THE HEALTH OF THE RACING GREYHOUND by TOM C. MEULMAN
Every effort has been made to provide accurate up to date information consistent with respected Veterinary authority.
However, the author accepts no liability for errors or omissions.
This publication also contains advice, opinions and manipulation procedures that are strictly the author’s opinions and procedures.
THEREFORE, ANYONE USING OR INTENDING TO USE THE ADVICE, OPINIONS OR PROCEDURES DESCRIBED IN THIS PUBLICATION DOES SO AT THEIR OWN RISK.
SELECTION OF RACING STOCK
To train greyhounds and be successful is not easy but certainly possible, providing some basic common sense rules are followed, strictly adhered to, and you have a little bit of the right kind of luck.
As the saying goes, “you cannot make a silk purse out of a sow’s ear” and every successful trainer will tell you that the selection of suitable racing stock is the first step to winning races.
This saying has even more validity when it comes to breeding your own racing stock
One of the worst mistakes I ever made was keeping a bitch for breeding, in the knowledge that she had very little ability, and in the forlorn hope that maybe the right sire would make her produce a litter of handy greyhounds.
Thousands of dollars later, I had to face the fact that this bitch would never be worthwhile breeding proposition.
A sorry position to find yourself in, and one I would not wish on anyone; besides the heartache, it is also an expensive lesson to learn.
When you buy a greyhound puppy or breed a litter, you cannot realistically expect the offspring to be faster than the slower of the two parents. I know it does happen, but that is the exception not the rule.
PHYSICAL LIMITING FACTORS
It is simple mechanics that the physical structures of the greyhound to some extend limits it’s speed, as well as dictate how sound this greyhound will race.
In my opinion the preferred physical shape of the racing greyhound is as follows:
Front Legs
Viewed from above you should be able to draw a straight line from the outside front edge of the shoulder blade to the centre of the elbow joint, the centre of the wrist joint, and finish central on the foot.
Any deviation away from this standard may cause some long-term injury problems.
For instance, in some greyhounds the point of the elbow protrudes outwards, this will increase the possibility of track-leg problems, simply because it reduces the clearance between the front leg, and the inside of the hind leg during part of the stride.
The wrist needs to continue in a straight line in relation to the long bones in the front leg, any sideways angulation will increase the strain on the ligaments and tendons of the wrist joint, and may lead to long term repetitive strain damage.
The feet should be neither turned inward nor outward.
While galloping the greyhound rotates the foot in the direction of it’s running line, and if the feet are turned naturally outward this will in turn force the elbow to turn outward, again reducing the clearance to the inside of the hind leg.
Many trainers will select a greyhound with turned in feet (pigeon toed) in the belief that this may reduce the chance of track-leg occurring, as the elbow turns inward during the stride, but doing so will turn the elbows closer to the trunk, possibly hampering the galloping action, in particular if the greyhound has a broader than normal rib cage.
The other problem that occurs with a pronounced inward turn on the foot, is that this will increase the strain on the rail side wrist joint while driving through the turns.
The Shoulder Blades
When viewed from the side, they should angle forward approximately 36 degrees in relation to a vertical line drawn from the tip of the blade to the ground.
This will allow the front legs to reach maximum forward extension without undue strain to the muscles of the shoulders, in particular the Long Head of the Triceps.
The shoulders should be closely coupled to the trunk, with the top of the blades level with the spine.
Shoulder muscles should be well developed and defined without excessive bulk; if the front end looks bigger and more developed than the hindquarters, it is likely that the greyhound is suffering from a lower back problem, or some type of bone damage to the hind legs.
The Wrists
When viewed from side on, these should be a straight continuation of the front leg, or stand slightly forward at the foot.
Any weakness in the ligaments or bones of the wrist joint that allow the wrist to flex forward unduly, will not only result in further ligament strain and possibly damage to the Carpal bones, but if severe enough may also reduce the length of the greyhounds stride.
Head and Neck
The only feature of the head and neck that may affect the galloping action, and thereby the speed of the greyhound, is that the head and neck should be carried well forward, as this will reduce the up and down movement of the head during the stride.
The size and shape of the head is rather unimportant when it comes to pure speed.
However, I must admit that I prefer a greyhound with a head that looks almost too small for its body, rather than the other way around.
Ribcage
The ribcage should be reasonably flat and not bulge outwards, as this may interfere with the smooth straight action of the front legs.
As far as the depth of the chest is concerned, it is generally accepted that the underside of the Pectoral muscles should be somewhere in line with the tips of the elbow joint when viewed side on, and thereby providing good depth, and sufficient space for the heart and lungs.
The Spine
This should be broad and well muscled, either straight or with only a slight arch to the lower portion, and with a strong well-muscled coupling to the pelvic area.
Greyhounds with a flat spine or only a slight arch, will be able to extend the hind legs out further.
This type of spine is capable of going concave during the full extension part of the stride, and this reduces the tension on the upper muscles of the hind leg, such as the Tensor Facia Lata and Lateral Vastus.
It has been said, that the greater the distance between the pin bones and the start of the tail, the faster the greyhound is capable of running.
There is some truth in this observation, as it gives a good indication of the type of pelvic bone where the hind legs are set back further, again allowing for easier extension of the hind legs.
Hind Legs and Hocks
Most of the driving power of the racing greyhound is derived from the lower spine and the muscles of the hind legs; it is for this reason that the hindquarters should be well developed, and possibly the most prominent feature of the greyhound.
The pelvic area should be broad with good development to the Gluteal muscles.
When viewed from above and behind, the hind legs may curve out slightly from the hip to the knee and then form a straight line to the foot allowing the dog to stand slightly wider with the hind feet than the front feet.
The line from the tip of the Tarsus (the uppermost part of the hock) to the foot should be straight, as any sideways angulation in the Tarsus / Metatarsus junction will eventually lead to hock damage.
Many greyhounds have hind legs that are turned out, where the foot instead of facing straight to the front of the greyhound faces slightly outward.
This slight deformity does not to appear to affect the speed of the individual greyhounds, however, I believe that on a tightly turning racetrack this may increase the side slip of the hind foot, and thereby contribute to the chance of hock damage.
The hind leg when viewed from the side, should again show a well developed muscle structure, and hocks that are straight from the tip of the Tarsus to the foot, with good angulation where the hock joins the rest of the hind leg.
The greyhound when standing normally, should stand with the hind feet well back, to the extent that the hocks are almost in a vertical position.
Straight hocks should not be confused with a structural deformity known as “cow hocked”; this is a problem that thankfully occurs only rarely. Where when viewed side on, the hind leg is virtually a straight line from the knee to the ground and the greyhound looks as if it is walking on stilts.
The greyhounds that I have seen with this problem, appear to be able to run with reasonable pace in a straight line, but tend to lose balance on tight turns.
The only other observation I should make in relation to the muscle structure of the hind legs, is that greyhounds with a larger than normal Extensor Pedis muscle (the muscle at the outside front of the hind leg just below the knee), appear to have more early speed after jumping from the boxes, than the greyhounds with less development in this area.
The Feet
It is an old saying and a corny one, but very true “A greyhound runs on its feet”. Well sprung and knuckled toes will reduce the strain on the wrists, and allow the greyhound to cope with different surfaces, while flat or splayed feet will cause no end of problems with Sesamoids, tendons, and wrist ligaments.
MENTAL ATTITUDE
I have trained a number of greyhounds who looked like the greyhound equivalent of Greek gods, and had unlimited ability, but no matter what I did, just would not try in a race.
Then there were greyhounds that looked like superstars, but had no pace at all, or as they say in the classics, were absolutely legless.
At the same time, I have trained many greyhounds with some structural problems and only limited ability, that tried their hearts out and won their share of races simply by never giving up.
That brings us to the only point that really matters.
What makes one greyhound a better performer than the next greyhound?
Simple answer: the greyhound’s attitude!
In other words: it is the greyhound’s attitude to chasing and competing that wins the races; while the structure of the body and muscle tissue, are simply a limiting factor.
All you can do is to breed with, or select greyhounds from keen chasing parents, rear them on the best of food, educate them with care and patience, and hope for the best.
As far as fast twitch muscle fibre is concerned, again this is inherited, and the same rules apply. If one or both of the parents could not or would not run fast and race keenly, why breed or buy a greyhound from that bloodline?
However, if you do buy a greyhound from the right parents, why not pick one out that has all the physical attributes required for a long and successful racing career.
OBSERVATIONS
With most of the various information sections, the accent has been on understanding the scientific testing that can be done to detect those health problems that may severely affect a greyhound’s performance.
However, for any trainer it is essential to be able to recognise the early signs of ill health, before it becomes a major problem requiring expensive Veterinary or laboratory work, and much can be deduced by simply having a good look at the greyhound!
A greyhound should look like a fine racehorse, shining glossy coat, clearly defined muscle structure with veins clearly showing, bouncing on its feet and full of energy.
It is extremely difficult for most Veterinarians and Chiropractors alike, to point out to their trainer clients the obvious general condition problems that may exist with some of their greyhounds, problems that in the long term increase the likelihood of muscle and stress damage.
In the past I have tried to point out some of these to my own clients, only to lose them for good. There again, no one likes to feel they are being criticised, even if it was during a genuine attempt to help them improve the greyhound’s performance.
DEHYDRATION AND SKIN TONE
Because a major portion of the fluid reserve is stored within the skin, skin tone is a good guide to the greyhound’s general state of hydration, and dehydration is often the first sign of something going amiss.
Slight Dehydration
The skin is slow to spring back above the coupling, but snaps back OK above the saddle area.
TREATMENT: provide 40 ml of Vitrate or Recharge in 2 cups of milk and water twice daily for the next two days. Re-access the distance the dog is running over and increase sodium and potassium in diet.
Moderate Dehydration
The skin is slow to spring back above both the coupling and saddle, but it does flatten out and there are no signs of weight loss or excessive urine production.
TREATMENT: provide drinks as for slight dehydration, plus inject the greyhound with 2 ml of TRIDENOSEN or similar in each back leg daily for two days, reduce work to walking only until the problem resolves.
Re-access the greyhound’s workload, and have a hard look at the diet and general state of health.
If the problem does not resolve itself within 7 days, blood test to check for infection, sodium, potassium, acid-base balance and PCV.
Severe Stress
Skin over coupling feels tight and is difficult to lift and slow to return, and the greyhound is usually drinking large amounts of water at this time.
Seek urgent VETERINARY advice, including intravenous fluids.
Severe Dehydration
The skin stay’s ridged after having been lifted up; the greyhound has lost weight and appears lethargic, is drinking excessive amounts of water and produces copious amounts of almost clear urine, generally in a slow dribble.
Seek urgent VETERINARY advice, including intravenous fluids.
Do not run the greyhound for at least 14 days, even if he appears to have recovered, and when you do, start with a 250 Meter handslip every third day for 3 runs, before running behind the lure again. Starting with a 14 second run and increasing only by 2 seconds every 2nd run.
BODY SHAPE
The shape of the greyhound’s body structure, and how it stands, will also provide some clues to both the health and soundness of the dog.
When the dog is standing relaxed, is he standing with all four feet equally taking the weight, or is he leaning slightly one way, with a foot just resting on the ground?
If that is the case, careful examination of the pads, toes, wrist joint, wrist tendons and muscle structure, including the area where the leg joins the trunk is indicated. If this occurs with a front limb, also carefully examine the area at the base of the neck, between the shoulder blades, and the saddle muscle area.
The toes are they well knuckled, or are some of the toes straighter or flat on the ground?
Again careful examination of the appropriate toes and tendons is required.
If some of the toes are flatter than others, TENS contracting treatment (toe flexion) to the muscles that operate the toes may improve the functioning of the toes, and reduce the chance of further toe Sesamoid, or toe tendon damage.
When you lift the front of the dog slightly off the ground, by placing one hand under the chest the other under the neck, do both front legs hang straight down with the toes pointing to the ground, and are both front legs exactly equal lengths? When you lower him slowly to the ground, does he place both feet on the ground at the same time?
If the answer is no, then careful examination of the muscles of the shoulder, base of the neck and THORACIC spine is indicated on the side where the leg is being held shorter.
If the leg is held forward, examine the muscles on the front of the shoulder and chest, or if the wrist of one leg is slightly flexed backwards, examine the muscles of the forearm.
The shoulder muscles, are they the same size and structure on each side of the dog, or are some of the muscles bulging out more than others? A muscle slightly larger than its twin on the other side may indicate muscle damage in the body of the muscle, or at its origin.
Are the muscles of one shoulder visibly flatter than the same muscles on the other side of the dog? If so, there may be some damage or compression to the nerves that operate those muscles, and examination of the upper THORACIC spine as well as the muscles themselves is required.
Is the spine strong and solid, with good strong lumbar muscles on each side, or are some of the spinal segments sticking up further than others, lifting the hair up on one side of them?
Reduced lumbar muscles may indicate weight loss, stress or dehydration, while some raised spinal segments, in particular those of the central spinal area, could indicate pain in the kidneys, gut or bladder, as well as possible spinal muscle spasm.
The ribcage, is it flat and well covered, or are the ribs on one side bulging out a little more than on the other side? Too many ribs clearly showing may indicate weight loss, stress, or dehydration. While a slightly bulging ribcage, more on the left side of the dog than on the right, is a likely indicator of an enlarged liver, and past or current liver problems.
The hindquarter of the dog is that in proportion to the front half, or does the hindquarter really belong to a smaller dog?
Greyhounds require good strong hind legs and coupling, as most of the driving power is derived from this area.
When a greyhound has a smaller hindquarter in relation to the front half of the body, this may indicate that the greyhound is using the front legs rather than the hind legs for driving power.
The cause of this may be a severe and long standing lower back problem. When spinal damage occurs during rearing, there is often a marked reduction in the development of the hind quarters, due to both pain and nerve compression.
COAT CONDITION
The hair of the coat will also provide some insight into the greyhound’s current state of health.
It should consist of soft shiny hair with a soft undercoat of smaller finer hairs, and the coat should be light and flat, clearly showing muscle structure.
Thick Woolly Coat
Carbohydrates provide not only the energy for muscle function, but also for body heat.
A thick woolly coat indicates the animal has a real need to conserve energy and heat.
TREATMENT: blood test to check for infection, examine the diet for sufficient carbohydrate content, possibly increasing the kibble or biscuit portion and look at the kennel arrangements.
A thick woolly coat does not provide the ideal conditions for cooling down after a race or hard run, and will increase the amount of panting the dog has to do.
Soft Dry Coat
With increased amounts of dandruff after a wash or hydro bath.
TREATMENT: Add cod liver oil and blood building supplement to the diet.
Soft Dry Coat
With irregular bald patches on area’s where the dog has been laying or rubbing
TREATMENT: Add cod liver oil, blood building supplement, and zinc from kelp or green leaf vegetables to the diet. Blood test for Thyroid function (free T4)
Soft Dry Coat
With a narrow strip of straight hard shiny hair along spine
TREATMENT: Blood test for kidney and liver function, worm the dog twice 14 days apart with a broad-spectrum wormer. Add cod liver oil and blood building supplement to diet, treat for two weeks with Liver Tonic, and reduce workload.
Soft Dry Coat
Interspersed with hard coarse hair showing a distinct kink or curl at the end of each hair.
TREATMENT: Blood test for kidney and liver function, worm the dog three times 14 days apart with a broad-spectrum wormer, and again 14 days later for hook worm only. Increase protein content of diet (meat), add cod liver oil and blood building supplement, treat for four weeks with a Liver Tonic, and reduce workload.
Note: A distinct kink, hook or curl, at the end of the hair generally indicates worm load, and or severely increased toxicity levels.
Almost Normal Coat
Not quite shiny enough with the hair curving slightly up at the end of some top hairs
TREATMENT: Add cod liver oil to the diet and treat with Liver Tonic for one week, reduce workload slightly.
Thin Shiny Coat
With some loss of hair to the outside of back legs and under the chest
It is not unusual for a racing greyhound in hard work to lose some hair in these areas.
If performance is poor, obtain a Thyroxin T4 or free T4 blood test.
THE EYES
There are a number of infections and problems that affect the eyes and all of them are best treated by your Veterinarian.
However, by carefully looking at the eyes there is some important information available about your dog.
In a healthy greyhound with a good blood count, and the right Haemoglobin levels, the area above and directly adjacent to the iris, will have what can only be described as a sky blue halo.
And as the Haemoglobin and therefore the oxygen content of the blood reduce, this area becomes grey.
While just inside the top edge of the iris, you may see a slight white line in the surface of the eyes of some greyhounds; this could indicate past or current liver problems.
Past liver problems may also be indicated by what appears as a brown stain in the outside corners of the eyes. This may show as a light to dark brown area to the white of the eye, clearly defined where it is exposed to sunlight.
It is my belief that increased blood levels of BILIRUBIN due to liver damage, and the subsequent jaundice effects, plus the action of ultraviolet light on the eyes, are the cause of this phenomenon.
WHAT DOES IT ALL MEAN?
Examples and likely combinations of visible changes and possible ill effects
(1)
SKIN TONE: OK.
COAT: OK.
EYES: The blue halo has gone grey
BODY SHAPE: OK.
REFERRED PAIN: None.
POSSIBLE CAUSES: Reduced HAEMOGLOBIN levels.
EFFECT ON PERFORMANCE: Reduction in ability to run on, slight stress symptoms.
(2)
SKIN TONE: Slight dehydration.
COAT: Slightly less shine and the ends of some of the hairs are curling away from the body.
EYES: The blue halo has gone dark grey
BODY SHAPE: OK.
REFERRED PAIN: Pain in the junction of the LUMBO-DORSAL FACIA and LATISSIMUS DORSI. (5 mm above the bottom edge of the muscle over the coupling in behind the last rib.)
POSSIBLE CAUSES: Reduced kidney function due to infection and or excessive stress.
EFFECT ON PERFORMANCE: Reduction in overall ability.
(3)
SKIN TONE: Moderate dehydration.
COAT: Less shine with the ends of a large number of hairs curving away from the body.
EYES: The blue halo has gone dark grey, faint white line in the iris on the upper-side edges of both eyes, most visible in the left eye.
BODY SHAPE: Rib cage slightly enlarged at the last four ribs on the left side of the dog, and the LUMBAR segments T2 – T4 may be protruding above the rest of the spine.
REFERRED PAIN: Pain in the junction between the LUMBO-DORSAL FACIA and LATISSIMUS DORSI, the LUMBO-DORSAL FACIA and the crest of the ILIUM, upper TRAPEZIUS muscle.
POSSIBLE CAUSES: KIDNEY and or LIVER damage, severe viral or bacterial infection, or severe stress over a long period of time.
EFFECT ON PERFORMANCE: This dog is ill and should not be running at all.
It should be clearly understood that the external visible signs that warn of possible illness or damage, might be quite minor compared to what is happening inside the greyhound’s body.
Unless you are prepared to pay for a complete blood and urine profile every month, all minor changes in the appearance of the greyhound should be carefully observed and noted.
Taking a good look everyday at the skin tone, coat, eyes, and body shape of your greyhound, can alert you to possible health issues long before they become a performance affecting problem.
And it is worth doing, even when you believe the greyhound is performing at its best.
The health and well-being of the greyhound, is the total responsibility of the trainer, everything that happens to the greyhound, happens because of an action or decision by the trainer.
WHAT IS THE RIGHT RACING WEIGHT?
There is no doubt that every trainer will tell you, the best racing weight for any greyhound is the weight it runs fastest at.
However, to get to this ideal weight can be a little involved, as it depends on a number of factors.
Assuming that the diet is right, and the greyhound is fit and healthy, the first item to take into consideration is the greyhound’s natural body structure.
