known to worsen the condition.
- Allergy - it is speculated that at least part of the disease may be an allergic reaction to foreign substances on the cornea or against the corneal tissue itself.
WHAT DOES IT LOOK LIKE?
Initially the eye(s) may look a little reddened. They may be sensitive, and the dog may rub them. As the disease progresses, there are clearly visible changes on the surface of the cornea, beginning at an edge and proliferating inward. 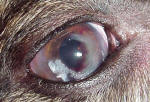




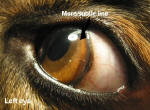
HOW IS IT TREATED?
- topical cortisone drops
- injections of cortisone under the outer surface of the eye
- topical 2% cyclosporine drops
- avoid sunlight. Try Doggles - doggie sunglasses that block 100% of the UV light - click the link below:

CAN IT BE CURED?
Unfortunately, not at this time. It's likely that your Greyhound will require medication of some sort for the rest of his or her life, although the frequency of medicating may vary seasonally. But the good news is that this disease can usually be controlled and in most cases there is no discomfort, and vision remains normal.
Seizures
WHAT IS A SEIZURE?
A seizure is an abnormal disturbance of brain function resulting in a change in physical actions and/or mental state. A seizure is thought of as a symptom of a disease, rather than a disease itself.
Typical seizures are
- relatively short, lasting between 1-3 minutes
- preceded by subtle or obvious behavior changes signaling the coming seizure
- followed by a recovery period lasting from a few minutes to many hours
CAUSES/TYPES OF SEIZURES
The classic seizure is a primary "epileptic" seizure. They have no known cause and they often begin at a relatively young age (under 5 years). Many or most are probably hereditary. Because there is no specific test for these "idiopathic" seizures, when other causes of seizures are eliminated, we then assume we are probably dealing with primary epilepsy.
Secondary seizures have specific and identifiable causes. These include, but are not limited to:
- brain tumors
- infectious disease
- blood sugar abnormalities
- thyroid imbalance
- liver disease
- heart disease
- trauma
- toxins
HEAD BOBBING IN GREYHOUNDS
Some adopters may see their Greyhound begin to "bob" their head up and down for no apparent reason. They remain fully conscious and respond to the owner, but the head trembling may continue for a few minutes. When it stops, they are perfectly normal again. This activity is very likely a minor seizure. Greyhounds who do this are not expected to progress to a worse form of seizure. The frequency of these episodes may vary greatly. You may be able to determine a cause or "trigger" but must be cautious not to jump to conclusions based on a single episode. These seizures should not require any treatment.
There are some tranquilizers or sedatives your veterinarian might use that could temporarily worsen the head bobbing, so if your greyhound does this be sure to inform your vet.
WHAT CAN BE DONE TO DIAGNOSE YOUR SEIZURING DOG?
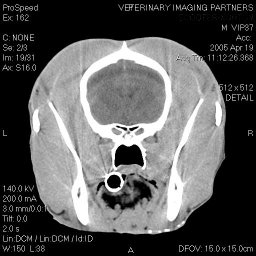
- thorough and accurate medical history
- complete examination to include a neurological exam
- serum chemistries
- urinalysis
- complete blood count
- tick disease panel to include Ehrlichia spp, Lyme's, and possibly Rocky Mountain Spotted Fever
- thyroid panel
- EEG, if available
- CT or MRI if the above testing hasn't identified a cause
SEIZURE THERAPY
The treatment plan for your pet must be made by your veterinarian based on your dog's history and test results. If a specific cause has been discovered then that problem must be addressed in the treatment plan. Not all seizures will need to be medicated with anticonvulsants, but many do. That decision must be tailored to your pet.
Drugs commonly used to treat seizures are Phenobarbital and potassium bromide. With both medications, there will be a period of adjustment during which your dog may seem groggy, wobbly, dull, weak. This is almost always temporary (lasting up to 3 weeks) and resolves as their body becomes adjusted to the medication.
Blood levels of both drugs can and should be monitored regularly to be sure the level is appropriate.
Hemangioma's
When you see a dark spot on your greyhound's skin, you may want to take a closer look. Dark "things" can be something serious, or they can be minor things that are more of a nuisance than anything else. One of the common things our greyhounds seem to grow easily is a hemangioma and, fortunately, these fall more into the nuisance category.
Appearance - smooth surface, red color, usually less than 1/4" across and often much smaller. (Click pictures for a full-size view)

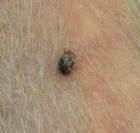

Location - especially common on the lower chest and abdomen, and the legs. They're usually seen in the areas with the least fur.
Significance - these are benign growths - not cancers. They will bleed if scratched.
Treatment - if they are clearly hemangioma's, these small growths require no further treatment. Some disappear on their own. Some remain for years.
What else could they be? There are other, more serious tumors that can be confused with hemangioma's so unless you're confident about it, your vet should be the one to make that distinction.
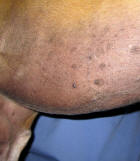
- Hemangiosarcomas - this is the malignant version of this tumor and these need to be quickly and completely removed surgically. Hemangiosarcomas tend to be larger, and tend to have a more irregular cobble-stone surface. These tumors can also be found internally, and they can be fatal.
Here are pictures of a hemangiosarcoma (click for full-sized)
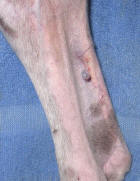

- Melanomas - a very serious cancer. These tumors are often black, not blood-filled red, and may be thick or flat. The borders may be irregular and hard to define. Melanoma's spreads to other areas, and can also be fatal.