A bulky short-coupled muscle structure is designed for fast explosive speed, while the flatter long-coupled muscle structure is better suited to slower longer strides covering more distance.
Reducing the bulk of the short-coupled muscled greyhound may allow it to run smoother and further, but it will be at a cost to early speed.
Increasing the bulk of the long-coupled muscled greyhound, may provide for increased early pace, but at a cost in distance.
Therefore it is the adjustment to muscle structure, rather than the overall weight of the greyhound, that influences the way it runs, and how fast it runs over a designated distance.
There is also a fine line between reducing the greyhound’s muscle bulk to gain extra distance, and having the greyhound stress or cramp due to insufficient muscle energy storage.
(Energy meaning all the electrolytic and energy components required for muscle contraction)
To increase muscle bulk: Anabolic Steroid injections (STANAZOL) 1 ml weekly for 4 weeks then 1 ml every two weeks, increase complex carbohydrates 10% and protein 5% in diet.
To reduce muscle bulk: Soften the diet to include more broth and reduce solid meals by 5%.
Increase general massage and stretching Physiotherapy.
It should be remembered that increasing a greyhound’s weight would proportionally increase the stress on bones and joints, but will often reduce the general level of stress, and aid in post race recovery.
The opposite will occur when weight is reduced.
MUSCLE STRUCTURE, SPEED and INJURIES
A muscle does not only have to contract rapidly; it also has to stretch sufficiently to allow for full extension of the limb.
Increased muscle bulk and increased muscle tone increases speed of contraction, and thereby increases the speed of the greyhound.
On the other hand, excessive bulk and excessive muscle tone may reduce the extension of the limb, thereby reducing the greyhound’s stride, and therefore its speed.
Excessive muscle tone also increases the likelihood of muscle tears as the limb is fully extended under pressure.
Many of the main muscles are in the form of biceps (two parts), and triceps (three parts). Excessive muscle tone in one part of a muscle compared to the remainder of the muscle, almost guarantees muscle sheath damage between the various sections of the muscle.
WHEN IS A GREYHOUND TOO THIN?
An increase in weight is certainly warranted when the junction between the coupling and the last rib becomes a deep groove, rather than a slight concave.
In the situation where the space between the last two ribs becomes a deep groove, not only does the food need increasing, but also the stress levels on the greyhound require some rapid readjustment.
WHEN IS A GREYHOUND TOO FAT?
75% 0f the fat in the body is stored in the subcutaneous tissue including the skin.
Therefore the thickness of the skin is a good guide to excessive body fat.
If it feels like tissue paper the dog is too lean, there again, if it feels like pinching the skin around your own waist, the dog is most definitely too fat.
STRESS
STRESS WHAT IS IT?
WHAT DOES IT CAUSE? AND WHY?
To be stressed is to be fatigued and close to breaking point
Stressed and fatigued metal breaks, and in the biological sense this is also true of the body.
However, because there are so many processes involved in normal body function, a fatigue or breakdown in one or more of these processes, or the excessive stimulation of others, totally throws the whole system out of balance.
As these progresses beyond a certain point, the ability of the body to function normally is reduced, and the first thing to go out the window is the ability to perform exercise at a high level.
All body processes are interrelated, and depend on enzymes or hormones produced by other body processes.
Which in turn depend on available fuel (food), and also on what functions they have to perform. This controls what levels of enzymes and hormones are produced, which governs body processes that trigger other body processes etc. etc.
Biology is an extremely involved subject, and many people have spent a lifetime unravelling some of its complexities.
Therefore, any greyhound trainer who believes they can control and influence the way a greyhounds body functions, by the addition of chemical additives to the diet in various quantities, or the injections of various substances, are really kidding themselves.
In the short term it may get the results they are looking for, in the long term, it causes more damage than can possibly be imagined.
The same applies to unsuitable training techniques, they simply over stress or fatigue some body processes. This causes progressively worse imbalances, and further reduces the ability of the body to cope with stress.
You must keep in mind that all greyhounds are different, and have different tolerance levels. What will be an acceptable routine for one may totally destroy the next greyhound.
Excessive protein or the wrong type of protein in relation to the required protein-carbohydrate balance, and this depends on the level of exercise. May cause the body to burn protein for energy instead of carbohydrate, and so increase the quantity of waste it has to get rid off.
Excessive quantities of vitamins and additives in the diet may also increase the amount of waste the system has to eliminate.
It is also worth noting that the manufacturers of the huge quantities of food additives available to the greyhound trainer are in the business of selling products, and selling more is the name of the game.
Many of these products are extensively advertised with, if not direct promises, at the very least with hints of possible improvements in performance.
Most of the food additives I have examined, have a recommended dosage up to twice as much as I believe is required for good health, when they are added to the greyhounds normal diet.
If the advertising convinces the trainer that they are giving the greyhound something that may improve the performance, there is no doubt that many of them will increase the dosage even further, thereby causing the dogs system even more wastes to cope with.
It is all good and well to say that food additives are easily eliminated from the body, however, in many instances this involves the dogs kidneys, and in most greyhounds these are already a much abused organ, and not necessarily capable of functioning at an optimum level.
Vegetable oils, when added to the diet may reduce the absorption of essential fatty acids normally obtained from a meat diet, and this reduces the body's ability to synthesise some essential steroid hormones.
The daily use of alkalising agents, chemical kidney flushes, or so called acid neutralisers, cause major problems with normal body processes by increasing the elimination of some of the essential electrolytic ions and buffering agents from the body.
It is also important to note that acidic urine does not necessarily indicate that the greyhound’s body is over loaded with acid waste products; in some instances of acidic urine the plasma is in fact alkaline, as in intra cellular acidosis.
When we start a greyhound in training, the whole program is aimed at slowly improving the health and fitness of the greyhound, thereby allowing it to cope with progressively harder runs, until it attains peak fitness.
However, if you examine this a little further, you realise that it's not only the heart, lungs, and muscle system that need to increase in fitness, but also the system that stores energy in the body, and most importantly the system that eliminates toxic wastes from the body.
It only stands to reason, that if you provided a large quantity of glucose in the diet each day, and so provided the body with instant useable energy, the part of the system that stores energy will never attain its full potential.
The same applies to providing the greyhound with an alkalising diuretic or acid neutraliser after each and every run. It not only stops the waste removal part of system learning how to cope with a hard run, but may also destroy the health of the dog by stopping the kidneys from doing their job, increasing fluid loss, and the possible loss of potassium from the system.
Take the situation where you have a greyhound that plays up in the kennels prior to a run.
The barking and panting the dog does in the kennel or dog trailer is likely to cause respiratory alkalosis due to excessive carbon dioxide removal by the lungs.
On top of that, when you have a greyhound that gets over excited before a race, it is also extremely likely that after 6 or 7 runs, this dog will also be suffering from some degree of Hyperadrenocorticism, that is an over stimulated adrenal gland.
Let’s examine this greyhound’s likely condition at this point in time just prior to the run.
Possible respiratory alkalosis due to panting and barking
Possible intra cellular acidosis due to the potassium loss caused by the hyper- adrenocorticism
It is also extremely likely that the greyhound will also be anaemic to some extend, because haemoglobin is destroyed in the process of the body's attempt to buffer the toxic waste that is being produced.
Now give the dog his race start or a trial, and then lock the dog up in a small space, such as a racetrack kennel or a dog trailer, and let it pant some more. Then take the dog home and give it a good dose of an alkalising agent, which will further increase potassium and fluid loss.
You now have a greyhound where the biological system is so far out of balance, that no matter what you give it, recovery is extremely slow, and if the greyhound is raced or run again in three or four day's time, the problems are simply aggravated.
Or worse still, the trainer may decide that this greyhound needs resting for ten days, and then runs it over the same distance again.
Soon you have a greyhound that starts cramping, or suffers from increased muscle soreness, and muscle damage that is slow to repair, no matter how hard you work on it.
Next up is the increased pain in the nerve pathways due to spinal muscle spasm or muscle contraction, and the increased levels of wastes in the body due to what is by now poor kidney function.
By this time off course the dog will be on two Potassium tablets a day to combat the Potassium loss, and then it will need Anabolic Steroid injections to combat the muscle damage and muscle wasting.
This will aggravate the already depressed Thyroid gland due to the Hyperadrenocorticism.
That means the dog will have to go on Thyroxine tablets to offset the depressed Thyroid gland.
This will unfortunately cause some imbalance in the Calcium absorption rate, which means you will have to increase the Calcium intake to avoid hairline fractures.
You will also have to watch the dose rate of Thyroxine as overdosing has been suspected of causing heart muscle damage in racing greyhounds.
At this stage it is also a good idea to start feeding some lard, as this may help the dehydration you’re trying to keep under control.
But if you do that, you should also put the dog on a Methionine supplement to try and avoid fatty liver problems.
And heaven forbid lets not forget the Electrolyte supplement, this must of course be given in extra large doses, because lets face it this is supposed to fix the dehydration.
By now you are well into the veterinary treatments, and the dog will have had at least two blood tests, and one or two courses of antibiotics.
Because stress causes an increase in the white cell count and alkalising agents increase the likelihood of urinary tract and kidney infections.
Then of course it will also have had a treatment for the anaemia, and a treatment for a depressed immune system, which is damaged by the Hyperadrenocorticism, which is caused by the stress, that was caused by the training methods.
Sarcastic? Maybe so. Far fetched? Certainly not!
This is exactly what happens to far too many greyhounds, greyhounds that showed lots of potential, but never had a racing career.
Some greyhounds suffer from stress problems more than others do, and it is the excitable over keen hard chasers, that require the most amount of patience in race preparation.
As a general rule, for this type of greyhound it is best to consider the time spent running, rather than the distance covered.
Because it is the amount of energy the greyhound is capable of using before it becomes stressed, is the only important consideration, and this should include the energy it wastes prior to the run by barking panting and shaking.
From experience, I have found that even an extremely unfit greyhound that has had only one weeks worth of solid walking, can handle a 14 second run behind the lure, and one 14 second run improves fitness enough for an 18 second run.
However, it then takes a minimum of two runs over each distance, before increasing the next run by an additional 4 seconds.
Until such time as the greyhound starts running over two turns, this increases the stress factor considerably.
If for instance, the last two runs of the greyhound were over the 25-second distance on a U turn track; the run over two turns should not be more than 25 seconds, such as a hand slip at Sandown.
It may then take two or three hand slips before the greyhound is allowed to run the full distance, depending on how well the greyhound recovers from each run.
It is also extremely important, not to increase the distance or time spend running, until the greyhound runs the current distance, and pulls up reasonably sound and free of stress.
Many trainers run their greyhounds on straight tracks in the belief that this is not as stressful as circle running. If this is done as an easy hit out between circle runs, it is a great idea.
However, the overuse of a straight track brings its own problems, particularly in relation to increased breakdown of the muscles in the left hind leg.
When the greyhound is allowed to spin around quickly at the end of the straight, without the benefit of soft sand in the catching pen, this may also result in injury to the lower spine, wrists or right hock.
The next factor is the time spent resting between runs; the general rule is a minimum of two clear days, but not more than five. If for any reason the time spend off is longer than five days, you should reduce the greyhounds next run by two seconds for each additional day’s rest counting from the fifth day.
The next item to take into consideration is the amount of energy used by the greyhound prior to running, and this may be difficult to judge. However as a rule of thumb for a highly excitable dog I reduce the time spend running by 5 seconds for each half-hour the dog has to wait.
There have been a number of occasions when I've taken a greyhound back home from a trial without running it, simply because the wait was to long for the dog. There have also been times when I have taken a distressed dog out of the kennels for a late race, and have been concerned enough by its condition to request that the greyhound be scratched from the race.
There is a real chance of causing permanent health damage by racing or running a dog already suffering from severe stress.
However if you do get caught out, and the greyhound has a harder run than you anticipated, there are some things you can do to minimise the effect on the dog.
First of all cool the dog down properly, and then walk him around until he stops panting before re-kennelling or making the trip home.
All of which should be standard practice at all times for every greyhound after every run.
As soon as the greyhound is home in his own kennel, provide a drink of one cup of milk one cup of water and add 40 ml of Vitrate liquid concentrate or an appropriate dose of Recharge, then provide his normal evening meal.
There are some injections that may be of some benefit to the greyhound at this time.
My preference is for a product called Tridenosen manufactured by Nature Vet; inject 2 ml into each back leg. If this not available, you may substitute with 1 ml of DADA 250 + 3 ml of a product called Tripart distributed by Equipharm, Tripart and DADA 250 may be mixed into the same injection.
Provide the same drink again the next morning, and monitor the greyhound’s condition carefully during the day; at any sign of stress repeat the injections again that night. If there is no rapid improvement by the next morning, or the greyhound’s condition deteriorates, in particular signs of excessive water drinking and or excessive amounts of clear urine, seek urgent Veterinary attention.
ACIDOSIS
ACID-BASE BALANCE
CHLORIDE AND BICARBONATE
The determination of serum chloride and bicarbonate levels is mainly concerned with establishing the pH of the blood, and to determine the existence of either Acidosis, or Alkalosis.
METABOLIC ACIDOSIS
Describes any clinical condition in which HYDROGEN IONS accumulate in the blood plasma, because of an excessive quantity of acidic waste in the blood, due to excessive exercise, and or reduced kidney function.
The excessive amount of hydrogen ions in the blood may cause the transfer of hydrogen ions into the cell, to maintain balance, potassium ions then shift out of the cell. This will reduce the ability of the muscle cell to function normally.
Acidosis also favours retention of potassium in the body fluid, due to the lower levels of bicarbonate entering the kidneys.
Therefore greyhounds with metabolic acidosis may have normal or slightly higher levels of serum potassium; however the cells (intra cellular fluid) may be low in potassium (INTRA CELLULAR ACIDOSIS).
METABOLIC ALKALOSIS
Any clinical condition, in which there is a deficiency of HYDROGEN IONS in blood plasma, this may be caused by excessive intake of alkalising medication, or from loss of acids due to severe vomiting.
INTRACELLULAR ACIDOSIS
In greyhounds suffering from HYPERADRENOCORTICISM, potassium depletion may cause an increase in HYDROGEN IONS within the cell, this is then followed by the excretion of acid urine despite the fact that the blood plasma may be alkaline, and the greyhound may be suffering from METABOLIC ALKALOSIS.
The use of alkalising agents in response to a dipstick urine test (acid urine) will only aggravate the condition.
Correcting the low potassium level is essential for recovery.
RESPIRATORY ACIDOSIS
This refers to any clinical condition where CARBON DIOXIDE production in the body tissue, exceeds the ability of the lungs to remove it.
Respiratory acidosis is not common, except in extremely severe lung infections, or when lung function is depressed, either under anaesthetic, or from inappropriate drug use.
RESPIRATORY ALKALOSIS
This refers to any clinical condition where CARBON DIOXIDE removal by the lungs, exceeds its production by body tissue.
Respiratory alkalosis is relatively common in low-grade lung inflammation, such as kennel cough, or any condition that includes hyperventilation.
Greyhounds suffering pre-race stress syndrome, may suffer from respiratory alkalosis as a result of excessive barking.
However, body defence mechanisms in the case of respiratory alkalosis are extremely efficient, and the condition normally clears quickly without treatment.
Unless of course, the greyhound stresses as a result of a hard race, and quite often greyhounds that suffer pre-race stress syndrome, also suffer from Hyperadrenocorticism in which case the RESPIRATORY ALKALOSIS may be complicated by METABOLIC ALKALOSIS.
BODY FLUID pH is normally maintained within narrow limits despite the continuous addition of large quantities of metabolic acids from the various processes within the body, and additions of carbon dioxide from cell function.
Three different types of mechanisms defend against any large changes of the blood pH
These are:
Chemical Buffers
Buffers are compounds that can absorb or donate HYDROGEN IONS as may be required; these include proteins, phosphates, sodium bicarbonate, and haemoglobin
Shifts in Ions
HYDROGEN IONS may shift into (where they are chemically buffered), or out of the body cells as may be required.
Response by Body Organ’s
The kidneys can either retain or excrete acids, while the lungs, via increased or lowered breathing, can regulate ACID-BASE BALANCE by either retaining or expelling CARBON DIOXIDE.
MUSCLE FIBRES
Muscle fibres have specific measurable properties such as:
Peak Force: Or just how much strength the muscle fibre can produce. Contraction Velocity: Or just how fast a muscle fibre can contract. Resistance to Fatigue: Or just how long a muscle fibre can produce contractions before it tires.
Because Greyhounds aren't weight lifters, the Peak Force or the strength the muscle fibre can produce, while important, it is not a major consideration.
However, it is the ability of the muscle fibres to contract at high speed, and still be Fatigue Resistant, that is of more interest to the Greyhound trainer.
Research into the structure of skeletal muscle fibre has found three main distinctly different types, and these have been classified as:
Slow Fibre This type of muscle fibre displays slow contraction speed, and an extremely high resistance to fatigue.
Fast, Fatigue Resistant Of the fibres with fast Contraction Velocity, these muscle fibres were found to be able to maintain their Peak Force production even after a large number of contractions.
Fast fatigable This group of muscle fibres displayed high Contraction Velocity, and extremely large forces, but where unable to maintain contractions for any length of time without resting.
From these research results I would have to conclude that the Greyhound, who is a "dead set" stayer, must therefore have more Slow Fibres in the skeletal muscle tissue, while the Greyhound classified as a "three hundred yard screamer" has mainly Fast Fatigable muscle fibres.
However, what I did find extremely interesting was that the only biochemical difference found between the various types of muscle fibres, is in the way in which they store and use energy, and in the type of energy used.
Slow Fibres These were found to be high in the specific enzyme that is required by muscle cells to utilise oxygen to release energy from stored fat molecules, while they were extremely low in enzymes that make use of blood sugar as an energy source, and were low in ATP activity.
Which confirms what we have known all along, and that is to be able run on in a race you need oxygen, and the body needs to be able to use it.
The other interesting aspect of that bit of information is that if a stayer makes use of fat molecules for energy, it makes sense to feed a more fatty diet to a stayer than a sprinter.
It would also make sense to use substances such as L-Carnitine prior to a race to assist in delivering those fat molecules to the muscle cells, and to use B15 in the form of DADA 250 to increase the delivery of oxygen to the muscle tissue.
Fast Fatigable These muscle fibres were found to be extremely low in the enzymes needed to utilise oxygen, but high in the enzymes needed to use blood sugar for energy, and high in ATP activity.
Therefore, for those Greyhounds that can only run over the shorter sprint distances, it would make sense to provide them with more complex carbohydrates in the form of kibbled biscuit in the diet.
It would also make sense to use substances such as injectable ATP in the form of Dynacleine, Enerzyme or AMP 5.
Fast Fatigue Resistant These muscle fibres, which are the ones we all want our dogs to have, were found to be high in enzymes that utilise oxygen and blood sugar, and high in ATP activity.
So if you are fortunate enough to have a Greyhound with Fast, Fatigue Resistant muscle fibres, you can in fact make use of all the substances mentioned, such as:
A tablespoon of lard in the diet if the meat you use is lean
L-Carnitine to improve the utilisation of fatty acids
DADA 250 to dilate blood vessels and improve oxygen delivery
Enerzyme to increase ATP stores
There is no doubt at all, that the structure of the Greyhounds muscle tissue is an inherited trait.
However, excellent training methods, and the perfect health of the animal, can enhance the function of any type of muscle fibre.
There again, from my point of view, excellent training methods also include obtaining whatever information or knowledge you can, so that you can be more targeted and efficient in those training methods.
THYROID GLAND & THYROXIN
When levels of THYROXIN are decreased, it results in decreased physical and mental vigour.
FACTORS THAT INFLUENCE THE FUNCTION OF THE THYROID
Iodine Metabolism Iodine is essential to the production of Thyroxin, and is the only known function of iodine in the body.
Thyroid Stimulating Hormone (TSH) A hormone produced by the pituitary gland stimulates activity of the thyroid gland by increasing the uptake of iodide, and stimulating its conversion into Thyroxin
Thyroid Binding Globulin (TBG) Serum proteins acting as carrier agents for Thyroxin, and distribute it throughout the body.
Anything that affects the IODIDE metabolism, the production of TSH, or the binding of Thyroxin to GLOBULIN, affects the function of Thyroxin in the body.
Hyperadrenocorticism (Stress) This causes a rapid decrease in TSH (thyroid stimulating hormone), and greyhounds suffering this condition are often HYPOTHYROID. (Low serum Thyroxin)
Anabolic Steroids These decrease the levels of available TBG (Thyroxin binding globulin), and so reduce the level of Thyroxin in the body.
There is also a genetic factor involved in thyroid function, in animals where it exists; much of the body iodide is not available for Thyroxin production.
LOW PLASMA THYROXIN Demonstrated by a test to determine the globulin bound level of Thyroxin (T4) or a test to determine the level of Thyroxin not bound to globulin (free T4), is extremely common in the racing greyhound, in many cases this may be due to severe stress.
Generally treatment consists of providing oral supplements of THYROXINE SODIUM.
The initial dose should be small, and increases made at 14-day intervals until the desired metabolic balance is achieved.
At this time it may also be worthwhile to provide the dog with extra iodine in the diet, by adding a pinch of iodised salt to the main meal each day.
Iodine may also be given as a supplement: 2 drops of 2.5% Iodine in a cup of low fat milk, given as a drink every third day for 5 doses.
Adverse Reactions Some dangers exist in providing excessive doses of oral Thyroxine in an attempt to rapidly increase thyroid hormone levels.
Administration of Thyroxine further depresses TSH production, possibly compounding the original cause.
Excess levels of Thyroxine may lead to heart muscle damage, and or bone fractures.
A single dose may take up to a week to develop its maximum response, and repeated daily doses may have a cumulative effect, which does not become fully apparent for 14 day’s or more.
The initial dose should be small, usually 100 microgram daily, and increases made at fortnightly intervals by 50 microgram until the correct metabolic balance is achieved.
Overdose may cause restlessness, increased excitability and the possibility of heart muscle damage during strenuous exercise.
As well as supplementing the thyroid hormone levels with Thyroxine sodium, every effort should be made to rectify the training program and reduce the stress levels.
PARATHYROID HORMONE (PTH) Small glands that are attached to the thyroid gland produce PTH.
PTH acts in conjunction with other hormones to control the CALCIUM and PHOSPHATE levels in the body.
When calcium intake is insufficient, it elevates the serum calcium level by dissolving CALCIUM SALTS in the bone, and increasing the excretion of PHOSPHORUS.
The primary function of the PARATHYROID HORMONE is to maintain the concentration of IONISED CALCIUM in the plasma within a narrow range, in spite of wide variations in CALCIUM intake.
COPROPHAGY
In certain situations Coprophagy is considered normal animal behaviour, for instance brood bitches normally ingest the faeces of their puppies from birth to about 3 weeks of age.
Many theories have been put forward as to the cause of Coprophagy; except for the behaviour of brood bitches the underlying cause for this abnormal behaviour is unknown.
It is generally assumed that it may occur as a result of certain dietary deficiencies.
However, in my experience Coprophagy in the racing greyhound is mainly associated with problems of the digestive system, such as Pancreatitis, or low grade gut infections.
It may therefore be worthwhile to treat the dog with a course of broad spectrum antibiotics, include a digestive enzyme additive in the diet such as Thrive D or Yakult, and make certain the dog receives enough food to slightly increase body volume, and empties properly on it’s walks.
Other possible causes listed that should be investigated are:
- Stressful conditions, such as abrupt changes in normal routine (a change of kennel or new dog in the kennel).
- The diet should be carefully analysed for any deficiencies, in particular for trace elements.
- Check for worm infestations such as tape, round or hookworm.
BLOOD & BLOOD PROFILES
On the other hand, everything that affects the blood will affect the body in some way.
It is for this reason that blood profiles are one of the best tools available to the trainer in determining the true state of the greyhound's health.
However, there are a large number of tests that may be carried out on a blood sample, and it is mainly the cost of these tests, that limits the number of compounds that are tested for at any one time.
It is therefore important that the trainer provides the Veterinarian with the right information regarding any symptoms they may have observed in the greyhound. This will assist in determining exactly what compounds of the blood should be investigated.
As with any investigation, if the wrong questions are asked the wrong answers will result.
A good understanding by the trainer as to the functions of the major blood components will greatly improve the overall process.
This knowledge will also assist the trainer in determining whether or not the feeding and training program is affecting the greyhound’s blood profile in any way, thereby the body, and ultimately the greyhound’s performance on the race track.
BLOOD Blood is a liquid that circulates in what is virtually a closed system of blood vessels.
It consists of solid elements; these are the red and white blood cells and the platelets.
All suspended in a liquid medium, the plasma, this also contains solids in the form of proteins; these are Fibrinogen, Albumin and Globulin.
Fibrinogen is one of the main compounds that cause blood clotting.
Blood also contain a number of biological minerals essential for normal muscle function and fluid balance, such as Sodium, Potassium, Calcium, Bicarbonate and Phosphorus, as well as the waste products and enzymes produced by the various organs and muscles.
FUNCTIONS OF THE BLOOD RESPIRATION Transport of oxygen from the lungs to the various tissues, and the removal of carbon monoxide from the tissues to the lungs
NUTRITION Transport of absorbed food nutrients
EXCRETION Transport of wastes to the kidneys, lungs and intestines for removal
MAINTENANCE of normal pH balance within the body
REGULATION of water balance between intracellular, and extra cellular fluid
REGULATION of body temperature by the distribution of body heat
DEFENCE against infection with the white cells, and circulation of antibodies (anti viral)
TRANSPORT of hormones to regulate the metabolism
TRANSPORT of enzymes and vitamins
HAEMOGLOBIN This is the oxygen-carrying component of the red blood cells.
Any reduction in functional Haemoglobin will immediately affect performance.
A packed cell volume test (PCV) of the blood will provide some indication of the level of red blood cells, and therefore an indication of Haemoglobin levels, however, even moderate dehydration will affect the PCV, and may provide a misleading result.
Non functioning Haemoglobin The ability of Haemoglobin to carry oxygen to the tissues, may also be affected by the production of non-functioning Haemoglobin taking the place of normal Haemoglobin in the red blood cells, these are Methemoglobin and Sulfhemoglobin.
This alteration to the Haemoglobin may be caused by treatment with antibiotic Sulphonamides such as Sulphanilamide, Sulphathiazole and Sulphapyrine, or the feeding of raw onions in the diet, due to a component of onion oil called Alylpropyl Disulfide.
It is also of some concern that many racing greyhounds are fed meat obtained from diseased or dead cattle that may have been treated with Sulphonamides or some similar substance, and thereby impregnating the meat with a sufficient quantity of drug to cause non-functioning Haemoglobin to be formed.
Of greater concern is the fact that most of this meat is treated with a preservative.
The product used is either Sodium Sulphite, or Sodium Metabisulphite; both destroy the Thiamine (Vitamin B1) in the diet.
In the long term, this may cause severe nervous system damage, and possibly even death.
Sodium Metabisulphite, under the right conditions, will breakdown to Sulphur Dioxide.
This is a gas that at 500 parts per million will kill, and it is my opinion that there is a real good chance that both these products may cause problems with the Haemoglobin in susceptible Greyhounds.
Normal blood should contain 19 to 21 g/dl of Haemoglobin. As little as 0.5 g/dl of Sulfhemoglobin, or 1.5 g/dl of Methemoglobin is sufficient to cause rapid oxygen depletion of the body during exercise.
It is reasonable to assume that when a greyhound races over its normal distance while suffering this syndrome, all other aspects of the blood profile would show symptoms relating to severe stress.
Further investigation of the Haemoglobin may be of some value in greyhounds suffering sudden loss of stamina.
ANAEMIA This is lower than normal levels of red blood cells, and may result from a decreased production, an increased loss, or an increased destruction of red blood cells.
Decreased production may occur due to loss of function of the blood forming tissue, as with some types of cancers or chronic infections.
Anaemia may also be caused by a lack of iron, B12, and or protein in the diet.
Increased loss may be due to a severe worm infestation or internal haemorrhage, and blood loss via the intestines or urine.
While increased destruction is generally caused by a combination of several factors, such as: infections, excessive workload or stress, increased levels of waste products in the blood, or may even be due to regular exposure to Carbon Monoxide from car exhaust fumes entering a dog trailer, simply because Carbon Monoxide combines with Haemoglobin more readily than Oxygen with Haemoglobin
MCV = Mean Corpuscular Volume
MCH = Mean Corpuscular Haemoglobin
MCHC =Mean corpuscular Haemoglobin Concentration
The results of tests for MCV, MCH and MCHC are generally used to determine the type and severity of the anaemia.
EPO (ERYTHROPOIETON) EPO is a hormone that is synthesised by the kidneys, and stimulates the production of red blood cells from the bone marrow.
This genetically engineered version of the hormone is used in chronic kidney failure to treat Anaemia
EPO acts on the immature cells in the bone marrow by maturing them much faster.
This process takes several days, and any noticeable rise in the Haemoglobin may take two weeks or more.
However, EPO is an illegal drug, and its use in an attempt for a quick fix solution for an anaemia problem in Greyhounds is dangerous and stupid.
It is dangerous due to the fact that dehydration occurring as a result of running with the illness that caused the anaemia, may result in permanent heart damage to the Greyhound.
It is stupid because it does not solve the problem that caused the anaemia in the first place.
WHITE BLOOD CELLS (WBC) A decrease in total white blood cell count is generally associated with severe destruction, an excessive demand, or decreased production by bone marrow and lymphoid cells.
Greyhounds with a chronic low white blood cell count are immune deficient, and often develop secondary bacterial infections.
Low white blood cell counts may also be caused by toxin producing infections.
Bactericidal antibiotics, rather than bacteriostatic antibiotics should be used when there is an infection present, as well as a low white blood cell count.
Chronic inflammation or infection may cause an increase in the white blood cell count.
However, white cell numbers may also increase significantly without the stimulation of inflammation or infection, it may also be due to Epinephrine release from excitement, and is often seen in easily excitable greyhounds, and those suffering from the pre-race stress syndrome.
NEUTROPHILS Because neutrophils comprise a majority of the white blood cells, a low neutrophil level is usually associated with a general decrease in all white blood cells.
Low neutrophil level (neutropenia) may be caused by increased use, or decreased production.
Increased use of neutrophils may be caused by a viral infection, severe inflammation, or overwhelming bacterial infection.
Decreased production is often associated with immune deficiency due to depressed bone marrow and lymphoid cell production. However inappropriate drug administration, as well as Infectious Canine Parvovirus may also cause a low neutrophil level.
Increased neutrophil level (neutrophilia) is usually caused by bacterial infections, but neutrophilia alone does not confirm the existence of an infection.
This is because other non-infectious problems, such as acute pancreatitis, severe stress, Glucocorticoid (Cortisone) therapy, or an increased workload and increased muscular activity, may also increase neutrophil levels.
Defects in neutrophil function may also increase neutrophil counts, because the existing neutrophils are not effective, and more are produced in response to body requirements.
LYMPHOCYTES Decreased lymphocyte count (lymphopenia) may be caused by chronic infections, severe stress (Hyperadrenocorticism), kidney failure, or prolonged use of Glucocorticoid (Cortisone) injections.
As a general rule, low lymphocyte count indicates a viral infection, while prolonged lymphopenia could indicate that the body is unable to respond to the disease.
However, of the total number of body lymphocytes only 10% are in circulation, therefore it is not always possible to be certain in the short term, that low lymphocyte count (lymphopenia) indicates a poor immune response.
Increased lymphocyte count (lymphocytosis) is a common feature of chronic inflammatory disease, and could indicate a severe problem such as leukaemia or cancer.
MONOCYTES Increases in monocyte count (monocytosis) may be seen in greyhounds suffering severe stress, chronic infection of the stomach, or an abscess.
Monocyte numbers also increase in cases of neutrophil defects, when monocytes are required to take over some neutrophil functions.
PLATELETS (THROMBOCYTES) Platelets are produced by the bone marrow, and any process that interferes with marrow production will reduce platelet levels, while increased platelet destruction as a result of the body's immune response to infection, also reduces platelet count.
Because the spleen is the main platelet storage site, increased platelet count may occur due to spleen contraction in response to excitement, chronic iron deficiencies, bone fractures or muscle trauma.
EOSINOPHILS Increase in eosinophils is usually the result of severe skin infection, chronic fungal infection or severe flea, roundworm, hookworm or heart worm infestation. However, similar symptoms may also be caused by an allergic reaction to wheat in the diet.
Circulating eosinophil level will rapidly decrease after an injection of cortisone or ACTH.
BASOPHILS Any infection or infestation that results in an increase in eosinophils will generally also result in an increase in circulating basophils, in addition; any increase in lipids in blood, will also cause an increase in basophils.
LIPIDS An increase in the amount of circulating lipids in the blood, can be the result of a number of diseases associated with poor fat and carbohydrate metabolism, including: low thyroid function, over active adrenal gland, and pancreatitis.
GLOBULIN Most globulin (gamma globulin) is synthesised in plasma cells and lymphocytes as a part of the Immunoglobulins.
The major function of this globulin is to act as antibodies in the immune response, and to bind certain compounds in the body, such as hormones, and aid in their transport through the blood stream to their sites of action.
Approximately 3% of globulin is manufactured in the liver, these globulin are Metal Binding Globulin, and function to transport iron in the plasma.
A diet with insufficient iron causes an increase in Metal Binding Globulin, in an attempt by the body to maintain sufficient iron distribution to the red blood cells.
However, some types of chronic infections or liver disease, causes a reduction of the metal binding globulin, and as result there is a reduction in the ability of the red blood cells to regenerate, causing anaemia
The manufacture of functional globulin largely depends on the quality of the dietary protein; the best protein to produce globulin is milk protein, then egg, and then beef muscle protein.
Low Globulin (Hypoglobulinemia) Causes of decreased globulin are due to decreased globulin production, or increased globulin loss. Decreased production may be due to inadequate diet or decreased liver function. Increased globulin loss may occur with kidney damage, depressed immune system, or immune system overload by toxin producing bacterial infections.
Low globulin level will make the animal more susceptible to infections.
High Globulin (Hyperglobulinemia) High globulin count generally results from dehydration or increased globulin production; however, increased production is usually the result of chronic inflammatory conditions, both infectious and non-infectious.
Long-term excessive exercise, with increasing muscle breakdown and inflammation, as well as some types of cancer may also increase globulin production.
There is no doubt, that both human and animal athletes are more susceptible to infections, both viral and bacterial. This appears to come about because of hard exercise, increased muscle destruction, and general inflammation changing the structure of the globulin, and reducing its ability to provide the antibodies required for fighting off infections.
There are a variety of disorders that may be associated with increased globulin levels, the cause should be determined and treated appropriately, and if dehydration is present intravenous fluid therapy may be necessary.
ALBUMIN Albumin is synthesised in the liver from dietary amino acids.
Small amounts of albumin are lost in the urine and faeces, but most albumins are used in various metabolic processes such as tissue healing and repair.
The primary function of Blood Serum Albumin is to maintain the correct pressure of plasma, and act as a carrier for various compounds such as bilirubin, calcium, drugs, hormones, toxins and others.
Low Blood Serum Albumin (Hypoalbuminemia) Hypoalbuminemia may be caused by a large variety of clinical disorders; therefore the physical examination findings are variable.
Symptoms are generally related to the various metabolic processes involving albumin, such as poor tissue repair, soggy muscle tone, and in severe cases, signs of oedema when contributing factors are present, such as blood vessel damage or increased Serum Sodium with water retention.
When assessing the causes of the low serum albumin level, it is important to also take into consideration the Serum Globulin level, because serum globulin is usually determined by measuring the total Serum Protein level, and then subtracting the albumin concentration.
Globulin levels may provide some clues as to the causes of the low albumin level.
Even though, albumin and globulin levels should be interpreted independently, the Albumin/Globulin ratio may provide a useful indicator of liver function.
Increased Blood Serum Albumin (Hyperalbuminemia) The only recognised cause of hyperalbuminemia is dehydration, and should be corrected with appropriate fluid therapy.
ENZYME LEVELS & DISEASE
Because of the large number of different metabolic processes, there many different enzymes.
A number of these enzymes may increase in quantity in the blood serum as a result of a specific illness, disease, or accelerated cell destruction.
Vigourous exercise also results in the release of small quantities of muscle enzymes.
ALT (SERUM ALANINE TRANSAMINASE)
Increased ALT Increased levels of this enzyme are due to either increased cellular release, or increased cellular production.
ALT is located in the liver cells (HEPATOCYTE’S), and is released whenever there is liver cell damage or destruction.
ALT is liver specific in dogs; other enzymes released during liver damage include AST (ASPARTATE TRANSAMINASE), and LDH (LACTATE DEHYDROGENASE).
However, AST is normally present in higher concentrations than ALT, except in liver disease when ALT exceeds AST.
The levels of increased SERUM ENZYME activity equals the number of liver cells currently being damaged, but provides no information regarding the ability of the liver to heal, nor the current ability of the liver to function.
Neither ALT nor SAP (SERUM ALKALINE PHOSPHATASE) determinations are liver FUNCTION tests.
It is also important to note, that because the half-life of serum enzymes released during liver damage is only 2-4 day's, poor liver function may still exist with NORMAL ENZYME levels.
Decreased ALT There is no known significance to decreased serum ALT.
SAP (SERUM ALKALINE PHOSPHATASE)
Unlike ALT, there are certain enzymes that can gain access to the blood circulation without damage to the cells that produce these enzymes.
Significant increases in SAP are usually caused by increased cell production, and not usually by cell destruction.
Tissues and cells known to produce this enzyme include cells in bone, liver, bile duct, intestine and placenta.
Increased SAP levels are also seen in greyhounds injected with CORTISONE, and those suffering severe stress accompanied by HYPERADRENOCORTICISM.
Although the precise mechanisms are unknown, it has been reported that GLUCOCORTICOID also cause increased production of SAP (ALKALINE PHOSPHATASE).
The duration of GLUCOCORTICOID induced increase in SAP is unpredictable, but it can take several months for the SAP levels to normalise
When the blood profile shows increased levels of both SAP and ALT, check for and rule out, Hyperadrenocorticism, liver disorders, chronic active hepatitis, liver infection, or acute pancreatitis.
SAP levels are also increased due to rickets, over active thyroid gland, and bone damage.
AST (SERUM ASPARTATE TRANSAMINASE) Increase may indicate heart damage, jaundice, acute hepatitis, or severe tissue damage.
CPK (SERUM CREATINE PHOSPHOKINASE) Increase may indicate muscle damage or recent run.
GGT (SERUM GAMMA GLUTAMYL TRANSPEPTIDASE) Increased may indicate liver or biliary disease, hepatitis or pancreatitis.
GMT (SERUM GLUTAMYL TRANSFERASE) Increase may indicate hepatitis or pancreatitis.
GOT (SERUM GLUTAMIC OXALOACETIC TRANSAMINASE) Increase may indicate heart muscle damage.
GPT (SERUM GLUTAMIC PYRUVIC TRANSAMINASE) Increase may indicate liver damage.
IDH (SERUM ISOCITRIC DEHYDROGENASE) Increase may indicate liver damage, brain tumour or meningitis.
LDH (SERUM LACTIC DEHYDROGENASE) Increase may indicate recent heart damage, levels return to normal after 5 days.
POTASSIUM
Maintaining high levels within the cell (intracellular), and low potassium levels outside the cell (extra cellular), is critical.
This is accomplished with the sodium/potassium pumps located in the cell membrane.
Low potassium within the cell may cause abnormalities in many biologic processes; including the cell volume, acid-base balance, production of RNA and Glycogen, and dramatically reduces the ability of the cells to support muscle contractions.
Potassium intake and excretion determine the total body potassium content. Equally important is the distribution of potassium between extra cellular and intracellular fluid. If potassium intake were not matched by excretion, high serum potassium would soon result. Under normal circumstances salivary and gastrointestinal potassium losses are minor; therefore excretion of potassium by the kidneys is vital.
On the other hand, the fluid that is filtered by the kidneys contains much more potassium than is present in the extra cellular fluid. Therefore reabsorption of potassium by the kidneys is also vital to normal potassium balance.
In health, and without the interference of well meaning trainers, the kidneys efficiently maintain potassium within a narrow range. However, in contrast to the kidneys ability to completely reabsorb sodium, small amounts of potassium continue to be lost even when potassium levels are low. It is therefore important that potassium levels are maintained by the appropriate diet, or by supplementation where required.
Internal Potassium Balance This refers to the distribution of potassium within the cell (intracellular), and the potassium in the extra cellular fluid.
When potassium intake temporarily exceeds the ability of the kidneys to excrete it, the cells then take up more potassium to prevent the accumulation of excess potassium in the extra cellular fluid.
However, when kidney and gastrointestinal losses exceed potassium intake, transfer of potassium from the cells into extra cellular fluid occurs. While this delays the onset of a low serum potassium level, it can have a detrimental effect on the ability of the muscle cells to support efficient muscle contractions.
Factors known to affect the handling of potassium by the kidneys are: (1) The amount of potassium in the diet
(2) The amount of sodium and fluid being reabsorbed by the kidneys.
(3) Bicarbonate accompanying sodium through the kidneys, (bicarbonate increases the excretion of potassium).
(4) Aldosterone, this is a mineralocorticoid produced by the Adrenal gland, not only in response to dehydration, but also in response to an increased extra cellular concentration of potassium.
Aldosterone stimulates sodium reabsorption and potassium excretion by the kidneys, and therefore increases the likelihood of a low body potassium level in dehydration
With chronic diarrhoea, loss of large quantities of potassium in faeces can occur.
Finally with vomiting, even though potassium losses in gastric juice may be minor, it is the loss of gastric juice Hydrochloric Acid, and resulting dehydration, which may cause Metabolic Alkalosis, and trigger a loss of large amounts of potassium in the urine and thereby cause low serum potassium.
Hypokalemia (Low Serum Potassium) This may occur because of decreased potassium intake, redistribution of potassium from outside the cell (extra cellular fluid) to inside the cell (intra cellular fluid), because of loss of potassium from the body, and in Metabolic and Respiratory Alkalosis.
Hyperkalemia (High Serum Potassium) This may occur due to increased potassium intake, an inability of the kidneys to excrete potassium, and in Metabolic and Respiratory Acidosis.
In metabolic acidosis accumulation of Hydrogen Ions in the extra cellular fluid causes the transfer of hydrogen ions to the intracellular fluid, potassium ions then shift from intra cellular to extra cellular fluid.
Acidosis also influences the kidneys to retain more potassium due to the lower availability of Bicarbonate.
In Respiratory Acidosis, it is Hydrochloric and Carbonic Acids that displace potassium ions from the cells
Potassium Levels Since 98% of body potassium is located within the cell and not available for measurement, determining whether or not potassium deficit is present, is an indirect process.
Normal Potassium Serum levels in a greyhound with Acidosis may still indicate low cellular Potassium levels, while low Potassium level in a greyhound suffering Alkalosis may indicate a redistribution of Potassium from extra cellular fluid to intracellular fluid.
Therefore any determination of potassium levels in a blood test, must take into consideration both the hydration state of the Greyhound, and the possible existence of either acidosis or alkalosis.
Severe tissue trauma, such as torn muscles with obvious oedema, or severe bruising may cause significant cellular release of potassium. Good kidney function generally prevents Hyperkalemia. However, greyhounds that are already suffering from some stress and dehydration may become affected.
Both high (hyper), and low potassium levels (hypo), cause muscle weakness.
Life threatening Hypokalemia is rare, and treatment consists of giving Potassium Chloride tablets.
Severe Hyperkalemia is potentially fatal due to heart damage, and treatment should not be delayed.
Treatment is generally aimed at reducing the effect of potassium on the heart by giving Calcium, and reducing extra cellular potassium with intravenous Sodium Bicarbonate, or lactated Ringer's solution.
SODIUM
SERUM SODIUM and BODY FLUID REGULATION
It is sodium that is primarily responsible for the level of fluid in the body, and the distribution of water between the inside (Intra cellular), and outside (Extra cellular) of the cells.
Problems associated with deficit and excess of sodium reflect this function, deficit-causing dehydration, while excess could cause problems as severe as brain damage.
Cell membranes are relatively impregnable to sodium, but are easily penetrable to water, and any sodium ions that do gain access to the cell interior are actively pushed back into the extra cellular fluid by pumps in the cell membrane.
This pumping action depends on Potassium Ions, and as sodium is pushed out of the cells, potassium is pumped in. In this way, potassium maintains the intracellular pressure.
Since water easily flows between the intracellular (inside the cell), and extra cellular (outside the cell) fluid, concentrations of both these major fluids is always the same.
Normal regulation of body fluid volume also depends up on a balance between water loss, and water intake.
If increased drinking is not compensated by increased urine loss, body water must increase, end result, over hydration of the cells.
On the other hand, if increased drinking does not compensate urine loss, body water decreases, with resulting cellular dehydration.
The stimulation to drink is generated in, what is called the primary thirst centre of the brain, and the basic stimulation for the primary thirst centre is intracellular dehydration.
Stimulation of the primary thirst centre may also be triggered by volume and pressure receptors located in some of the larger blood vessels.
A reduction of 8% in blood volume or pressure can induce thirst, and stimulate the release of an anti diuretic hormone (ADH).
While a 2% change in the extra cellular fluid volume will also cause ADH release, and cause the kidneys to reabsorb water, and concentrate the urine.
In addition to water reabsorption, ADH also increases the reabsorption of Urea.
This is important, as Urea influences the ability of the kidneys to reabsorb water.
However, stimulation of the primary thirst centre is not the only mechanism that determines water intake in normal animals. Food intake as well as exercise, also triggers thirst in anticipation of possible water needs before any actual cellular deficiencies can occur.
Sodium balance is closely regulated and maintained within narrow limits regardless of large variations in the dietary intake of sodium. Although sodium is excreted from both the gastrointestinal tract and the kidneys, it is the kidneys that primarily regulate sodium balance.
Several factors influence this function; this includes a mineralocorticoid called Aldosterone secreted by the Adrenal Cortex, the volume of blood flow through the kidneys, and the availability of ADH and Urea.
In a normal healthy dog nearly 75% of the fluid that passes through the kidneys is reabsorbed
Essential to this function are Aldosterone, ADH, Urea, and Sodium.
Anything that affects the available levels of these substances will affect the ability of the kidneys to function normally.
So called acid neutralisers, alkalising diuretics, some infections (viral and bacterial), toxic substances and kidney disease, all reduce the ability of the kidneys to reabsorb water, and cause various levels of dehydration and loss of essential substances, such as potassium.
Low Serum Sodium (Hyponatremia)
Low sodium levels can be due to decreased intake, or increased excretion of sodium.
Any decrease in the serum sodium concentration following sodium loss is initially corrected by a reduction of both thirst and ADH secretion, reducing fluid intake and increasing urine volume.
In this manner serum sodium concentration is maintained, but at the expense of body fluid volume, causing rapid dehydration.
With progressive sodium loss, extra cellular volume (hydration) keeps on reducing, and at a critical point, (8% reduction in blood volume) blood vessel volume receptors stimulate extreme thirst and ADH production, causing a water gain, and a rapid decrease in serum sodium concentration.
Hyponatremia is characterised by signs of dehydration, decreased skin pliability, weak pulse, and the increased production of urine with low specific gravity (Polyuria).
High Serum Sodium (Hypernatremia)
High serum sodium causes water to transfer out of the brain into the extra cellular fluid, resulting in severe weakness and coma. Severe heat-stroke, excessive sodium administration, and kidney failure, may also cause high serum sodium.
This is life threatening, and requires immediate and appropriate therapy, which will depend on the degree of dehydration.
CALCIUM
CALCIUM and MUSCLE FUNCTION
In addition to calcium's structural role in bone, the concentration of Calcium Ions within the body is critical for normal muscle contraction.
Muscle fibres are connected to the nervous system via neuromuscular junctions; these junctions release a substance called ACETYLCHOLINE, the released acetylcholine binds to special receptors on the muscle fibres
This produces electrical activity by stimulating the movement of SODIUM and POTASSIUM IONS through the cell membrane, although this binding occurs for only a few milliseconds, it creates far more electrical activity than is required to stimulate muscle contraction.
This electrical activity generated on the surface of the muscle fibre is conducted into the cell, where it causes the release of CALCIUM IONS.
The calcium ions then modulate the acetylcholine, and stimulate contraction of the muscle fibres. (MYOFIBRILS)
A pump within the muscle cell returns the calcium ions to the cell, keeping the concentration of calcium ions in the myofibrils at an extremely low level, except when required for the next muscle contraction.
Calcium is present in the extra cellular fluid in three forms, IONISED, bound to ALBUMIN, or combined with CHLORIDE or BICARBONATE.
Only ionised calcium is biologically active in muscle contraction.
Most laboratory methods for measuring SERUM CALCIUM simply measure the total serum calcium, however this provides no real guide to the availability of IONISED CALCIUM.
Nor does simply measuring total serum calcium take into consideration changes in calcium value's depending on blood pH
ALKALOSIS decreases ionised calcium, while ACIDOSIS has the opposite effect.
Special equipment is needed to measure ionised calcium.
Low Serum Calcium (Hypocalcemia)
The initial symptom of low serum calcium may simply be an episodic weakness after a hard run.
If severe, the symptoms may include muscle tremors, panting, nervousness, seizures, and increased body temperature.
These signs may be sporadic instead of constant.
HYPOCALCEMIA is potentially life threatening and should be treated without delay.
High Serum Calcium (Hypercalcemia)
Although high serum calcium in greyhounds is rare, depending on the cause, the symptoms may include: depression, anorexia, constipation, weakness, Polydipsia / Polyuria (excessive water drinking and urine production) and cardiac arrhythmia's.
When high serum calcium is coupled with elevated SERUM PHOSPHORUS levels it may cause soft tissue mineralization, and severe kidney damage due to kidney calcification.
Severe HYPERCALCEMIA may be fatal.
BLOOD GLUCOSE
Sources of blood glucose are Exogenous (food intake), and Endogenous (produced within the body).
When food is not available, continuing body requirements causes endogenous glucose production.
The liver, under hormonal influences, maintains blood glucose for about 24 hours.
Thereafter, body proteins (mainly muscle) are used as the main source of endogenous glucose, resulting in a reduction of muscle bulk.
Several hormones increase blood glucose; these include Glucagon, Glucocorticoid, Epinephrine, Growth Hormone and Progesterone.
The Pancreas, using Glucagon and Insulin, controls the normal regulation of blood glucose levels.
When blood glucose decreases, Glucagon output from Alpha cells in the Pancreas increases, and Insulin secretion from Pancreatic Beta cells is suppressed.
Low Blood Glucose (Hypoglycemia) In the racing greyhound, Hypoglycemia is seldom seen in isolation, but generally as part of a syndrome that may include signs of liver failure, Adrenocortial insufficiency, and acute Pancreatitis.
The severity of the symptoms of Hypoglycemia is related more to the speed of the decline in blood glucose, than a gradual decrease, and generally cause few signs other than intermittent weakness after exercise, or occasionally 2 to 6 hours after eating.
With persistent Hypoglycemia check for Pancreatic tumours
High Blood Glucose (Hyperglycemia) The most common cause of mild to moderate Hyperglycemia is stress or excitement. Stress causes Glucocorticoid secretion by the adrenal gland, which results in the liver producing more Glucose.
While excitement causes Catecholamine release, and that also results in the liver producing glucose.
In severely stressed greyhounds suffering from Hyperadrenocorticism, other signs may include, Polydipsia (increased thirst), Polyuria (excessive amounts of urine), thin skin, some hair loss (due to Thyroid suppression), and possibly abdominal distension.
It is not usually necessary to treat the symptoms of Hyperglycemia, except to change and treat the underlying causes of the stress, such as changing training methods
CHOLESTEROL & FATTY ACIDS
CHOLESTEROL and FATTY ACIDS
Fatty acids are an essential part of the diet, and influence the growth of skin, healthy hair, kidney function and optimum utilisation of energy.
The ability to breakdown the fatty acid to components that can be absorbed into the bloodstream depends upon the availability of bile and pancreatic juice.
The Cholesterol part of the fatty acids is also required for maintaining energy levels, and the production of steroid hormones.
Cholesterol from egg yolk, meat and cod liver oil is easiest to absorb, while the addition of fatty acids from plant oils to the diet, such as peanut, corn or safflower oil reduces the absorption of cholesterol.
The body also synthesises cholesterol, mainly in the liver.
The cholesterol in the bloodstream is mostly derived from cholesterol synthesised by the body, while the fatty acids in the diet contribute to fat stores.
Approximately 50% of all body fat are stored in subcutaneous tissue (under the skin), while less than 5% is stored in muscle tissue.
The liver plays a central role in the processing of cholesterol, both by synthesising cholesterol and adding it to the blood, and removing it by oxidisation and excreting it into the bile.
However, both the thyroid and the adrenal gland influence the speed at which the liver processes fatty acids and cholesterol.
Low thyroid levels may lead to increased fat storage, as well as elevated levels of cholesterol in the blood, while prolonged high levels of blood cholesterol may further reduce thyroid function.
Hyperadrenocorticism (severe stress) will also reduce thyroid function and increase the levels of cholesterol.
CREATINE
Muscle contraction requires high energy, this energy is supplied by ATP (Adenosine Triphosphate), this in turn, is produced by the action of Creatine + Phosphate using a specific enzyme as a catalyst. Thus Creatine acts as part of the high-energy reserve, that is required for rapid and sustained muscle contraction.
Injections of Phosphate (Coforta) will increase production of ATP, while injections of Adenosine Triphosphate (Dynacleine or Enerzyme) will directly increase high-energy reserves.
Creatine + Phosphate = ATP Creatine (Cr) is one of the basic muscle energy stores in the body, particularly in fast twitch fibre
It combines with phosphate to form PCr
During exercise the phosphate and Creatine complex (PCr) is thought to be an immediate source for the high-energy phosphate groups with which to replenish ATP.
However there is some evidence to suggest that Creatine only contributes significantly to ATP for the first few seconds of intense activity.
Creatine Balance In the racing Greyhound it is estimated that Creatine has a turnover rate of approximately 3g per day, meaning that about 3 grams of Creatine is irreversibly broken down to the waste product Creatinine, and 3 grams synthesised to replace it.
There appears to be a natural balance between Creatine within the cell and Creatine circulating in the blood.
This balance can be altered only slightly by Creatine supplementation in the diet.
Within a few days, intracellular Cr levels reach a new equilibrium, however a much smaller fraction of this additional Creatine appears to be stored in the high-energy PCr form.
Finally the body appears to have a maximum level for circulating Creatine, and supplementation reduces Creatine production by the body.
Supplementation Creatine can be found in many forms, raw muscle meat contains approximately 0.5% Creatine by weight, commercial supplements are also available.
It has been suggested that Greyhound muscle have a maximum capacity of roughly 300-mmol Creatine per Kg of muscle, making supplementation in excess of 30g per day pointless.
Energy Effect A number of studies have examined the effect of Creatine supplementation on performance.
The consensus appears to be that, while not increasing strength, Creatine supplementation can increase the amount of energy available by about 8% and therefore increase the duration of function of fast twitch muscle fibre
The mechanism of this enhancement is not yet clearly documented, but is most likely due to the increased availability of PCr.
Resting muscle does not require high energy, 60% of the energy required for maintenance of resting muscle is derived from direct use of carbohydrate diffusing into tissue from the blood circulation.
INCREASED SERUM CREATININE Creatinine, the waste product of Creatine metabolism is excreted in the urine, and is not believed to be toxic, but is accompanied by toxic waste products that cause problems when there is a decreased excretion of Creatinine by the kidneys.
Complete urine analysis (not just a general dipstick test) is essential to finding the exact cause and determining the appropriate treatment.
BILIRUBIN & LIVER DAMAGE
70% is derived from the destruction of cells mainly in the spleen and liver, 10% is from bone marrow, and the remainder is from myoglobin breakdown.
Newly formed bilirubin is insoluble in water, and binds to circulating albumin.
This binding allows transport of bilirubin via the blood to the liver, and the now large bilirubin/albumin complex prevents diffusion across cell membranes, and helps to confine bilirubin to the blood vessels.
Binding ability may be reduced by the drugs, Sulphonamides and Salicylate, or in animals suffering acidosis.
Bilirubin separates from albumin prior to entry into the liver cell. Once inside, specific proteins bind the bilirubin; it is then combined with Glucoronic Acid to form bilirubin Monoglucoronide.
The importance of this process is that the bilirubin, previously insoluble in water, has now been transformed into a water-soluble compound, which is essential for its excretion.
Even in the event of considerable liver damage, this part of the system appears to continue to function efficiently.
Normally, the now water-soluble bilirubin is excreted from the liver cells into the bile ducts. However, this excretory system is extremely sensitive to various types of liver damage, and when the liver is under stress, increasing amounts of bilirubin are returned to the Plasma.
On the other hand, in greyhounds with liver damage the Total Plasma Bilirubin may not increase significantly. This is because dogs as a species, easily pass water-soluble bilirubin through the kidneys into the urine, and it is only when both liver and kidney damage occurs, that the plasma levels of bilirubin increase sharply.
The use of tests to measure the quantity of bilirubin in plasma is therefore not an accurate assessment of liver function in dogs.
As liver function is directly involved with bile production, measurement of Serum Bile Acids is a more reliable procedure to test current liver function.
When total plasma bilirubin exceeds 1.0 mg/dl, one can observe a yellow colour of plasma in a spun micro-haematocrit tube.
Impaired liver function leads to a decreased bile flow and is characterised by increased Serum Bile Acid and Alkaline Phosphates (SAP) levels.
There are drugs that may also cause decreased bile flow and increased serum bile acids; they include Corticosteroids, and long-term treatment with anti-convulsants, such as Dilantin or Phenobarbital.
Other drugs that may cause liver damage in dogs include Mebendazole (Telmintic), and possibly others such as Oxibendazole.
Liver damage may also be caused by Aflatoxins, a mould found on grain type foods.
Greyhounds, as a species, are also extremely sensitive to liver damage from Cholinesterase inhibiting compounds, mainly found in flea killing products.
When treating greyhounds for flea infestations, the product label should be carefully read and products listed as Cholinesterase Inhibiting should be avoided, or at least used strictly as directed.
Ongoing liver damage is often associated with marked increases in Serum Alanine Aminotransferase (ALT), and may include decreased concentrations of Blood Urea Nitrogen (BUN), Albumin and Glucose, with increased Plasma Ammonia, and with Bilirubin appearing in the urine in increased amounts.
A marked reduction of available bile due to liver damage, may also cause low levels of intermittent diarrhoea. This is due to low bile levels reducing fat and carbohydrate digestion, and bacterial action on the partially digested foods producing Lactic Acid and Hydroxyl Fatty Acids that irritate the intestines, and aggravate the diarrhoea by increasing gut secretions of fluid and electrolytes.
To obtain the full picture, any tests for Serum Bilirubin should be accompanied by a urine test for water soluble Bilirubin.
BLOOD UREA NITROGEN (BUN) Urea is produced in the liver from Ammonia and Amino Acids in the blood.
After entering the circulation from the liver urea is filtered through the kidneys, where it plays an important part in the fluid reabsorption ability of the kidneys, and is then excreted in the urine.
Low Blood Urea Nitrogen Low BUN can occur because of decreased production or increased excretion.
Decreased production is most commonly associated with chronic liver damage, or long term consumption of a diet severely restricted in protein.
Kidney disease, diabetes insipidus and some types of nephritis may cause increased excretion. However, increased excretion causing a low BUN is often seen in greyhounds with significant Polyuria.
Polyuria is the increased production of urine, generally urine of low specific gravity.
In some cases this is bought on by Polydipsia (increased thirst) triggered by severe intracellular dehydration.
This in turn may be caused by severe stress, due to a hard run by an unfit greyhound, or one suffering from a bacterial or viral infection.
However, some instances of Polyuria are in fact inflicted by the overuse of diuretic alkalising agents, the indiscriminate use of anti-inflammatory injections in injury treatments, or the use of Glucocorticoid injections, in the belief, that they may improve the greyhound’s performance.
It must be said however, because greyhounds are generally on a high protein diet, normal or slightly lower BUN levels, may not give a true indication of the severity of problems relating to possible kidney disease, resulting in the Polyuria / Polydipsia syndrome, and a varying degree of dehydration.
Increased Blood Urea Nitrogen An increased BUN may occur due to increased urea production by the liver, the intestinal tract, an excessively high protein diet, or a combination of any three.
However, decreased excretion of urea by the kidneys, is the most common cause of an increased BUN, and may be due to partial kidney failure, urinary tract obstruction, and or urinary tract infection.
It is generally believed that urea is relatively non-toxic, but other wastes that accompany increased BUN may cause toxicity and dehydration.
The method most used to treat the symptoms of an increased BUN is intravenous fluid therapy. However a urine specimen obtained prior to treatment, should be submitted for a complete urine analysis, including sediment examination.
Specific treatment of the underlying cause should be started as soon as possible.
URINE ANALYSIS
While a dipstick test is available for specific gravity, accuracy is not always as good as required, and sediment examination provides essential information on red blood cells, white blood cells, bacteria, casts, crystals and other cells in the urine.
Whilst specific gravity provides a good indication of the ability of the greyhound to retain water: Any specific gravity test, if looked at in isolation without considering the hydration of the dog, forced fluid intake such as extra water added to the meal, the addition of alkalising diuretics to the diet, or the effects of a recent run, may provide a misleading result.
Correct sample collection is also of extreme importance, a clean container must be used as any contamination, and even soap or detergent will alter test results.
It is also best, if first urine of the morning can be collected, and a midstream sample if possible, to reduce the chance of bacterial contamination.
Wiping the animal first with a clean tissue will also help in this regard.
It cannot be stressed enough that the sample should be tested when the urine is fresh, any sample left longer than 20 minutes should be refrigerated and tested within a few hours.
SPECIFIC GRAVITY Specific gravity 1.045 A specific gravity of this level and higher in dogs with slight dehydration indicates normal kidney function.
Specific gravity 1.045----1.030 In dogs with no medical problems and with normal hydration, BUN, and serum Creatinine, this range is considered normal. However, in dogs with dehydration and or a high BUN reading, this may indicate a slight loss of urine concentrating ability.
Specific gravity 1.029----1.013 Urine specific gravity in this range may be normal in dogs, when no need to concentrate urine exists. In greyhounds with dehydration however, further tests to check kidney function may be indicated, as in that case only slight ability to concentrate urine exists.
Specific gravity 1.012----1.008 No urine concentration has occurred in urine with this specific gravity, there again that may be normal in dogs with no need to retain water. However, if dehydration exists, values in this range are definitely abnormal, and a blood chemistry profile is indicated.
Specific gravity 1.008 Specific gravity at this range and lower may still be normal if the dog has a need to excrete extra water, but are abnormal if any dehydration exists, and would indicate the need for a blood chemistry profile, as well as a complete urine test, including sediment examination.
If these are normal, an Anti Diuretic Hormone response test should be carried out.
URINE pH Urine pH in greyhounds may vary each day, as the kidneys maintain and adjust electrolyte and acid-base balances, in relation to dietary intake, or a hard run.
Therefore, no specific urine pH is abnormal, except as it relates to other findings from urine analysis, and to the acid-base and electrolyte balance as a whole.
Urine pH 7.1 and lower Urine in this range is acidic or neutral, and because greyhounds are usually fed only one main meal each day, they generally have a pH in this range.
However, if the urine is markedly acidic (6.0 or lower) a systemic problem may exist, and further investigations should be undertaken.
Urine pH 7.0 and higher Alkaline urine may be caused by addition of excessive amounts of alkalising medications to the diet, however consistent alkaline urine may also be caused by a urinary tract infection.
Some of the types of bacteria that cause urinary tract and kidney infections produce an enzyme that breaks down to ammonia and turns the urine alkaline.
Consistent alkaline urine in dogs may also cause the formation of a type of kidney stone (crystals); these may also be caused by the indiscriminate use of sulphonamide antibiotics.
Another reason for persistent alkaline urine may be the inability of the kidneys to reabsorb bicarbonate.
Any consistently alkaline urine should be investigated, including a urinary sediment examination.
PROTEIN Protein in the urine is usually tested for by dipstick analysis; however this test does not provide for an accurate quantity of protein in the urine, nor are dipsticks capable of detecting some proteins in the urine associated with plasma cell damage.
Protein urine dipstick tests are qualitative and are recorded as a trace to 4+.
For the significance of protein in the urine to be accurately interpreted, the urine specific gravity must be known.
For example; a small amount of protein may read as negative in urine with a specific gravity of 1.010, but will read positive in urine concentrated to 1.045.
A small amount of protein in the urine is normal, providing the specific gravity is in the normal range for the state of the dog being tested, however any amount of protein in the urine at a specific gravity of less than 1.030 may be abnormal.
Blood in the urine can provide a false positive reading for protein in the urine, because proteins are present in blood in large quantities, compared with the amount of protein in normal urine.
There are a number of diseases that cause increased quantities of protein in the urine including kidney disease; therefore, any significant increase in protein in the urine should be investigated.
KETONES Any reading of ketones in the urine is abnormal, false positive reactions are uncommon but could occur in highly concentrated and pigmented urine.
Causes of a positive reading may include impaired liver function, persistent fever, and chronic diseases involving blood glucose levels.
GLUCOSE Normal urine does not contain glucose; therefore, any glucose reading is abnormal.
The most common cause of glucose in the urine is an elevated blood sugar to a level that exceeds the ability of the body to reabsorb the glucose; however this is extremely rare if not unheard of in greyhounds.
BILIRUBIN Some bilirubin in the urine of dogs is normal; however the amount of bilirubin should be compared with the urine specific gravity. A trace to 1+ of bilirubin in urine with a specific gravity above 1.035 is normal, any increase above this level is abnormal, and may indicate some degree of liver damage.
UROBILINOGEN Far too many problems exist in the measurement of urobilinogen using a dipstick test, and a false negative or a false positive result is common, and is therefore not recommended.
BLOOD A positive test to blood in the urine may indicate the presence of haemoglobin, myoglobin, or intact red blood cells. Any positive blood urine test warrants further investigation.
URINE COLOUR Urine is normally yellow to amber in colour, and depth of colour will depend on urine volume.
However, dark urine does not necessarily indicate that the kidneys are concentrating the urine in a fluid saving effort.
Red Coloured Urine The discolouration of the urine will depend on the type of pigment causing the discolouration and the urine pH
HAEMOGLOBIN in acid urine colours the urine a smoky brown while in alkaline urine the colour is red.
If a urine sample is to be checked for Red Blood Cells, it should be done as soon as possible after the sample has been collected, as RBC’s start to breakdown within minutes, releasing HAEMOGLOBIN into the urine. (HAEMOGLOBINURIA)
The presence of blood in the urine may indicate a variety of diseases ranging from kidney- nephritis, cysts or trauma, to infections in the bladder, urethra, prostate, or genital area. While HAEMOGLOBIN only in the urine may indicate a blood disease, bacterial infection, red blood cell parasites, or even some type of chemical poisoning.
Brown Red Urine MYOGLOBIN in the urine (MYOGLOBINURIA) is characterised by brownish red urine.
MYOGLOBIN is released from the muscle tissue following excessive exertion (RHABDOMYOLYSIS) or trauma such as torn muscle fibres.
The presence of MYOGLOBIN in the urine indicates the need for a thorough muscle check, and a blood test for muscle enzymes to rule out muscle disease.
MYOGLOBIN in the urine may also adversely affect the kidneys (toxicity), and the greyhound should receive intense fluid therapy.
Blood, Haemoglobin and Myoglobin, will all give a positive result to occult blood with a dipstick test.
SYMPTOMS OF ILLNESS
Because a simple loss of appetite may be the first symptom of further problems, the greyhound should be kept under close supervision.
Check the greyhound’s temperature twice daily, and if normal: Keep the greyhound warm and in a comfortable quiet environment. Provide a bland but nutritious meal such as cooked chicken broth and rice.
If the temperature is over 40 Celsius, or below 37 Celsius, seek Veterinary advice
(As a guide but not a hard and fast rule, a high temperature is generally caused by a bacterial infection, while a low temperature is often associated with a viral infection.)
VOMITING The definition of vomiting is the forceful ejection of fluid or food from the stomach.
Vomiting may be caused by gastro-enteritis, toxins or drugs, a foreign body in the gut, an obstruction in the intestines, an obstruction in the bile ducts, liver disease, acute pancreatitis, distemper, or something as simple as a severe case of travel sickness or a bad lot of meat.
Vomiting may be a sign of many different disorders, and if allowed to continue for too long will lead to severe dehydration and loss of electrolytes from the system.
First look at the severity of the vomiting. Vomited only once or twice, and vomited up only the recently eaten food.
This is likely to be caused by excessive bacteria in the food, or contamination of the food.
Symptomatic treatment; Take temperature, if high or low seek Veterinary advice.
Withhold solid food for 8 to 10 hours.
Provide clean cold water with ‘Vitrate’ or “Recharge” added at the rate of 80 ml per litre of water.
For the first two meals provide chicken broth, rice and toasted whole meal bread.
Vomiting every time any food or liquid is ingested. This requires Veterinary treatment rather than supportive home therapy.
Vomit is tinged with blood or smells like faeces. Seek urgent Veterinary advice.
DIARRHOEA The definition of diarrhoea is a change in the normal bowel movement, characterised by increased frequency and increased fluidity of motions, caused by an increase in faecal water, or an increase in gut secretions.
As with vomiting, diarrhoea may be a sign of many different disorders, and even more so than vomiting, can and will lead to severe dehydration.
Diarrhoea may be due to bacterial contamination of the food by Salmonella or E-coli causing gastro-enteritis, or something as severe as Parvovirus or Distemper.
Again look at the severity of the symptoms, and take the greyhounds temperature.
Moderate diarrhoea (no vomiting) Diarrhoea in the kennel first thing in the morning, and further loose stools when taken out for a walk, no other signs of illness
This type of diarrhoea is generally caused by a drastic change in the diet, or due to some contamination of the feed.
Withhold solid food for 8 to 10 hours
Provide clean cold water with ‘Vitrate’ added at the rate of 80 ml per litre of water
For the first two meals provide chicken broth, rice and toasted whole meal bread.
Diarrhoea and vomiting This is generally caused by a bacterial gastro-enteritis, and may require antibiotic and intravenous fluid treatment. Seek Veterinary advice.
Diarrhoea tinged with blood, or a jelly like diarrhoea with a particularly foul odour Blood in the stools may indicate a severe viral problem such as Parvovirus, or something as simple as a hookworm infestation, while a jelly like diarrhoea may indicate severe intestinal inflammation caused by toxin producing bacteria.
Seek urgent Veterinary advice.
PERSISTENT LOOSE STOOLS A persistent problem with loose stools (cow plat) requires further investigation; it may indicate such diverse problems as intolerance to wheat, lactose, brewers yeast, overgrowth of the wrong type of bacteria in the gut, or something as severe as liver damage.
LETHARGY, DEPRESSION Greyhounds are no different to you or me when it comes to feeling tired or down, when you are ill, have a dose of the flu, or a pain in the gut.
Any change in the normal behaviour of the greyhound should set alarm bells ringing for the trainer.
Take the greyhounds temperature.
Keep the greyhound under observation.
Reduce workload.
DEHYDRATION, DRINKING EXCESS WATER, DIFFICULTY URINATING, ABNORMAL URINE COLOUR, WEIGHT LOSS All of the above, if taken individually may indicate some type of stress either due to an excessively hard run, or a run while suffering from a bacterial or viral infection.
If taken all together, it means the greyhound has a severe case of acidosis.
Anyone of these symptoms will require investigating, and appropriate Veterinary treatment if the greyhound is to continue performing as required, if all of them are present seek urgent Veterinary advice.
DIFFICULT OR UNUSUAL BREATHING OR SEVERE COUGHING Any difficulty in breathing, any unusual sounds while breathing, or a deep hacking cough, require immediate treatment by your Veterinarian.
Under no circumstances allow the greyhound any running exercise while exhibiting any of these symptoms.
Keep the greyhound quiet and warm.
Isolate away from other greyhounds
Seek Veterinary treatment
Respiratory infections may lead to lung damage if left untreated, or the unusual breathing you hear may be due to severe tonsillitis, soft palate malformation, or even heart damage.
NASAL AND OR EYE DISCHARGE Nasal discharge may be due to kennel cough, or the eye discharge may be caused by a simple eye irritation.
However any discharge from the nose and eyes, in particular if it appears crusty, will require the immediate isolation of the affected greyhounds and urgent Veterinary advice, as this is one of the first symptoms of the Distemper virus.
Always insure all of your greyhounds have been correctly vaccinated, including any booster doses as required, and don’t bring greyhounds into your kennels that are not immunised
That way you may never have to worry about crusty nasal and eye discharge.
MUSCLE DAMAGE
It comes at no surprise therefore, that differently shaped racetracks may cause specific injuries to occur.
Muscle injuries, including ligament and tendon damage, are usually classified as stage 1-2 or 3 injuries, starting with severe strains as stage 1 through to torn or ruptured muscles at stage 3.
A number of books have been written about the injuries sustained by the racing greyhound and their treatments, in particularly one written by Dr. James R. Gannon, Dr Linda L. Blythe and Dr. A. Morrie Craig called "Care of the Racing Greyhound" is excellent for its concise and comprehensive coverage of the subject.
Anyone wishing to learn more about this subject, or indeed Greyhounds, would do well to purchase the same.
However, I would like to take a step back and look at the basic reason for muscle injuries occurring, other than those sustained during specific racetrack accidents.
You can run most greyhound’s solo on a safe track, on a safe surface, and after 4 or 5 runs these greyhounds will have sustained some damage to specific muscles.
Quite often there are also, what I can only describe as undesirable changes in the muscle structure.
These changes consist of the top edge of the muscle sheaths separating between various muscles or muscle groups that are normally joined together.
Such as the separation that often occurs between the bottom edge of the GLUTEAL and the top edge of the TENSOR FACIA LATA. This separation if left untreated, will eventually result in a torn groin that splits at the top edge of the PECTINEUS.
The only reason that these changes occur is due to the repetitive strain causing some muscles to tighten into excessive muscle tone.
The muscle still functions and contracts as normal, but is no longer capable of extending to its former length. Creating extra strain to the adjacent muscles or the attachment point of the muscle in question.
As mentioned earlier, muscles don’t only contract; they must also be capable of allowing the limb to extend fully. In fact the distance a greyhound is capable of stretching, has a direct bearing on how fast it runs.
And believe you me, the fact that you can stretch the greyhound’s legs out for him, has little relationship to the true picture that occurs when he has run for 200 meters or more and some of the muscles have tightened due to the strain.
In golf, the varying distances the ball will travel, depending on how well you follow through with the club is enormous, and yet the ball has already left the club surface.
To a certain extend, the same is true for a greyhound’s stride.
The foot has left the ground, but it is the follow through that dictate how far the Greyhounds body travels before the next foot touches the ground.
Treating excessive muscle tone after each and every run will minimise all of the muscle injuries, and maximise the greyhound’s speed.
EXCESSIVE MUSCLE TONE The muscles that are most vulnerable are those muscles that take most of the pressure as the greyhound drives around the turn or accelerates from the boxes.
Left Front Limb The centre section of the LONG TRICEPS tightens, and when the leg is fully extended this may cause strain and muscle sheath damage to the top attachment, and or the junction between the top and centre sections (egg or pin muscle).
On the forearm the PERFORATUS tightens and this reduction in flexion may cause damage to the tendons that flex the foot and toes.
Right Front Limb Again the centre section of the LONG TRICEPS becomes too tight.
However, any muscle sheath damage on this leg tends to be more severe due to the fact that on the turn the leg may slide slightly further forward, aggravating the strain.
This tightness in the shoulder will also cause the dog to place the leg in a slightly awkward position on the track, particularly on the turn, causing excessive pressure on the wrist joint.
And if severe enough, this may damage the ACCESSORY CARPAL LIGAMENT, the ANNULAR LIGAMENT, and or the PERFORATUS TENDON.
Left Hind Limb Because of the galloping style of the modern racing greyhound, this leg is the main driving leg when the dog runs on the straight sections of the track.
The main muscle of concern is the TENSOR FACIA LATA (triangle) this tightens and tends to split away from the GLUTEUS MEDIUS (hip support).
Also of concern is the rear edge of the BICEPS FEMORIS causing damage at its insertion.
However, the muscle that tightens and damages probably the most is the GRACILIS. Excessive muscle tone causes it to pull away from the SEMITENDINOSUS (hamstring) at the lower edge.
Right Hind Limb This leg takes most of the pressure when driving around the turns, and again the TENSOR FACIA LATA tends to tighten, pulling away from the GLUTEUS MEDIUS.
While the top edge of the GLUTEUS MEDIUS often tightens enough to cause the muscle to almost split in the middle.
Also on this leg the LATERAL VASTUS, which extends the stifle, will tighten sufficiently to cause damage at its uppermost attachment (origin)
As on the left hind leg, the rear edge of the BICEPS FEMORIS also tightens, damaging the lower attachment (insertion)
However, it is the GRACILIS on the right hind leg that generally sustains the most damage, more often than not, damaging the muscle sheath of the SEMITENDINOSUS in the process.
Also on the right hind leg, because of the pressure it takes on the turn, excessive muscle tone may reduce the function of the GASTROCNEMIUS and the PERFORATUS. This lack of elasticity may damage the tendon section of one or both, severely limiting the greyhounds racing career.
The other area of concern is the UPPER TRAPEZIUS (saddle muscle), excessive tension in this muscle will not only result in the front tip damaging, but may also cause the THORACIC section of the spine to lock up, often interfering with the function of the RADIAL NERVE.
All of these injuries reduce the speed and racing life of the greyhound, and all of them originally start with a muscle or section of muscle that tightens too much, can’t stretch fully and extend the limb comfortably.
The pressure of acceleration and driving around the turn does the rest.
There is no doubt in my mind that most of the muscle injuries sustained by the racing greyhound would be minimised if the greyhound received regular and thorough massage and physiotherapy, in particularly to those muscles most at risk.
It is a real pity that massage seems to have gone out of vogue, to be replaced by ultrasound and/or laser therapy only when the muscle finally breaks down.
LOCATING EXCESSIVE MUSCLE TONE and INJURY PROBLEMS Most people when they check a greyhound for injuries simply squeeze the muscle and wait for some type of pain response.
However, this is certainly not the best way to check for injuries, as a severe pain response is often caused by transfer pain from a spinal muscle spasm, or occasionally by the fact that the greyhound is severely stressed and has an excessive build up of toxins in it’s system.
There again, if your sense of touch tells you there is a problem with the muscle you are checking, slightly firmer pressure and a pain response will help to differentiate between a past problem or a current injury.
Because much of the muscle damage that occurs to the racing greyhound occurs in the surface of the muscle or muscle sheath, it takes very little pressure to detect.
Everyone can tell the difference between varying surfaces by lightly touching those surfaces, such as the difference between touching a bench top or a sponge, between a rough piece of cloth or a piece of silk.
In fact the harder you press, the less you are likely to feel.
Checking muscle tissue is much like that, with a little practice it is not difficult to feel whether or not a particular area of muscle is harder than the surrounding tissue, or the exact same muscle on the other side if the dog.
Excessive muscle tone does not normally, even with firm pressure, give you a pain response, and yet it is the start of most muscle damage.
When checking each leg for changes in muscle tissue it is important that the leg is supported lightly off the ground, and that all of the muscles in the area to be checked are relaxed.
MUSCLE TEXTURE AND LIKELY SIGNIFICANCE Sound healthy muscle tissue should feel firm, resilient, springy, and with a smooth even texture in the belly of the muscle, firming slightly near attachment points.
The Muscle Feels Ok Except it is a little harder on one edge. This is the start of a muscle developing excessive muscle tone.
TREATMENT: Massage daily until the hard area softens 50 firm strokes by hand, or 20 with a mechanical massager. Apply heat-producing liniment after completion of massage.
The Muscle Feels A Little Harder All Over This is likely excessive muscle tone, unless of course it feels stringy and rough, in which case the problem is older, and there is some scarring. However, the same treatment will benefit both problems.
TREATMENT: Ultrasound twice daily for 2 days, then treat as above, except for the heat producing liniment if the problem is scar tissue.
In that case a product such as LASONIL made by BAYER best replaces the liniment.
The Muscle Feels Hard/Tight All Over With some heat and pain response, but no fluid or swelling. In this situation the problem has gone a little further, and there is likely some strain to the muscle fibres
TREATMENT: Ultrasound twice daily for 3 days, rest 24 hours, then contract for 1 minute daily for 3 days using the BURST setting on a TENS unit.
Apply a heat-producing liniment after each contracting session.
The Muscle Feels Hard All Over Except for a distinctly softer or hollow section at one end, or in the belly of the muscle
In this case there is some muscle fibre disruption and damage within the muscle structure.
If there is fluid or swelling, ice or cold pack twice daily until the swelling is relieved before any other treatment is undertaken.
In a situation such as this, a decision needs to be made whether or not the damage is severe enough to require strengthening by injecting a sclerosing agent such as MUSCLE REPAIR or PROMOTE.
Keeping in mind that the resulting scar tissue may reduce muscle flexibility.
TREATMENT: If the damaged area is to be injected this should be done first.
Using a 1 ml syringe with a 29-gauge needle, inject 1/10th of 1 ml at 10 mm centres into the central area of the damage to approximately 10 mm below the skin.
Then inject 1/10th of 1 ml at 10 mm centres keeping approximately 5 mm inside the damaged area, angling the needle to place the injection 5 mm below the skin.
Do not inject into the harder area of surrounding muscle tissue.
Rest for 48 hours then use ultrasound treatment, first daily for 2 days, then twice daily for 3 days and again daily for a further 3 days, the first 2 treatments at a maximum setting of 0.8 watts.
After the completion of ultrasound treatments, rest a further 48 hours before starting TENS contracting treatments. After each TENS treatment the area should be massaged and stretched by the appropriate limb movement.
Excessive Separation To Muscle Sheaths When excessive separation occurs between muscle sheaths, again the decision will need to be made whether or not to strengthen the attachments between the muscles in question.
The problem in this case consists of the fact that this separation would probably not have occurred, if the muscles involved were capable of stretching properly in the first place.
Under these circumstances, the treatment would be better limited to ultrasound treatment, massage, and physiotherapy only. Simply because the creation of scar tissue may result in one of the muscles tearing eventually.
However, there is sometimes a case for increasing the strength of the muscle sheaths on both sides and at each end of the separation, particularly if the injury has been treated appropriately with Ultrasound, and after further exercise, it continues to keep splitting deeper and further.
In this situation inject 2/10th of 1 ml at each end of the split and continue injecting both sides at 10 mm intervals with 1/10th of 1 ml approximately 2 mm inside the muscle sheath, using the appropriate sclerosing agent such as Merolin (Ethanolamine Oleate 5%). Effectively buttonholing around the area leaving the centre capable of stretching if required.
Following up with ultrasound and physiotherapy is essential
INJURY TREATMENT GUIDELINES
Excessive Muscle Tone With No Pain Response Hand massage a minimum of 50 firm strokes, or 1 minute of light finger kneading 2x daily for 3 days, or a mechanical massager 20 firm strokes 2x daily for 3 days.
Excessive Muscle Tone With Pain Response Treat as for above + apply heat producing liniment after each treatment.
Slight Inflammation With Pain Response TENS treatment for 1 minute daily for 3 days using very gentle contractions only, apply heat producing liniment after each treatment.
Or Muscle Contractor (Faradic Current Stimulator) treatment consisting of 20 gentle contractions daily for 3 days, + apply heat producing liniment after each treatment.
Inflammation With Pain Response Ultrasound treatment consisting of 2 treatments on day 1 at 1.2 watts for 3 minutes, 2 treatments on day 2 at 1.8 watts for 5 minutes, 2 treatments on day 3 at 1.8 watts for 5 minutes, then TENS or Muscle Contractor treatment as above for the next two days.
Drug Therapy For Stage 1 Injuries On occasion the need may arise for the Greyhound to perform within 3 days of the diagnosis of a stage 1 injury, not allowing for more conventional methods of therapy to heal the injury.
In this situation the use of 1 ml of ATP (Dynacleine or Enerzyme, I prefer Enerzyme as it is far less painful to inject) combined with 0.1 ml of Adequan, and injected into 4 evenly distributed areas of the affected muscle, will get the Greyhound to the track and performing.
A word of warning, the excessive use of this method of injury treatment will cause a reduction in the muscle size, and a reduction of the muscle's ability to handle continuing strain. This type of treatment should always be followed with TENS or Muscle Contractor treatment after the race.
STAGE 2 INJURIES These range from a small tear in a muscle sheath, to excessive separation of the muscle sheath or fascia between two muscles.
In each case the initial treatment will be to relieve any swelling, so that the full extend of the injury may be diagnosed.
If at that point in time, it is discovered that the tear or split is in excess of 2.5 centimetres for separation between muscle sheaths or in excess of 1.5 centimetres in a muscle sheath. Veterinary advice should be sought, as this amount of damage may be best treated with surgery.
Healing by fibrosis, using a sclerosing agent (5% MONO-ETHANOLAMINE OLEATE) or (3% SODIUM TETRADECYL SULPHATE).
Important! Never inject a sclerosing agent into a damaged muscle while there is still some inflammation present, as this will result in the excessive formation of scar tissue.
Using a 1 ml syringe with a 29 gauge needle inject 1/10th of 1 ml at 10 mm centres around the edge of the damage, angling the needle to place the product 5 mm below the skin.
Ice pack 3 times daily for the first 48 hours, then rest for a further 24 hours prior to starting Ultrasound treatments.
Ultrasound treatment, first daily for two days at 0.8 watts, then 2 x daily for 3 days at 1.2 watts, then further daily treatments for 3 days at 1.8 watts, rest the area a further 48 hours before starting TENS or Muscle Contractor treatments.
After each TENS or Muscle Contractor treatment the area should be massaged with LASONIL and stretched by the appropriate limb movement.
STAGE 3 INJURIES If you are unfortunate enough for your Greyhound to suffer a torn muscle, cold pack as soon as possible to reduce the swelling and seek urgent Veterinary advice.
THERAPEUTIC TREATMENT DEVICES
CURRENTLY AVAILABLE THERAPEUTIC TREATMENT DEVICES
ULTRASOUND
Ultrasound treatment is one of the most widely used methods of repairing soft tissue injuries.
The high frequency sound waves (1000 MHz) that radiate from the applicator head produce both heat and a micro massage effect within the muscle fibres, and the heat so produced dilates the blood vessels, while the micro massage effect breaks up blood clotting.
The frequency of the sound wave produced is extremely important, because at 1000 MHz it has a penetrating ability of around 6 centimetres or more (2-½ inches), while at a frequency of 3000 MHz this penetrating ability is reduced to 1 centimetre (1/2 inch).
Limitations
The use of ultrasound is strictly limited to the treatment of soft tissue injuries, such as damage in muscle tissue, tendons and ligaments.
Contraindications
Ultrasound radiation should never be used for the treatment of bone fractures as it produces excessive heat on the bone surface, creating extreme bone pain, and the likelihood of permanent damage to any muscle or tendon attachment at the radiated area.
The use of ultrasound treatment too soon after the occurrence of an injury may increase internal bleeding at the injury site.
The excessive use of ultrasound produces a feeling of fatigue, and should not be used within 24 hours of racing.
PULSED MICROWAVE
Pulsed microwave may be used in all types of injuries where the application of deeply penetrating heat is deemed to be beneficial, and may be used for both soft tissue damage, and bone fractures.
Limitations
Because the heat produced by the pulsed microwave covers a large area, it also radiates the sound tissue around the injured muscle, limiting its use to a general treatment of soreness due to stage 1 injuries, and minor bone fractures.
Contraindications
Due to the fact that microwave radiation has been linked to various types of cancer, and the danger this represents to both the patient and operator, the use of microwave radiation as a therapeutic treatment tool has largely been discontinued for general medical use.
The heat produced by the pulsed microwave has a tendency to “cook” or “dry out” the muscle tissue, and therefore its use should be limited to one treatment every 24 to 36 hours.
The use of microwave radiation over large areas of the body produces a feeling of extreme fatigue and debility, and should not be used within 48 hours of racing.
LASER
Since its introduction as a therapeutic treatment device, laser treatment has been surrounded by a great deal of “hype”, and it is “reputed” to be able to treat anything from a torn muscle to a sore tooth.
Unfortunately some of its treatment reputation is unwarranted; however the use of laser therapy is beneficial in all areas where stimulation of healthy cell growth is required.
This includes all soft tissue injuries, trauma on the skin surface, the bone periosteum, as well as reduction of fibrosis tissue and scar tissue.
Laser therapy seems to be more effective when used around 48 hours after an injury has been injected with a sclerosing agent. The sclerosing agent stimulates rapid scar tissue formation, and while this is occurring, laser therapy appears to improve healthy cell growth rather than scar tissue.
Limitations
Because of the fact that the laser treats such a small area at each application (about the size of a ten cent piece) and the requirement that sufficient energy needs to be absorbed into each area, laser treatment can be quite time consuming.
Therefore its use tends to be limited to the treatment of tendon and ligament injuries.
While the cost is still high, the advent of multi head laser units has certainly improved the use of laser therapy for larger soft tissue injuries.
It should however be clearly understood that the effectiveness of laser is dependent upon the output of each laser diode. For effective healing it is accepted that an absolute minimum of 2 Joule of energy (preferably 4) is delivered to the injury site in each treatment.
One joule of energy is delivered by a 1000 milliwatt laser in one second. Therefore a 100 milliwatt laser will take 10 seconds to deliver the same amount of energy.
Purchasing a cheaper 30 milliwatt laser can therefore be poor economy, as this laser will take 66 seconds, or just over one minute to treat an area the size of a ten cent piece with the minimum required 2 joule of energy.
Contraindications
There are currently no known contraindications to the laser as a therapeutic device.
PULSED MAGNETIC FIELD
As for laser, the original introduction of pulsed magnetic field as a therapeutic treatment device was surrounded by a great deal of unwarranted “hype”.
Pulsed magnetic field may be used in all soft tissue areas where a low level of blood flow stimulation may be beneficial, such as in a “tying up” syndrome, or in those Greyhounds that suffer from tightness and excessive muscle tone all over the body.
However it is in the treatment of bone trauma that pulsed magnetic field treatment really is worthwhile, as its most beneficial effect is on the bone matrix, where it at least halves normal healing time.
Limitations
The use of pulsed magnetic field to treat minor muscle trauma is simply not worthwhile, a good liniment will have a similar beneficial effect.
Contraindications
It has been reported in the media that pulsed electromagnetic fields have been implicated in causing cancerous brain tumours
Due to the fact that magnetic field has a greater effect on the kidneys than muscle tissue; excessive use may lead to loss of electrolytes from the body.
INFRARED HEAT LAMPS
Infrared heat may be used in all areas where low level penetrating heat is deemed beneficial.
Limitations
The use of heat only on muscle tissue has a minimal beneficial effect, unless it is combined with massage.
Infra red heat lamps have a limited penetrating ability.
Contraindications
The use of heat alone on damaged muscle tissue may lead to excessive scar tissue formation.
The use of an infrared heat lamp too soon after incurring muscle trauma may increase internal bleeding.
The use of an infrared heat lamp may cause excessive heat on the skin surface.
If liniments are to be applied they must be applied after the treatment is completed, not before
THERAPEUTIC TREATMENT GUIDELINES
THERAPEUTIC TREATMENT GUIDELINES
LASER AND LASER TREATMENTS
The word Laser Stands for Light Amplification by Stimulated Emissions of Radiation.
Laser light is produced by exciting atoms in such a manner that they collide with each other. During this collision in the excited state, each atom releases photons; some of these photons lock together and travel in the same direction, wavelength and frequency.
Thus by exciting a specific substance and producing a chain reaction of the atoms, a coherent light is produced; this phenomenon is called Stimulated Emission.
This Light is then Amplified by refocusing it into a tight beam and allowing it to Radiate out.
When a laser beam is applied to living tissue it produces both a thermal, and a photochemical reaction.
The ability to focus the laser beam into a tightly controlled area, and the thermal cell destruction phenomena, are being used successfully in both major surgery, and plastic surgery.
Sophisticated techniques have been developed using high intensity lasers that have a considerable advantage over conventional surgical methods by reducing scarring, and by providing better control over bleeding.
Photochemical reactions follow the application of low energy laser beams, and consist of the reactions that occur when the cells take in the light energy, and incorporate this into their metabolic processes.
The intake of laser light causes the cell mitochondria to produce more energy, thus stimulating cell replacement, it increases ATP production providing more useable energy, and it causes a reduction of nerve cell excitability, providing instant reduction in pain and inflammation levels.
The energy produced by the laser light is measured in Joule, 1-Joule equals the energy produced by a 1000 mw laser in 1 second, or the energy produced by a 10-mw laser in 100 seconds.
Therefore a 4-joule treatment with a 30-mw laser will require 2 minutes and 15 seconds.
It is also important that the laser tip is held stationary on the treatment area; this reduces laser light loss, and maintains penetrating ability.
Treatments
For a worthwhile healing effect of muscle or ligament damage, and depending on the type of injury being treated, it is generally accepted that 2 to 8 Joule of laser energy needs to be absorbed by each 2x2 cm area of tissue at each treatment session.
Therefore the time spent treating each area depends entirely on the output of the laser.
Most injuries will require from 10 to 20 treatments.
It should also be noted that the joule output as described is based on a laser with a continuous beam, not a pulsed beam, as this dramatically reduces the joule output.
Acupuncture
Low output lasers are especially effective for acupuncture treatments, as each treatment spot only requires 0.5 joule of energy absorption.
Safety
Lasers emit powerful light radiation that can damage the eye retina, never stare directly into the laser beam, or allow others to do so.
All persons within the treatment area should wear suitable eye protection.
Allow laser treatment only when the hand piece tip is pressed firmly onto the treatment area.
Remove highly reflective surfaces from the treatment area, such as stainless steel fittings and mirrors. Do not allow anyone, especially children, to play with a laser.
APPLICATION NOTES FOR ULTRASOUND THERAPY
Ultrasonic therapy is the principle of applying waveform energy at frequencies above the normal range of hearing, but lower than radio frequencies.
Ultrasonic therapy uses a frequency of one million cycles per second (1 megacycle).
Normal range of hearing ceases above 20,000 cycles per second.
Ultrasonic energy penetrates body tissues to a depth of 5 cm or more, and affects the tissues in three ways simultaneously, thermally, mechanically, and chemically.
Thermally, the energy is transformed to heat, increasing blood flow and stimulating healing.
Mechanically, it has a stirring action within the tissue, providing a cellular micro massage effect.
Chemically, it increases cellular permeability and the diffusion of ions into and out of the cells.
The blood supply and lymph drainage are improved, more than by the application of heat alone.
In inflamed tissues, acid breakdown products are drained away.
Muscle spasms and pain are relieved in skeletal muscle, ligaments and tendons.
Ultrasonic therapy is normally applied utilising two different types of output; they are continuous wave, and pulsed wave.
The use of continuous ultrasound is generally limited to cases where the major aim is to deliver heat to the muscle tissue, or in large muscle bulk that is capable of absorbing the heat so produced.
Treatment with pulsed ultrasound reduces the heat effect, but enhances the micro-massage effect.
Pulsed ultrasound is best employed when treating small muscle areas, or when ultrasound treatment is undertaken to ligament or tendons, as in most instances this treatment will involve radiating the bone under the ligament or tendons.
When continuous ultrasound is used for this type of treatment it increases the chance of causing periosteum (bone) pain.
Each pulse of ultrasound energy consists of a large number of individual vibrations, which cause specific reactions to occur within the tissue, these reactions remain, until the next pulse arrives.
It is therefore unnecessary to increase power or exposure time, when pulsed beams are used.
Cautions In Ultrasound Therapy
Always use a good coupling agent such as a quality clear ultrasound gel, the addition of any type of liniment to the coupling medium is totally contraindicated.
For two reasons:
The addition of any particles to the coupling agent will reflect some of the energy produced by the ultrasound back into the ultrasound head, increasing the temperature of the face plate, and increasing the chances of damaging the barium titanite crystal.
Liniments are formulated to produce heat on the surface of the skin, and contain ingredients that may cause either kidney or liver damage when the ultrasound energy punches them through the skin and they have to be excreted from the body via the blood stream and the internal organs.
Over-Dosage
Of ultrasound produces a general feeling of fatigue and debility, which may also be accompanied by headaches and nausea.
It is therefore not a good idea to treat your Greyhound with ultrasound therapy in the 24 hours prior to racing.
Selection Of Dosage
It is desirable to always use the smallest effective dosage; the use of a short high dose is not equivalent in effect to a longer period of low dosage.
In general start with a low intensity 0.8 to 1.0 watt per cm for fresh injuries, and in subsequent treatments increase the dosage slowly to a maximum of 1.8 watts per cm.
Deep Seated Injuries
Due to the absorption in the tissues, ultrasound energy decreases with depth, after penetrating a tissue layer of 5 cm the intensity is reduced to half of its original value.
For deep-seated injuries when the power of the output needs to be increased to 2.0 watts per cm it is best to use a pulsed output to reduce the heat in the upper layer of muscle.
Should the head of the ultrasound unit get hot?
Not more than a comfortable body temperature, if the head gets hot there is something wrong with the unit.
Always unplug the ultrasound unit when not in use, or at the very least turn off the power point, it is far to easy for the unit to be turned on accidentally and burn out the face plate.
TENS APPLICATIONS
T.E.N.S this abbreviation stands for Transcutaneous Electrical Nerve Stimulation, the term Transcutaneous simply meaning “through the skin”.
TENS treatment utilises short electrical pulses that are designed to penetrate the skin and travel along the nerve pathways to the brain.
The main function of this is to interfere with the pain impulses that travel along the same pathways, providing pain relief for many chronic problems.
However a considerable body of evidence exists that indicates that the electrical pulses produced by the TENS also stimulate healing in damaged muscle tissue, and in damaged bone surface.
Pain Relief
An analgesic reaction may be achieved by setting the unit switch to NORMAL, the FREQUENCY to 100 and INTENSITY to 5.
Position one ELECTRO PAD on each end of the painful muscle or joint.
Treatment time is 30 minutes or more, and may result in a pain control period of 6 to 36 hours.
Caution, the masking of pain prior to strenuous exercise may result in a more severe injury.
To Accelerate Healing
Place the 4 ELECTRO PADS close around the injury site, with the pads of each pair being placed directly opposite each other. The field of maximum stimulation is central to each pair.
Set unit switch to NORMAL, FREQUENCY to 100 and INTENSITY to 5.
Treat for 10 minutes twice daily for 3 days, and then treat as for severe muscle strain.
Severe Muscle Strain
Place one ELECTRO PAD of a pair at each end of the muscle to be treated, set unit switch to NORMAL, FREQUENCY to 4 and slowly increase INTENSITY until a slight twitching movement is noted in the muscle being treated. Treatment time is 1 minute for the first treatment and 3 minutes for the next two daily treatments.
Thereafter treat as for general muscle strain.
General Muscle Strain
Place one ELECTRO PAD of a pair at each end of the muscle to be treated, set unit switch to BURST, and slowly increase INTENSITY until full but comfortable contractions are achieved.
Treatment time is 1 to 3 minutes twice daily for 3 days.
Treatment should be comfortable for the patient, if any signs of pain or discomfort are noted REDUCE INTENSITY, check setting, and resume treatment at a lower setting.
Electro Pads
It is vital to ensure good electrical contact between the pads and the area being treated. This is best done using a good conductive clear ultrasonic gel.
After each treatment rinse pads in warm water, and allow to dry.
Please Note
There are a large number of different brands and types of TENS treatment units on the market, and the controls may vary to the examples given. However it is essential that the unit design include a burst setting, as this is the only setting suitable for muscle re-education or contracting.
WHY TENS TREATMENT?
The Greyhound is racing over 515 meters and hurts itself, and you treat the injury with an ultrasound or laser until the damage is repaired. Unfortunately at this point in time, the rest of the Greyhound is capable of running over 515 meters, except the muscle you have treated and healed.
The healed muscle does not have the muscle tone to stand up to racing over the same distance, and you have two choices. Either give the Greyhound 2 or 3 runs over a shorter distance until the muscle tone in the healed muscle catches up with the rest of the body, or you follow up the ultrasound or laser treatment with either muscle contractor treatment or TENS treatment and re-tone the muscle.
Failure to do this is the main reason the same muscles keep breaking down run after run.
SPINAL MUSCLE SPASM
The brain via the spinal cord, supplies every muscle and internal organ with the signal to affect normal function, and receives signals back including those in the form of a pain response. Spinal muscle spasm and spinal compression may interfere with those signals.
We worry about wrist joints, hock joints, shoulder joints etc. and yet, counting from the base of the skull and including the very top tail segments, there are about 30 joints in the spine that, if damaged, can seriously interfere with the way a greyhound gallops.
The muscles of the spine are one of the largest and hardest working muscles in the body, and have a considerable effect on how well the greyhound stretches out and how fast it runs.
Carefully examining the spine is just as important as checking the limbs, wrists and toes.
The fact that you can bounce his spine up and down without the dog collapsing in pain means absolutely nothing, when it comes to detecting spinal or spinal muscle damage.
Each spinal segment must be checked individually for soundness and stability, including any referred pain it may be causing.
In fact, referred pain provides a good guide to the location of the problem, and the type of therapy or spinal adjustment that is required to relieve it.
However, simply relieving a spinal muscle spasm does not cure the problem, a muscle spasm indicates damage to the tissue and requires follow up treatment, like any other muscle injury.
I find it rather disconcerting that people who have a “crook back” will go to a Chiropractor for relief, and afterwards will hobble around in pain (sometimes for weeks), and yet expect a greyhound to run like a champion the day after having a spinal problem treated.
A specific spinal spasm across a specific spinal segment or groups of segments will have an effect on a specific muscle or muscle group.
This effect may include: excessive muscle tone, reduced muscle tone, reduced muscle volume (Muscle atrophy) and reduced reflexes.
It may also cause an exaggerated pain response in specific muscles or bone surfaces when they are checked for injuries, (that is, excessive pain in relation to the amount of pressure being placed on the area) and severe pain on flexion or driving pressure on the affected limb.
Severe spinal compression at the LUMBAR segments L4 – 5 may affect bladder control.
Voluntary movement requires control by the brain; a long-standing and severe spinal problem may also cause some uncoordinated movement. However, uncoordinated movement is generally caused by a far more severe problem such as spinal lesions or brain damage.
What I have listed next are the main nerve pathways in the CERVICAL (neck), THORACIC (upper spine – saddle area), LUMBAR (coupling area) and SACRUM (lower back) and the spinal segments that may be affected by compression and muscle spasm, as well as the main muscles that these nerves control and the possible effect on the greyhounds stride.
For the location of the various spinal segments in relation to the greyhound’s structure, see the drawing covering the general BONE STRUCTURE of the greyhound.
NERVE | COMPRESSED AT | AFFECTED MUSCLES | FUNCTION | EFFECT ON STRIDE |
Suprascapular | C6 – C7 | Supraspinatus | Extends shoulder | Slight loss of shoulder extension |
| Axillary | C6, 7, 8 | Deltoid | Flexes shoulder | Decreased shoulder flexion |
| Musculocutaneous | C6, 7, 8 | Biceps | Flexes elbow | Decreased elbow flexion |
| Radial | C7 – T1 | Triceps | Extends elbow carpus & toes | Decreased triceps strength |
| Median | C8 – T1 | Flexor Carpi Radialis | Flexes carpus and toes | Decreased flexion |
| Ulnar | C8 – T1 | Flexor Carpi Ulnaris | Flexes carpus and toes | Decreased flexion |
| Lumbosacral | L4 - 6 | Quadriceps | Flexes hip and extends stifle | Loss of extension |
| Obturator | L4 - 6 | Adductor | Adducts Pelvis | Lack of sideways control |
| Sciatic | L6 – S2 | Biceps Femoris | Extends hip and flexes stifle | Decreased flexion of stifle |
| Tibial | L6 – S2 | Gastrocnemius | Extend hock and flexes toes | Decreased extension and flexion |
EXAGGERATED PAIN RESPONSE (REFERRED PAIN)
A severe pain response in a muscle or on some bone surfaces without the presence of contributing factors such as bruising, muscle fibre disruption, fluid etc. or an inflammatory reaction on the bone surface generally indicates a sensitised nerve pain response.
The basic explanation is this: the touching sensation is transmitted to the brain along the nerve pathway, picks up pain at the site of the spinal spasm, and registers as pain only.
In fact, a recent and severe muscle injury that includes muscle fibre disruption will exhibit a lower pain response than most sound muscle tissue when squeezed.
Simply because the disruption of muscle fibres also disrupts the nerves that conduct sensations, and the initial release of fluid into the area also contains some natural pain killing substances.
It is not unusual for a greyhound to finish last in a race and to be sent to the track Veterinarian by the stewards for an examination, and to be given “the no apparent injury” by the Veterinarian.
Only to turn up the next day with an obvious injury, such as a torn GRACILIS or a severely damaged SEMITENDINOSUS much to the disgust of the trainer, who then blames the Vet. for not finding the problem on the night.
All I can say is, the Veterinarian never had a chance, fresh injuries like that, unless they fill with fluid immediately are extremely difficult to detect, particularly on a greyhound straight off the track.
This can make checking for injuries extremely difficult, on the one hand you have severe pain response in an area that does not contain an injury (referred pain), on the other hand you may have a severe injury that may provide an extremely low pain response (torn muscle)
A good case for learning to check for injuries by touch rather than by pain response only
EXCESSIVE PAIN IN THE FOLLOWING AREAS MAY BE CAUSED BY A SPINAL MUSCLE SPASM.
Lower part of the CEHALO-HUMERAL (base of the neck), compression to C5/C7
Upper part of the PECTORALIS MAJOR (chest coupling), compression to C6/C7
Lower part of the PECTORALIS MAJOR (chest muscle), compression to C7/T1
DELTOID along the edge of the SPINE OF THE SCAPULA, compression to C7/T1
BICEPS in the body of the muscle, possibly due to compression to C7/T1
Wrist flexion, possibly due to compression to C8/T1
Medial surface of the lower RADIUS, compression to C8/T1
Upper TRAPEZIUS (saddle muscle), compression to T1/T2
In the junction between the LUMBO-DORSAL FACIA and LATISSIMUS DORSI, compression to L3/ L4
In the junction of LUMBO-DORSAL FACIA and the crest of the ILIUM, compression to L5/L7
In the lateral surface of the TIBIA just below the level of the PERFORANS, compression to L4/L5
In the lateral lower surface of the POSTERIOR SARTORIUS, compression to L6/S2
In the lower edge of the GLUTEUS MAXIMUS, compression to L6/S2
In the GASTROCNEMIUS, compression to L6/S2
In the rear of the TARSUS – METATARSUS junction, compression to L6/S2
Pain on fully extending the front leg, possibly due to compression to C7/T3
Pain on fully extending the rear leg, possibly due to compression to L5/S2
All of the above referred pain problems would benefit from spinal adjustment.
However, this is a specialised field, and unfortunately takes a considerable amount of practice and learning.
To simply rotate or twist the neck or spine of the greyhound in the vague hope that it may fix the problem, is dangerous to say the least.
Inexperienced and/or rough treatment, more often than not will cause a spasm in other parts of the spine or neck, or worst-case scenario, damage the spine permanently.
Under no circumstances should any spinal adjustment include sharp forceful downward pressure with the hand, as this may damage the area each side of the spinal segment being forced downward.
It is extremely important that any adjustment to a compressed nerve be done one spinal segment at a time.
Many of the spinal spasm problems of the greyhound would be far better treated and relieved by heat, thorough massage, gently stretching and more massage than by rough or inexperienced manipulations.
SPINAL ADJUSTMENTS
Unfortunately, this is not the case with spinal adjustments in racing greyhounds, where the practitioners are mainly self-taught, nor do they ever get together to share techniques for the betterment of all, a damn pity.
So it remains an inexact science practised by amateurs with varying degrees of proficiency.
Humans can clearly describe to the Chiropractor the problems they have, while the unfortunate greyhound has to rely on the individual manipulator to find the problem.
The damage in the human spine is generally caused by spinal disk compression due to lifting heavy weights awkwardly, or simply wear and tear; after all we do walk on our hind legs.
The damage to the greyhounds spine is generally caused by a sudden awkward movement, such as grabbing the lure only to have it continue on, or stop suddenly, falling during a race, or twisting sharply at the end of a straight run.
Incidents such as these cause muscle spasm and nerve compression, not weight bearing disc compression.
Some similar manipulation movements may be employed in greyhounds as in human chiropractic, but that is where the comparison stops, it is a completely different science with different manipulation techniques.
In the next section I will attempt to describe the basic movements to be made when releasing a muscle spasm, and my reasons for doing it a certain way.
It is difficult to accurately describe in print the amount of pressure or the movement required to successfully relieve a muscle spasm across a spinal segment.
This relies on the experience, finesse, and touch of the practitioner, and the state of the dog.
In each instance, the movement as described is made until slight resistance pressure is felt. Then with a very slight but firm flick in some instances, or with a little extra movement of pressure in others, the spasm is released.
In most instances, a popping sound may be heard signifying the joint releasing.
However if the tissue around a joint is severely inflamed, no sound will be heard, and there is a chance that any manipulation, while temporarily relieving the symptoms, will be unsuccessful in the long term.
All areas with inflammation must be allowed to settle, prior to any adjustments being made.
If you believe the adjustment was not successful, do not have a second go while holding the dog in the manipulation position.
Allow the dog to relax, re-massage, and then try again if necessary.
Important
Do not attempt spinal manipulation without a valid reason.
Under no circumstances should spinal manipulation be attempted if there is swelling or fluid on any part of the spine.
Do not attempt spinal manipulation if the dog has eaten its main meal within the last 4/6 hours.
Do not attempt spinal manipulation unless the dog has been properly emptied out.
Do not attempt spinal manipulation if the problem is severe enough to cause paralysis or partial paralysis of any limbs; this requires X rays and qualified Veterinary treatment.
Do not attempt spinal manipulation if the greyhound exhibits more than three classic signs of referred pain.
Any spinal segment to be adjusted should be thoroughly massaged, and/or warmed prior to any manipulation.
Using hot towels plus at a minimum 1-minute of firm deep finger massage on both sides of the spinal segment to be adjusted, or preferably a minimum of 20 firm strokes with a suitable mechanical massager.
At the completion of this preparatory treatment recheck the referred pain, in some instances just heat and massage only may relieve the problem, if it does, continue with heat and massage daily for at least 3 days prior to running the greyhound again.
I believe it is essential that every effort must be made to make the dog as relaxed as possible.
All spinal manipulation relies to a large extend on feedback from the dog prior to, during, and after the adjustment, and again every effort should be made immediately after any manipulation to reassure and relax the dog.
It is also important that the adjustment technique is designed to support the dog comfortably but firmly, in order to avoid sudden movement by the dog that may nullify the adjustment being undertaken.
At the end of each adjustment release the head, neck or limb immediately.
Spinal adjustments done correctly may cause some discomfort, but never severe pain.
If it appears to hurt severely, you are not doing it right.
To adjust C6 – 7 with pain on the left side Straddle the animal, placing your knees just in front of the last rib and supporting the animal firmly with your legs, hold the base of the neck with the left hand at, and just below the C7 level. With the right hand hold the muzzle of the dog, and firmly with a smooth continuous motion; bring the head and neck around to the right, in a very slightly downward under and upward direction, finishing with the head pointing almost towards the rear of the dog.
For pain on the right side, use the same procedure on the left side of the dog.
To adjust C7 – 8 with pain on the left side Again straddling the dog with both legs, this time just behind the last ribs, bend over the dog and bring your right hand around the right side of the trunk, and in between both front legs.
The right hand then grips the front and outside of the lower end of the left shoulder blade just above the HUMERUS, and lift the front of the dog off the ground.
This will allow the body and neck to tilt to the left, then using your left forearm halfway up the neck bring the neck around in a smooth continuous motion to the left and under, pointing the head towards the middle of the back legs.
For pain on the right side use the same procedure on the right side of the dog.
To adjust C7 – T1 with pain on the left side To complete this particular adjustment successfully you will require assistance.
Again straddle the dog, with your legs firmly holding the dog just at the last ribs.
Place your assistant at the front of the dog, have them hold the dogs left forearm just above the wrist with the left hand, bringing the leg up so that the forearm is horizontal.
Have them place their right hand on the dog’s elbow and push the elbow slightly towards the body, and then pull the leg slightly forward, so that the shoulder blade is approximately at a 45-degree angle.
Then place the four fingers of your left hand (with the fingers level at the tip) in between the top of the shoulder blade and the trunk, with the palm of your hand against the shoulder blade, and your fingers curled over the top of the blade.
Use your fingers to hold the blade slightly away from the trunk, with your palm supporting the blade, and holding the dog steady.
Place your right hand around the dogs’ upper muzzle with your thumb straddling the head, and in a smooth continuous motion rotate the head and neck to the right in a downward under and upward direction, finishing with the head almost pointing to the rear of the dog.
For pain on the right side use the same procedure on the right side of the dog.
To adjust T1 – T2 Straddle the dog with your legs placed around the rib area, bend over the dog and place your elbows on your knees, and link both hands under the dog’s breastbone to the rear side of centre. By rocking backward in this position, you can comfortably lift the front of the dog off the ground.
Place the tip of your chin in between T1 and T2 and while rocking back and lifting the front of the dog, place firm sharp pressure downward and slightly forward in between the spinal segments, using your neck and chin. Then re-massage to avoid a rebound spasm.
General spinal rotation is often practised in an attempt to cure a spinal muscle spasm in the LUMBAR region of the spine.
There again, I am not in favour of rotating the whole of the spine in order to relieve one or two spinal muscle spasms.
All muscle spasms are the result of some type of physical trauma; quite often a spinal rotation will duplicate the type of twisting that caused the problem in the first place.
It is impossible to gauge the total effect of the rotation until at least 24 hours later. It will appear OK immediately after the adjustment, just the same as the dog will appear all right when coming off the track, and it is not until 24 hours after the run that the worst of the problems become obvious.
You cannot get out of using rotation on the neck of the dog, nor can you avoid rotation if you have to work on the SACRUM – PELVIC area, however, indiscriminate spinal rotation should be avoided whenever possible.
That is why I have used the chin procedure on the THORACIC spinal area, and advocate the following adjustment method on the LUMBAR section of the spine.
It may seem weird to use your chin to free a spinal spasm, however I have tried a lot of other methods, and the chin is still the best.
First of all it fits perfectly in between the tips of the vertebrae, your neck is extremely strong, and allows perfect control over the amount of pressure you exert.
It also allows you the freedom of adjusting only those segments that are required to be done; most other methods are not specific enough, and often cause spasms in the adjacent spinal area.
Best of all, it allows both hands free to control the movement of the dog.
To adjust L1 to L6 Stand behind the dog with your feet slightly spread, bend over the rear of the dog and wrap one arm around the upper portion of the back legs the other around the hips.
Lift the back legs off the ground, and extend both legs out behind the dog, do this while bending over, and without lifting the rear of the dog any higher, so that the spine remains horizontal.
(Some greyhounds may resist having both back legs extended, this is generally caused by damage in either the TENSOR FACIA LATA or the top of the LATERAL VASTUS if this is the case both areas will have to be thoroughly massaged, prior to proceeding with the adjustment)
Place your chin between the segments to be adjusted, and using a firm downward and slightly rearward pressure with your chin, flex the spine downward.
This particular method will also allow you to rotate the spine very slightly, if extra pressure on either side of the spine is required.
However, as a normal rule the spine should be kept as straight as possible.
After massaging the spine, recheck the spinal area, and if not completely free, repeat the same adjustment.
This type of manipulation does not cause any trauma to the spine or the dog, nor does it compress the internal organs as with spinal rotation.
Spinal adjustment to L6 – S2 This section of the spine causes the most problems with the racing greyhound.
However, this area does not normally sustain injury or muscle spasm during the normal course of racing.
Generally, it is an injury or weakness first caused during the rearing of the greyhound, and sometimes simply because of the training methods employed by the trainer.
Damage, weakness or injury in this area of the spine is the result of the dog making a sudden and drastic change of direction at the end of a rearing yard, or a straight run.
It affects in particular those greyhounds that have spend a considerable amount of time as pups running up and down full speed, in a long narrow rearing yard.
It is the action of running to the end of a straight run, spinning hard to the left, and running back again repeatedly, that causes a massive muscle spasm on the left side of the 7th LUMBAR vertebrae.
In many cases severe enough to cause the tissue on the right side of the vertebrae to tear or weaken severely.
In the worst cases, when the spinning around at the end of a run involves sliding on a slippery surface, it may fracture the spinal section of the vertebrae.
Physical symptoms and effects of this injury listed in order of severity are:
1 No other symptoms other than the inability to extend one or both hind legs fully
2 The above + a reduction in the size of the left GLUTEUS MEDIUS
3 All of the above + a reduction in the size of the right GLUTEUS MEDIUS
4 All of the above + a reduction in the size of both the BICEPS FEMORIS muscles
5 All of the above + damaged tissue on the right hand side of L7 allowing fractional sideways movement of L7.
6 All of the above + a fractured spine of L7 capable of being pushed sideways both left and right.
To remove all the muscle spasms around the L6 – S2 area including some around the pelvic bone, a number of adjustments must be made, and in a specific order.
Firstly, the pelvic bone requires rotation, even though it is a relative simple procedure, it is rather difficult to describe in print.
Next is the adjustment of the tissue around the S2 – tail area, adjusted by rotating the tail.
Last but not least, the L5 – L6 and L6 – L7 junctions will require adjusting, simply because the first adjustment, the pelvic bone rotation, may cause muscle spasm to this area.
The extent to which you follow through on each adjustment will depend largely on the severity of the problem being adjusted, minimum muscle spasm minimum rotation, severe muscle spasm maximum rotation.
When adjusting L6 – S2 both sides of the body must be rotated, the side with the least problem being treated first
It is also unfortunate that much of this area is difficult to massage deep enough to make the adjustment easier on the dog, however 3 or 4 minutes with a hot towel just prior to the adjustment will help some.
Pelvic Rotation (with the worst problem on the right side of the dog) Stand on the left side facing the dog with your left leg (knee slightly bent) against the coupling- hip junction.
Bend over the dog bringing your left arm over, around and under the dog, placing your left hand on the outside of the dogs left knee.
At the same time, with your right hand reach over the dog picking up the right leg of the dog just below the tarsal bone, and bring the right leg over towards the left, and with your index finger between the two, grip both hocks firmly.
Lift both the hocks and knees, bringing them closer to the dog’s body as you lift.
At this point the dogs body will be resting on your left thigh, held there firmly by the back of your left arm; his back legs will be tucked close to him, and at a right angle to his body. Your right arm holding the hocks will be against the outside of the upper part of the dogs right hind leg, gripping the hocks.
With a smooth firm motion lift the knees up and towards the rear of the dog, while bringing the hocks slightly down with your right hand, and pressing down on the top of the hind leg-pelvic bone area with the inside of your right forearm.
Rotating far enough to bring the TIBIA part of the hind leg into an almost vertical position.
IMPORTANT: this rotation is mainly done by lifting the knee and pushing down on the pelvic area with the inside of the forearm, do not force the hocks downward, this will cause severe damage in the knee joints.
Extra pressure (if required) may be placed on the pelvic bone with the knee of your right leg during the rotation.
Do not hold at the furthest point of rotation, release immediately.
Tail rotation Prior to any tail rotation, grip the tail firmly approximately 200 mm down from the butt of the tail (not the end) and pull firmly downwards.
This is to free any spasms in the tail so you may use it as a lever to adjust the tail – S2 area.
Standing to the side of the hind leg of the dog (left hand side if you are right handed) place the ball of your thumb of your left hand approximately 5 cm to the front of the left crest of the ILIUM (pin bone). Press down firmly and slide the thumb to the rear of the dog between the pin bone and spine, stopping just 2 cm past the pin bone.
Grip the tail firmly approximately 400 mm down from the butt, and turn your wrist inward while bringing the tail up and around to the left.
Repeat the procedure in the opposite direction on the other side of the dog.
When completed, again pull the tail downwards firmly to remove any spasms.
Then use the procedure as described for the L1 to L6 ADJUSTMENT to adjust L5 – L6 and L6 – L7.
To remove the spasms around the L6 to S2 area, all of the adjustments must be done, and in the right order.
I realise the whole procedure when written down may appear difficult, and possibly hard on the dog, in particularly the pelvic rotation.
However if you did the pelvic rotation extremely gently and slowly on a perfectly sound dog, you may be surprised as to how far you can actually rotate this area, and not cause any discomfort.
L7 with damaged tissue on one side When the spasm to the L6 – S2 area is severe enough to have caused a weakness on one side of the L7 spinal segment (the spine of L7 can be moved sideways in one direction only), further action will have to be undertaken after doing all of the L6 – S2 adjustments.
You will find that after completing the manipulation that the L7 spine will have stabilised somewhat, and will feel a lot firmer, even so the weaker area will have to be injected with a sclerosing agent, (not an anti inflammatory) to increase the strength of the area.
It is unlikely that either “Muscle Repair” or “Promote” will be strong enough to do the job effectively, and the easiest available product that may help is 5% ETHANOL AMINE OLEATE (Merolin).
Inject 1 ml in 1/10th of a ml doses along an area in line with the spine 12 to 15 mm out from the centre of the spine of L7 to the full depth of a ½ inch needle.
Allow the area to settle for 7 days then recheck
After the spine has sustained this type of damage, it is imperative that the dog not be allowed free galloping in a small yard or enclosure, as the problem is likely to reoccur
L7 with suspected fractured spine When the L7 spine is capable of being moved sideways in both directions, it is likely that it has fractured. Use X ray to confirm, and in this situation surgical removal is the only option.
Additional adjustments that may have some benefit are those related to the joints of the limbs.
However, in each instance, they involve tendons and ligaments that have sustained damage, and inexperienced efforts to relieve the stiffness of the joint may cause further damage.
Anti-inflammatory creams or heat producing liniments, along with massage and gentle physiotherapy, are often a better alternative.
There are a large number of other “manipulations” that are practised on the racing greyhound, such as rolling shoulders, and putting back “cords” and tendons that have “slipped” out of position.
However, after 35 years of looking at the injuries sustained by the racing Greyhound, I still have yet to find a tendon or "cord" that has "slipped out of position" which could be replaced successfully by manipulation only.
In almost every instance of the often extremely painful to the Greyhound of “muscle manipulation” I have ever witnessed, the only real benefit has been a reduction in muscle spasm, possibly better treated with massage, liniment, Ultrasound treatment, or simply rest.
However, if you need instant results, firm-sliding pressure over a tendon and some stretching action will temporarily relieve adhesions due to damage in the tendon or ligaments, and may allow the Greyhound to perform.
Then again, I certainly don’t profess to know everything there is to know about manipulation, and if it works for your Greyhounds that’s great.
MUSCLE STRUCTURE
GENERAL MUSCLE STRUCTURE AND FUNCTION

- 1. SCUTULARIS – action: to move ears.
2. ZYGOMATICUS – action: to move top lip.
3. PAROTID GLAND
4. MASSETER – action: to raise lower jaw and close mouth.
5. MAXILLARIS – action: to move nose and lip.
6. NASALIS – action: to move nose.
7. WHISKER BED
8. BUCCINATOR – action: to move lip.
9. DIGASTRICUS – action: to depress the lower jaw and open mouth.
10. MYLO-HYOID – action: to support or raise the tongue.
11. STERNO-HYOID – action: involved in swallowing.
12. STERNO-THYROID – action: involved in swallowing.
13. THYROID GLAND
14. CEHALO-HUMERAL – action: to advance the limb or draw limb and head together.
15. MASTOIDEUS – action: to raise head or neck.
16. SPLENIUS – action: to extend or incline head.
17. JUGULAR VEIN
18. SERRATUS MAGNUS – action: to extend or turn the head.
19. ANGULARIS – action: to lift the lower end of the SCAPULA.
20. HUMERUS
21. ACROMION – action: to flex the shoulder joint
22. SCAPULAR DELTOID – action: to flex the shoulder joint and rotate the HUMERUS outward.
23. ACROMION DELTOID – action: as for SCAPULAR DELTOID.
24. CEHALO-HUMERAL – action: to advance the limb or draw limb and head together.
25. CEPHALIC VEIN
26. SPINE OF THE SCAPULA
27. UPPER TRAPEZIUS – action: to raise the shoulder or carry it forward.
28. LOWER TRAPEZIUS – action: as for UPPER TRAPEZIUS.
29. LATISSIMUS DORSI – action: supports the forelimb and carries the trunk forward.
30. INFRASPINATUS – action: to adduct the HUMERUS and rotate it outward.
31. GREAT OBLIQUE – action: to flex the spine, or incline it laterally.
32. RECTUS ABDOMINIS – action: the principal FLEXOR of the spine.
33. INTERCOSTALS – action: in breathing.
34. SCALENUS – action: to draw the shoulder backward.
35. PECTORALIS MINOR – action: to draw the shoulder downwards and backwards.
36. PECTORALIS MAJOR – action: to adduct, flex and rotate inwards the forelimb.
37. EPITROCHLEARIS – action: to draw the forelimb backwards.
38. FLEXOR CARPI ULNARIS – action: to flex the CARPUS and foot.
39. PERFORATUS – action: to flex the toes and the whole foot on the forearm.
40. ANCONEUS – action: to raise the capsule of the elbow joint.
41. FLEXOR CARPI RADIALIS – action: to flex the CARPUS on the forearm.
42. PRONATOR TERES – action: rotate the RADIUS and turn the paw downward and outward.
43. PERFORANS – action: to flex the toes and foot.
44. SUBCUTANEOUS VEIN
45. PISIFORM BONE
46. PLANTAR PADS
47. METACARPUS
48. LONG TRICEPS – action: to extend the forearm.
49. OUTER TRICEPS – action: to extend the forearm.
50. BRACHIALIS – action: to flex the forearm.
51. EXTENSOR CARPI RADIALIS – action: extends the METACARPUS on the forearm.
52. EXTENSOR DIGITORUM COMMUNIS – action: extends the toes and foot.
53. EXTENSOR DIGITORUM BREVIS – action: extends the three outer toes and foot.
54. EXTENSOR CARPI ULNARIS – action: to extend the CARPUS with slight outward rotation.
55. FLEXOR CARPI ULNARIS – action: to flex the CARPUS and foot.
56. EXTENSOR OBLIQUE – action: to extend the first toe (dewclaw).
57. ANNULAR LIGAMENT
58. CARPUS
59. PHALANGES
60. SUPRA SCAPULAR GLAND
61. 1st SARTORIUS – action: to adduct the leg and carry the thigh forward.
62. 2ND SARTORIUS – action: as above.
63. VASTUS INTERNUS – action: to extend the leg.
64. ADDUCTOR MAGNUS – action: to adduct and rotate the thigh outwards, push body forward.
65. SEMIMEMBRANOSUS – action: to extend the thigh and flex the knee.
66. GRACILIS – action: to adduct the thigh.
67. SEMITENDINOSUS – action: draws back the thigh and pushes body forward.
68. GASTROCNEMIUS – action: to extend the foot on the TIBIA.
69. POPLITEUS – action: to rotate the TIBIA sideways and outward.
70. PERFORATUS – action: to flex the toes, draw the foot back, and bend the knee.
71. PERFORANS – action: to flex the toes and draw the foot backwards.
72. PERFORANS AUXILIARY – action: to flex the toes.
73. TIBIALIS ANTICUS – action: to bend the foot forward and upward.
74. LUMBO DORSAL FASCIA – action: to assist in spinal flexion.
75. CREST OF ILIUM
76. LONG TENSOR FASCIA – action: to flex the thigh.
77. SHORT TENSOR FASCIA – action: to flex the thigh.
78. GLUTEUS MEDIUS – action: to extend, rotate or adduct the thigh.
79. GLUTEUS MAXIMUS – action: to adduct the thigh and rotate the knee outward.
80. GREAT TROCHANTER – action: muscle insertion point (GLUTEUS).
81. ISCHIUM – action: insertion point for GEMELLUS – action: to carry the thigh forward.
82. SEMIMEMBRANOSUS – action: to extend the thigh and to flex the knee.
83. ERECTOR – action: to raise the tail.
84. CURVATOR – action: to draw the tail sideways and upward.
85. FASCIA LATA – action: to flex the thigh.
86. SEMITENDINOSUS – action: flex the knee, draw back the thigh and push body forward.
87. BICEPS FEMORIS – action: flexes the leg, when leg is fixed it rotates the PELVIS.
88. DEPRESSOR – action: to depress the tail.
89. GASTROCNEMIUS – action: to extend the foot on the TIBIA.
90. GREAT SAPHENOUS VEIN
91. PERFORATUS – action: to flex the toes, draws back the foot and bend the knee.
92. PERFORANS – action: to flex the toes and draw the foot backward.
93. CALCANEUM
94. TARSUS
95. METATARSUS
96. TIBIALIS ANTERIOR – action: to flex or rotate the foot.
97. EXTENSOR PEDIS – action: to extend the toes and draw the foot forward.
98. LONG PERONEUS – action: to turn the lower end of limb outwards.
99. SHORT EXTENSOR – action: to extend the toes.
100. PHALANGES
BONE STRUCTURE
BONE STRUCTURE
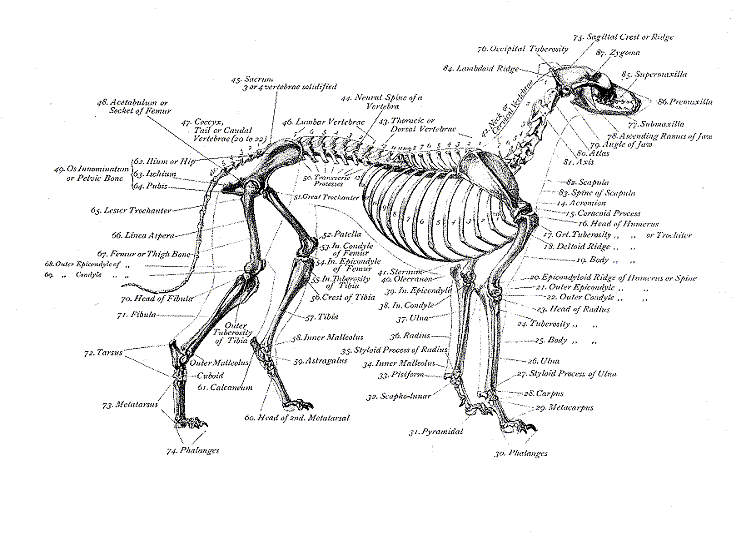
INNER SIDE OF LIMBS
INNER SIDE OF LEFT FRONT LEG
& LEFT HIND LEG
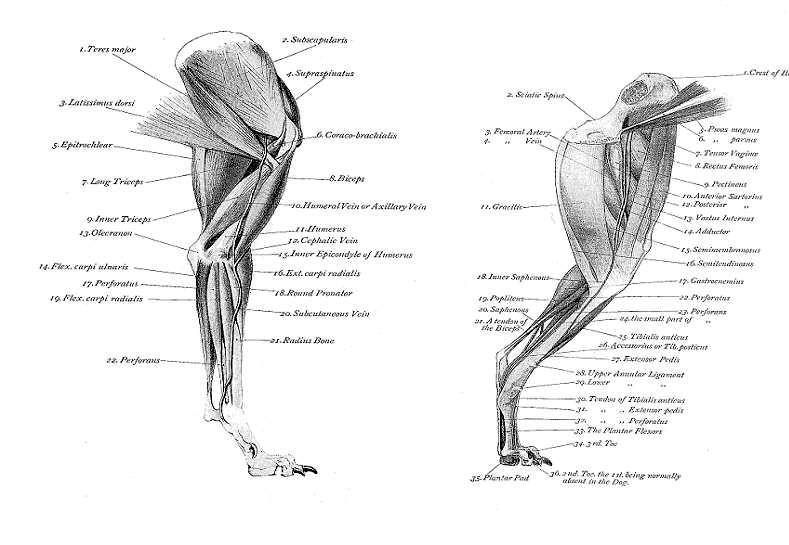
L/H Side: INNER SIDE OF LEFT FRONT LEG-
MUSCLE STRUCTURE AND FUNCTION
1. TERES MAJOR – action: to flex the shoulder joint and draw the forearm back.
2. SUBSCAPULARIS – action: to extend the shoulder joint and push arm forward.
3. LATISSIMUS DORSI – action: supports the arm and carries the trunk forward.
4. SUPRASPINATUS – action: extends the HUMERUS.
5. EPITROCHLEARIS – action: to draw the arm backwards and aid the TRICEPS.
6. CORACO-BRACHIALIS – action: to advance the arm-rotate inwards-extend shoulder joint.
7. LONG TRICEPS – action: to extend the forearm.
8. BICEPS – action: to flex the forearm.
9. INNER TRICEPS – action: to extend the forearm.
10. HUMERAL VEIN
11. HUMERUS
12. CEPHALIC VEIN
13. OLECRANON
14. FLEXOR CARPI ULNARIS – action: to flex the CARPUS and foot.
15. INNER EPICONDYLE OF HUMERUS
16. EXTENSOR CARPI RADIALIS – action: to extend the METACARPUS on the forearm.
17. PERFORATUS – action: to flex the toes and the whole foot on the forearm.
18. ROUND PRONATOR – action: to turn paw downward and outward by rotating the RADIUS.
19. FLEXOR CARPI RADIALIS – action: to flex the CARPUS on the forearm.
20. SUBCUTANEOUS VEIN
21. RADIUS
22. PERFORANS – action: to flex the toes and foot
1. CREST OF ILIUM
2. SCIATIC SPINE
3. FEMORAL ARTERY
4. FEMORAL VEIN
5. PSOAS MAGNUS – action: to flex and rotate the thigh and incline the lumbar region laterally.
6. PSOAS PARVUS – action: to flex the pelvis on the spine.
7. TENSOR VAGINA – action: to flex the thigh and tense its muscle sheath.
8. RECTUS FEMORIS – part of the QUADRICEPS – action: to extend the leg.
9. PECTINEUS – action: to flex, adduct, and rotate inward the FEMUR.
10. ANTERIOR SARTORIUS – action: to adduct the leg and carry the thigh forward.
11. GRACILIS – action: to adduct the thigh.
12. POSTERIOR SARTORIUS – action: to adduct the leg and carry the thigh forward.
13. VASTUS INTERNUS – action: to extend the leg.
14. ADDUCTOR – action: to adduct and rotate the thigh outwards and push the body forward.
15. SEMIMEMBRANOSUS – action: to extend the thigh and flex the knee.
16. SEMITENDINOSUS – action: draws back the thigh and pushes the body forward.
17. GASTROCNEMIUS – action: to extend the foot on the TIBIA.
18. INNER SAPHENOUS VEIN
19. POPLITEUS – action: to rotate the TIBIA sideways and outward.
20. SAPHENOUS VEIN
21. TENDON OF THE BICEPS
22. PERFORATUS – action: to flex the toes, draws back the foot and bend the knee.
23. PERFORANS – action: to flex the toes and draw the foot backwards.
24. SMALL PART OF PERFORANS
25. TIBIALIS ANTICUS – action: to bend the foot forward and upward.
26. FLEXOR ACCESSORIUS – action: to flex or rotate the foot.
27. EXTENSOR PEDIS – action: to extend the toes and draw the foot forward.
28. UPPER ANNULAR LIGAMENT
29. LOWER ANNULAR LIGAMENT
30. TENDON OF TIBIALIS ANTICUS
31. TENDON OF EXTENSOR PEDIS
32. TENDON OF PERFORATUS
LEFT FRONT FOOT
THE BONES, TENDONS, AND LIGAMENTS
OF THE LEFT FRONT FOOT

LEFT HIND FOOT
THE BONES, TENDONS, AND LIGAMENTS
OF THE LEFT HIND FOOT
